Researchers find proliferating cells in normal and diseased corneal endothelium
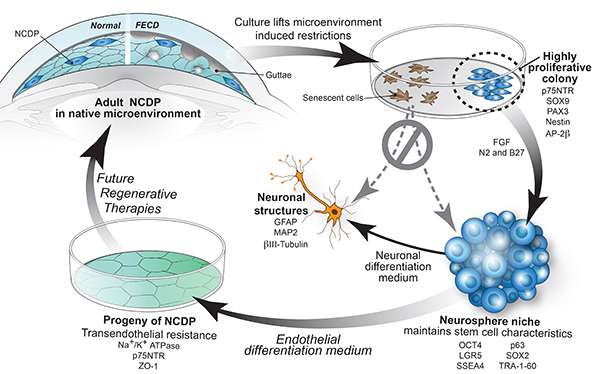
Researchers from Massachusetts Eye and Ear have, for the first time, identified rapidly proliferating cells (known as "neural crest-derived progenitor cells") in the corneal endothelium of specimens from normal corneas and from corneas with Fuchs' Endothelial Corneal Dystrophy (FECD), a condition in which the cells responsible for keeping the cornea clear die prematurely—often leading to blindness. The findings, published today in the American Journal of Pathology, hold promise for new therapies to be developed using the proliferating cells to return normal clearing abilities to the cornea in patients with FECD.
"Previously, we thought that all of the cells in the corneal endothelium were unable to divide, but we were surprised to find this small population of dormant stem cells capable of proliferating," said principal investigator Ula Jurkunas, M.D., a corneal and refractive surgeon at Massachusetts Eye and Ear and Associate Professor of Ophthalmology at Harvard Medical School. "We showed with various markers that they are progenitor cells. In addition, we were able to differentiate these cells into neurons— and that's a characteristic of all neural crest-derived tissue and its progenitors"
The corneal endothelium is responsible for pumping water throughout the cornea to keep vision clear, and when cells of the corneal endothelium die, they do not regenerate. Accelerated cell loss in patients with FECD prevents clearing of the cornea, and if left untreated, may progress to blindness. An age-related and genetic eye disease, FECD is one of the most common causes of corneal swelling. It affects up to four percent of the American population over the age of 40, and it is becoming more prevalent in women.
Full or partial corneal transplants are the most often recommended course of treatment to restore lost vision in patients with FECD. However, a few clinical studies have shown that, by stripping away a central portion of the diseased cells, the surrounding cells can grow in to clear the cornea. The proliferating cells described in the American Journal of Pathology paper may explain why this method, known as Descemet-stripping, has been successful in some patients.
Additionally, the newly described proliferating cells hold the promise of being able to regenerate a person's own endothelial cells, even in cases of FECD, as an alternative to transplanting corneas from a donor. The findings may change the clinical approach to patients with FECD, who are currently being treated as being irreversibly damaged, requiring transplants to provide a new source of healthy cells.
"Our research shows that some cells in Fuchs' dystrophy are still healthy, and that means that we could potentially stimulate them to divide and regenerate the corneas in a diseased state," said Dr. Jurkunas.
More information: Existence of Neural Crest–Derived Progenitor Cells in Normal and Fuchs Endothelial Dystrophy Corneal Endothelium, dx.doi.org/10.1016/j.ajpath.2016.06.011 , ajp.amjpathol.org/article/S000 … (16)30238-3/fulltext















