New UN treatment targets for HIV/AIDS would be 'expensive but worth every penny'
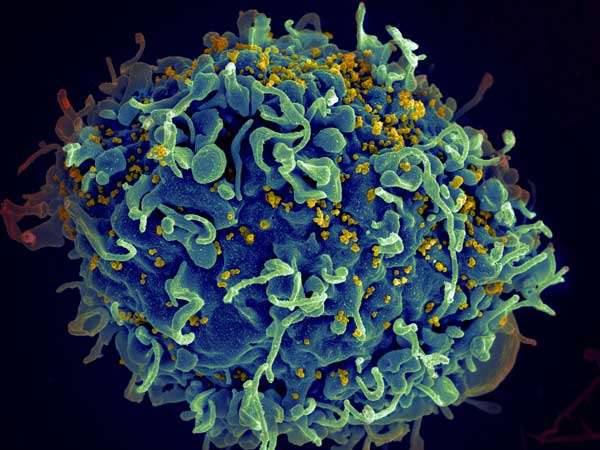
A new study finds that implementing the United Nations targets for HIV testing and treatment would be an expensive but ultimately very cost-effective way to increase survival, reduce the number of children orphaned by HIV, and contain the global AIDS epidemic. That is the conclusion of researchers at the Massachusetts General Hospital (MGH), the University of Cape Town and the Yale School of Public Health, who estimated the likely impact of the so-called "90-90-90" program.
"Based on our findings, there is nothing overstated about the suggestion that 90-90-90 could lay the foundation for a healthier, more just and equitable world for future generations," says Rochelle P. Walensky, MD, MPH, of the MGH Division of Infectious Disease, who led the study that will appear in the May 31 online edition of Annals of Internal Medicine. "Yes it would be very expensive, but it would be worth every penny."
Launched in September 2014 by the Joint United Nations Programme on HIV/AIDS (UNAIDS), the 90-90-90 program has three key objectives - diagnosing 90 percent of HIV-infected persons worldwide; linking 90 percent of identified cases to antiretroviral therapy (ART); and achieving virologic suppression among 90 percent of ART recipients. The program's overall goal is achieving viral suppression - reducing the viral load to an undetectable level - among 73 percent of HIV-infected persons worldwide by 2020, a marked improvement from current estimates of 24 percent.
Critics have expressed concern that successful implementation of 90-90-90 would require unprecedented cash infusions from donor organizations such as the President's Emergency Plan for AIDS Relief, the Global Fund, and the World Bank. Study co-author Linda-Gail Bekker, MD, PhD, of the Desmond Tutu HIV Centre and University of Cape Town in South Africa, notes, "Recent funding from these sources has been flat. Our goal for this study was to provide donors and partner countries with pragmatic estimates of what it will cost and what return they can expect by investing in 90-90-90."
The study used South African epidemiologic data and results from HIV screening and treatment programs to give a realistic picture of the likely impact of 90-90-90 in South Africa and compared it with the current pace of HIV detection and treatment over the next 5 and 10 years. Using a well-published computer simulation model developed by the research team, their analysis revealed that, over the next decade, the 90-90-90 strategy would avert more than 2 million new HIV infections, more than 2.4 million deaths and over 1.6 million orphans - saving an additional 13 million patient-years of life compared with the current strategy.
Over the same period, the cost of the 90-90-90 effort would be $54 billion, a 42 percent increase over the costs of current scale-up activities that still suffer from challenges related to both linkage to care and treatment retention. But taken as a whole, the study found that investment in 90-90-90 would yield a cost-effectiveness ratio of $1,260 per year of life saved, well within what would be considered very cost effective for South Africa and a ratio similar to that of HIV treatment itself.
A. David Paltiel, MBA, PhD, professor of Public Health (Health Policy) at the Yale School of Public Health and senior author of the study, says, "We're convinced, based on the results of our analysis, that successful implementation of the 90-90-90 targets would effectively put an end to the AIDS epidemic worldwide,"
Publication of the study coincides with a June 8-10 United Nations meeting of world leaders, HIV program implementers, government representatives and other key stakeholders to solidify a plan to put an end to the global AIDS epidemic by 2030. "Implementation of 90-90-90 would represent a 'virtuous circle' of care - leading to earlier HIV diagnosis, more rapid treatment initiation, longer survival for HIV-infected persons, and fewer new cases of HIV transmission," says Walensky, a professor of Medicine at Harvard Medical School. "The time to jump-start this worthy global undertaking is now."
More information: Annals of Internal Medicine, DOI: 10.7326/M16-0799