Research may soon lead to better therapies for itching and acne
The sensation flutters across your back like a butterfly and crawls up your neck like a spider, provoking an irresistible urge to scratch. For most of us, an itch ends there, but thousands of unlucky people continue to suffer for days, months or even years with only momentary relief.
"Pain? That is easy to deal with, my patients often tell me. But itching kills you," says Paul Bigliardi, a clinical dermatologist, allergist and immunologist at the A*STAR Institute of Medical Biology (IMB) and National University Hospital in Singapore. For more than a decade Bigliardi has been treating patients with chronic and intractable itching, and has recently unearthed surprising findings that may lead to more effective treatments.
Patients with severe cases of itching, says Bigliardi, have difficulty concentrating and sleeping. "They scratch their skin away and wake up from a very bad night's sleep with blood all over their sheets and pajamas and scratch marks on their bodies."
Itching is just one of the many skin conditions being studied by researchers at the IMB.
Scratching the surface
Chronic itching manifests in a broad range of disorders, including kidney and liver failure, diabetes, HIV infection, eczema and psoriasis, autoimmune diseases, cancers and allergies. "As a result, no single discipline feels responsible for studying the itch," says Bigliardi, "which makes finding effective treatments very difficult."
Furthermore, itch, like pain, is very subjective, so studying animal models is of limited use. "You cannot ask a mouse if it feels a burning or an itching sensation. You need human subjects." Objective methods for measuring exactly how itchy a person actually feels need to be improved.
Despite these challenges, recent advances in deciphering biological processes in the peripheral and central nervous systems have improved our understanding of the distinct itch pathway. An itch usually originates from the skin, induced by various mechanical, chemical, infectious or inflammatory triggers, and is then transmitted via the peripheral nervous system to the central nervous system. Less frequently an itch originates directly in the peripheral and central nervous systems. Neurologic and psychiatric disorders can further aggravate the sensation.
In 2007, Bigliardi revealed a clear link between itching and two types of opioid receptors expressed in skin cells. Mice lacking these receptors scratched less than normal mice when a chronic inflammatory skin condition was induced. Many researchers thought that opioid-induced itching was derived solely from the central nervous system, until Bigliardi's results proved otherwise. In clinical studies on patients with severe, chronic itching, he found that applying a cream containing a molecule called methylnaltrexone that inhibits opioid-receptor activity by preventing molecules from binding to the receptors halved itching intensity nearly 30 minutes faster than in patients who used a soothing moisturizer alone. Importantly, methylnaltrexone does not cross the blood–brain barrier and is selective to peripheral opioid receptors. "This was an entirely new concept; that sensations like itch and pain could also be influenced from the periphery, not just from the central nervous system."
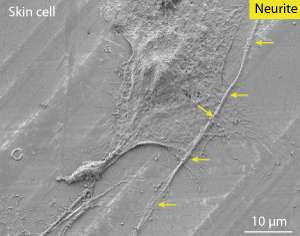
The Experimental Dermatology Laboratory at the IMB, which Bigliardi heads, is building on this discovery by developing the first cellular model for studying the interaction between skin cells and nerve cells by growing them in the same Petri dish (see image). They plan to test different compounds on the co-culture to better understand how signals are transferred from the skin cells to the nervous system.
Bigliardi is also the director of the Clinical Research Unit for Skin, Allergy and Regeneration (CRUSAR) at the IMB, which started its first clinical trial in June 2015 and will be a comprehensive testing ground for theories, strategies and devices to diagnose and treat skin disorders like itching and acne, as well as wound healing and allergy.
Acne lab
Acne, like itching, remains a puzzle to researchers. While mild acne usually resolves spontaneously, severe conditions require medical intervention and can lead to scarring or disfigurement.
Poor understanding of why acne develops has yielded a lack of effective drugs to treat it. These must be taken for a long time and have potentially severe side effects. Maurice van Steensel, a dermatologist and molecular geneticist at A*STAR, is studying a genetic pathway associated with acne that might offer a direct route to a new class of drugs for treating the skin condition. "It has the potential to be the biggest breakthrough in the field and could change our understanding of acne entirely," he says. Van Steensel heads the IMB's Acne Lab, which was established in 2013 as part of the Skin Research Institute of Singapore.
The long accepted cause of acne begins with the excess production of keratin—a protein that makes up skin, hair and nails. Hormonal changes during puberty or a genetic predisposition can exacerbate this process. The keratin accumulates inside hair follicles and eventually blocks the secretion of an oily lubricant called sebum from the sebaceous glands. The clogged follicles then form comedones—either whiteheads (covered by skin) or blackheads (not covered by skin). Comedones are vulnerable to infection by the bacteria Propionibacterium acnes, leading to inflammation and the formation of pimples.
Van Steensel's research suggests this model is flawed and that keratin accumulation is not a cause but rather a consequence of other events potentially linked to genetic factors that lead to comedo formation.
Research informed by the prevailing model has not produced a new class of acne drugs in two decades. Furthermore, researchers are increasingly uncertain about the role of P. acnes in acne. Animal models used, such as hypersensitive rabbit ears or the hairless rhino mouse with its nude drapery of skin, are poor substitutes for human skin.
Instead, van Steensel studies ultra-rare genetic skin disorders that can point to specific genes and pathways involved in acne and could be targeted for treatment.
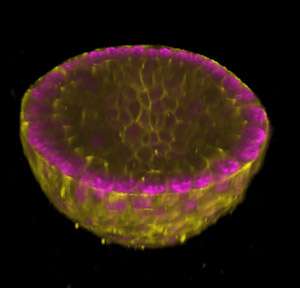
Just before joining A*STAR, he discovered genetic mutations associated with a progressive disorder characterized by severe acne called Borrone dermatocardioskeletal syndrome. "Acne follows if the pathway that the Borrone genes are in is dysfunctional," says van Steensel. The Acne Lab is studying the effect of these genes on cell growth using three-dimensional models (see image). They are also developing zebrafish models of the disease, as well as skin cells such as fibroblasts with the acne genes mutated. They plan to use these models to test for compounds that can correct abnormal cellular behavior. "By focusing on libraries of drugs already in clinical use for other disorders, we have a very quick path to the clinic."
The lab is also collaborating with another principal investigator at the IMB, Xinhong Lim, and Procter & Gamble to study sebaceous gland development. This joint venture is called the Sebaceous Gland Lab, and has already provided insights and tools for cosmetics development. Prescription drugs for acne make up a USD 2.5 billion industry worldwide, with hundreds of millions more spent on over-the-counter lotions, creams and scrubs. Research at the IMB is drawing medication and cosmetic markets closer together.
"There are a lot of converging interests in Singapore and a very collegial spirit at A*STAR," says van Steensel. "Sharing space with top-notch scientists and state-of-the-art facilities has proved to be very beneficial."