Ischemic stroke therapy – does the gut microbiota hold the key?
As the world's population grows older, the burden of stroke continues to increase. Epidemiological data indicates that around 17 million people suffer a stroke each year, making it the second leading cause of death in the world and a major source of disability.
The incidence of ischemic stroke (occurring due to loss of blood supply to the brain) in young adults is also increasing, almost doubling since the 1990s; epidemiological projections estimate that the total worldwide number of ischemic stroke survivors may rise to 77 million people by 2030. Post-stroke complications are frequent and include motor deficits, dementia, depression, or fatigue, for example.
Despite major advances in knowledge of the pathophysiology of stroke, effective therapeutic options for ischemic stroke are still fairly limited. Research has shown that inflammation is a key component in the pathophysiological mechanisms of cerebral ischemia and that immune responses seem to play important roles in the primary and secondary progression of ischemic lesions, as well as in their repair and recovery, thus having a vital impact on the overall post-stroke outcome.
Immune and inflammatory mechanisms are now being explored as potential therapeutic targets, but there is still a lot to be understood about their roles in the pathophysiology of ischemic stroke until new and effective therapeutic strategies arise. Given its increasingly acknowledged role in the modulation of systemic immune and inflammatory responses, the gut microbiota has become a particularly engaging research subject.
The immune system, the gut microbiota, and the brain
The interaction with our commensal microbes is essential for the development, maintenance, and function of our immune system. But the gut microbiota may also be a key regulator of brain function through the gut-brain axis. As research on this field blooms, the gut microbiota is impressively gaining awareness as a central regulator of many neurophysiological functions due to its ability to influence the brain's chemistry through the release of neuroactive molecules and through modulation of immunological and inflammatory responses.
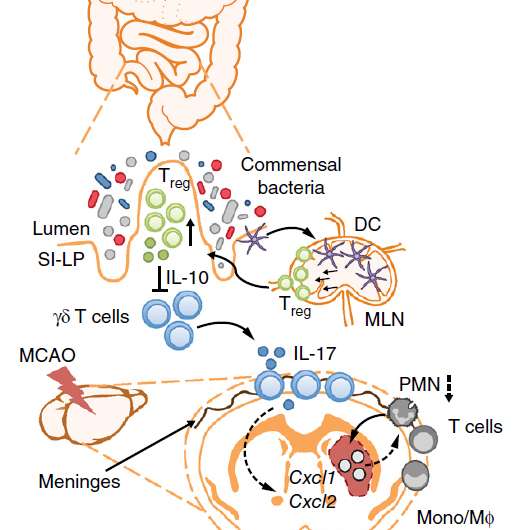
Through their interaction with the immune system, intestinal microbes have emerged as key regulators of lymphocyte populations, including regulatory T (Treg) and effector γδ T cells, both known to be involved in cerebral ischemic injury. γδ T cells are known to be able to exacerbate ischemic brain injury by secreting IL-17 and generating chemotactic signals for other immune cells; Treg cells, on the other hand, can contribute to neuroprotection by decreasing post-ischemic inflammation and increasing the secretion of the anti-inflammatory cytokine IL-10. Treg cells may modulate the peripheral immune system rather than directly act on the brain, and can maintain an anti-inflammatory environment in the gut by suppressing the proliferation of γδ T cells.
With these premises in mind, a new study recently published in Nature Medicine aimed at determining the effects of an altered intestinal microbiota on the immune system and on the outcome of cerebral ischemia. The results were groundbreaking – the study describes a new microbiota-gut-brain axis pathway with a potential impact on the outcome of ischemic stroke.
The gut microbiota may dictate stroke outcome
Using two groups of mice – a group sensitive to antibiotic treatment with amoxicillin–clavulanic acid, and a group resistant to the same antibiotic treatment – it was shown that antibiotic-induced alterations in the intestinal microbiota (dysbiosis) can reduce ischemic brain injury in mice. Causing an intestinal microbial imbalance altered immune homeostasis in the small intestine, leading to an increase in neuroprotective Treg cells and a reduction in detrimental IL-17-producing γδ T cells.
But the most impressive finding of this study was that there is trafficking of intestinal T cells to the meninges; intestinal T cells were known to traffic to extra-intestinal lymph nodes and to the spleen, but the new data presented in this study now shows that, after stroke, intestinal T cells can preferentially accumulate in the meninges as opposed to the cervical lymph nodes, suggesting a specific mechanism of gut-brain trafficking.
So, according to this study, in a normal gut microbial environment, after stroke there is a trafficking of IL-17+ γδ T cells from the gut to the leptomeninges, where they enhance ischemic neuroinflammation by secreting IL-17; this then leads to an increased production of chemokines in the brain and to the subsequent infiltration of cytotoxic immune cells.
Treg cells can inhibit the differentiation and proliferation of IL-17+ γδ T cells by secreting the anti-inflammatory cytokine IL-10. However, this ability is more efficiently achieved in mice treated with antibiotics, indicating that antibiotic-induced alterations in the intestinal microbiota can potentiate the neuroprotective effect of Treg cells.
Since the levels of Treg cells were increased in the small intestine but not in the meninges (nor in the colon, peripheral blood, spleen or lymph nodes of antibiotic-treated mice), changes in the bacterial composition in the small intestine are most likely accountable for this effect.
Treg cells may therefore affect stroke outcome through an intestinal mechanism involving IL-17+ γδ T cell suppression. Indeed, fewer IL-17+ γδ T cells were found in the meninges after stroke in mice with intestinal dysbiosis, and this was associated with reduced IL-17–responsive chemokine expression in the brain, indicating that antibiotic treatment suppressed the trafficking of effector IL-17+ γδ T cells from the gut to the leptomeninges after stroke.
Similarly to the effect observed on Treg cells, antibiotic treatment rendered dendritic cells isolated from the mesenteric lymph nodes more efficient in inducing Treg cells proliferation than those isolated from mice resistant to antibiotic treatment, whereas their inhibitory effect on IL-17+ γδ T cell proliferation was less marked. This suggested that dendritic cells induce the proliferation of Treg cells, which in turn suppress the proliferation of IL-17+ γδ T cells through the action of IL-10.
Therefore, a suppression of effector IL-17+ γδ T cell function by Treg cells can be achieved by modulating the activity of intestinal dendritic cells though the induction of dysbiosis with antibiotic treatment. However, the bacterial species responsible for these protective effects of dysbiosis remain to be identified.
These findings thus unraveled a previously unknown gut-brain axis pathway and once again highlight the impact of the gut microbiota on the brain, in this case, on the outcome of ischemic brain injury. Importantly, these findings fit those from studies on human stroke: infiltration of γδ T cells and secretion of IL-17 have also been reported in ischemic human brain tissue, as well as increased levels of circulating IL-17 in stroke patients.
This research may open a new avenue for potential therapies for ischemic stroke.
More information: Y. Béjot et al. Epidemiology of stroke and transient ischemic attacks: Current knowledge and perspectives, Revue Neurologique (2016). DOI: 10.1016/j.neurol.2015.07.013
Corinne Benakis et al. Commensal microbiota affects ischemic stroke outcome by regulating intestinal γδ T cells, Nature Medicine (2016). DOI: 10.1038/nm.4068
Daniel Erny et al. Host microbiota constantly control maturation and function of microglia in the CNS, Nature Neuroscience (2015). DOI: 10.1038/nn.4030 M.
Gelderblom et al. Neutralization of the IL-17 axis diminishes neutrophil invasion and protects from ischemic stroke, Blood (2012). DOI: 10.1182/blood-2012-02-412726
Costantino Iadecola et al. The immunology of stroke: from mechanisms to translation, Nature Medicine (2011). DOI: 10.1038/nm.2399 Sung-Gyoo
Park et al. T Regulatory Cells Maintain Intestinal Homeostasis by Suppressing γδ T Cells, Immunity (2010). DOI: 10.1016/j.immuni.2010.10.014
This story is republished courtesy of PLOS Blogs: blogs.plos.org.