An exercise approach to cystic fibrosis
We can't change our genes – yet – but we can alter our environments to ease life with an inherited illness. Meet two young people whose love of dance, running, yoga, and more is helping them live with cystic fibrosis (CF).
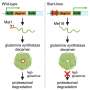
Mikayla Polski of Minnesota and Evan Scully of Ireland are "double deltas" – they have two copies of the delta F 508 mutation in the CFTR gene. Neither takes the drug Kalydeco that has helped many people with the disease.
Mikayla's Story

I first spoke with Donna Polski, Mikayla's mom, while writing the first edition of Human Genetics: The Basics (not a textbook). For the second edition, I recently spoke with Donna again, after following Mikayla's progress through Facebook. At age 13, she's edging closer to her dream of becoming a professional dancer.
The Polskis knew their daughter had CF before she was born, thanks to an astute genetic counselor who suggested testing for the common CFTR mutations along with amniocentesis when learning of the couple's northern European background – this was years before prenatal screening for the disease became routine.
When an ultrasound exam revealed intestinal blockage, Mikayla was delivered early and due to complications of the surgery that happened on her first day, she spent her first month in the NICU. During her early childhood, hospitalizations for lung infections peppered the daily grind of bronchial drainage treatments.
Evan Scully's parents came up with a great analogy for these exercises that parents typically perform on their young children. "CF is like a ketchup bottle. The ketchup won't come out unless you turn it upside down and belt the bottom of it until it comes out. It's like CF. If you don't do anything with your lungs, the "ketchup" is just going to stay in your lungs," Evan recalls. Mikayla replaced the ketchup bottle routine with a vibrating vest at 16 months, something Evan has used too.
But the most important thing to happen to Mikayla was when she saw a ballerina in a cartoon. "So we enrolled her in dance class. She just lit up – she loved it!" says Donna.
"I was 2 or 3 when I first started dancing," Mikayla told me last week. "I do tap, jazz, ballet, and some other stuff. I like it because if I'm having a bad day, I can dance and it's a way to communicate without having words."
It must have been a tough decision for her parents, who knew the dangers of exposure to infections that wouldn't threaten youngsters who don't have cystic fibrosis. "But we did it to get her out around other kids, because she needed the peer interaction. Never did I think dance would become her passion. Some people never know what their passion is. I can't imagine her without dance," says Donna.
During flu season Mikayla has to move some of her practice to a big screen at home. At other times, she can sometimes fit in two sessions a day, right after school and again at night – all the while maintaining the daily treatments and medications to manage the disease that won't stop her.
Although Mikayla still takes many drugs to keep her lungs clear, Donna credits her daughter's high activity level with at least one bit of good news: preventing diabetes. Some people with CF develop a special type of diabetes that happens when the hallmark sticky secretions plug up the pancreatic islets, mimicking type 1, but also has some aspects of insulin resistance, like type 2. Exercise and diet are not expected to help much with the CF version, but it helped Mikayla – perhaps because she was actually on the road to type 2, Donna says some physicians have speculated.
When Mikayla's glucose tolerance test came back high, "we changed the way she was eating, cutting back on sugar, adding protein, right about when she started dancing competitively," Donna recalls. Her blood glucose level went from hovering at the diabetes mark down to 128 mg/dL two hours after eating – normal.
Mikayla wants to one day move to New York City or LA to dance in musicals. I expect to see her on Broadway!
Evan's Story

When Evan Scully was born in 1986, doctors told his parents he wouldn't live past age 10. "I was symptomatic from birth, but I was diagnosed at 6 months old. I wasn't thriving, I was coughing, and I couldn't keep anything in me for long enough. But obviously they were wrong." He's never even been hospitalized.
Evan's website chronicles his lifelong effort to compensate for what nature gave him with attention to diet and exercise. His medication list has shrunk over the past 4 years as his lung function has risen.
Evan credits his health as well as his career as a sports therapist to his parents' mantra of listening to the body. He shares some tips.
He eats vegetarian during the week and meat at weekends. "I do a 3-day exercise cycle – about an hour running on day 1, gym workout on day 2, and yoga and movement on day 3." When he was running competitively for Ireland, he did 120 miles a week! Still, Evan must be vigilant at keeping up his medical routine, including daily airway clearance procedures.
Like Mikayla, Evan is prone to infection. In 2015 he contracted Pseudomonas, Staphylococcus, and Candida infections simultaneously. That followed a grueling multi-city trek with an Olympic athlete that also exposed him to air-conditioning and didn't leave him enough time for his own exercise or the daily airway clearance protocols. A lapse like that can spell disaster.
The drugs to treat the infections wiped him out. "But I started doing everything possible to clear it because I had a feeling I was on my way to hospital for the first time. I knew I needed to get back out there. My first run back was 1 mile. It took me 12 minutes and I was dying doing it!!!" Soon, though, he broke 40 minutes in a 10-kilometer run, his goal.
Evan explains the logic. "Because I don't let mucus lay in my body, it doesn't give the infections mucus to house in. My parents would have said, 'infection can't grow if there is no mucus there.' It makes sense. So a lot of it is down to mental strength and positivity."
Caveats
I'm not an MD so this post isn't meant to offer medical advice. And Mikayla's and Evan's experiences may lie within the natural history of the disease. But if exercise – dance, yoga, running, anything – is not dangerous for a particular individual and can increase aerobic capacity while boosting self-esteem and fostering social relationships, then I think that is every bit as valuable to a patient's well-being as the most targeted of molecular therapies.
This story is republished courtesy of PLOS Blogs: blogs.plos.org.