New findings on prostate cancer screening

The prostate-specific antigen test for prostate cancer was developed in the 1990s, quickly followed by an explosion of PSA screening for the disease and a further explosion of treatment. Treatment consists of either radiation or surgical removal of the prostate. The treatments have hard-to-live-with side effects such as urinary and bowel incontinence and loss of sexual function.
Yet the disease itself is often not particularly life-threatening. It's a truism that most men diagnosed with prostate cancer will die of something else first. Experts grew alarmed at the rush to treatment, much of which was likely to injure patients without extending their lives. They began arguing against routine PSA screening, especially mass screening.
Now there is strong evidence that watchful waiting is a reasonable approach for most men with prostate cancer. British scientists studied more than 1600 men for 10 years. The men had been randomized into groups that had surgery or radiation or underwent only "active monitoring." Most of the men survived no matter which group they belonged to.
"Active monitoring" does not mean ignoring a diagnosed prostate cancer or taking no action. It includes regular blood testing and clinical follow-up so a patient can move on to treatment if his cancer is growing.
"While the study provided some of the longest follow-up in prostate cancer research to date, a decade remains a fairly limited window," Laura Newman said at Undark. She noted that more study is needed to know for sure whether the therapies extend lifespan.
Some of the treatment effects reported in two papers that appeared in the New England Journal of Medicine last week: neither radiation therapy nor active monitoring lead to urinary incontinence; surgery often does. Neither surgery nor active monitoring lead to bowel problems; radiation often does.
Only 1% of subjects in the study died of prostate cancer, a lower-than-expected rate. The lead investigator told Newman, "With an equivalent and extremely low ten-year death rate no matter what you do, you can think very carefully before you choose what to do."
HealthNewsReview was pleasantly surprised at the quality of the reporting on the new study. Joy Victory concluded, "overall solid." Robust sourcing, level-headed patient anecdotes, and accurately described findings were the norm, she said.
But she also had complaints. Some stories stressed relative risks rather than the preferred absolute numbers. The cancer spread twice as often in the monitoring-only group, but the number of patients affected was low (33 out of 545 compared with 13/553 who had surgery and 16/545 who had radiation.) And none of the stories examined the costs of surgery and radiation or compared them with active monitoring.
Prostate cancer soars, surges, and skyrockets?
Prostate cancer has been much discussed of late. In July, the media were reporting that metastatic prostate cancer is "soaring," "surging" and "skyrocketing." This time HealthNewsReview bemoaned the quality of reporting.
Some accounts blamed the apparent increase in advanced prostate cancers on reduced PSA screening, but Kevin Lomangino noted that these claims came from well-known partisans of screening. He traced the alarmist reporting to an alarmist press release from Northwestern, home base for the paper's authors.
He also quoted an American Cancer Society rebuttal, noting that the increase was in raw number of cases, not in the rate of prostate cancer. A numerical increase in cancer can be due to an increase in population size and/or to an aging population, where the disease is more common.
Lomangino linked to a post at The Debunker, where Denise Grady suggested that another reason for the apparent increase might be improvements in diagnostic technology via magnetic resonance imaging. In short, maybe docs are getting better at finding prostate cancer.
She wrote, "the frightening news appears to be a false alarm—the product of a study questioned by other researchers but promoted with an incendiary news release and initially reported by some news media with little or no analysis from outside experts."
Incidental Economist Aaron Carroll despaired at reporting on this study. "You can't just look at the numbers of cases. You also have to look at the numbers of people who might have been diagnosed. You have to look at the rates. This is epidemiology 101."
He conceded that he doesn't know how to fix the problem of clueless reporting. "So what's the solution? I'm seriously wondering. This kind of stuff hurts science and the credibility of the media."
Prostate cancer and the two-hit hypothesis
Ricki Lewis, my colleague here at the PLOS Blog Network, examined the two-hit hypothesis of inherited cancers at her blog DNA Science, analyzing a NEJM paper about metastatic prostate cancer. The two-hit hypothesis, first proposed in 1971, argues that some inherited cancers are the product of a kind of one-two punch.
First, the patient is born with an inherited mutation in every cell, often in a gene that repairs broken DNA. This is a patient that is already half-way to cancer. But the mutant gene does no damage unless the patient has the misfortune to acquire another mutation, making the cell with the two damaged genes vulnerable to turning cancerous.
The paper reported finding inherited mutations in DNA repair genes in 84 out of 692 men with metastatic prostate cancer but without a known family history of cancer. At least some of their relatives are likely to have inherited the damaged DNA repair gene as well, and therefore be at higher risk for cancer.
The authors argue that all men with advanced prostate cancer should be tested for inherited mutations. DNA testing of this kind is not now common practice, and so insurance will probably not pay for it.
Prostate (and other) cancer in ancient times
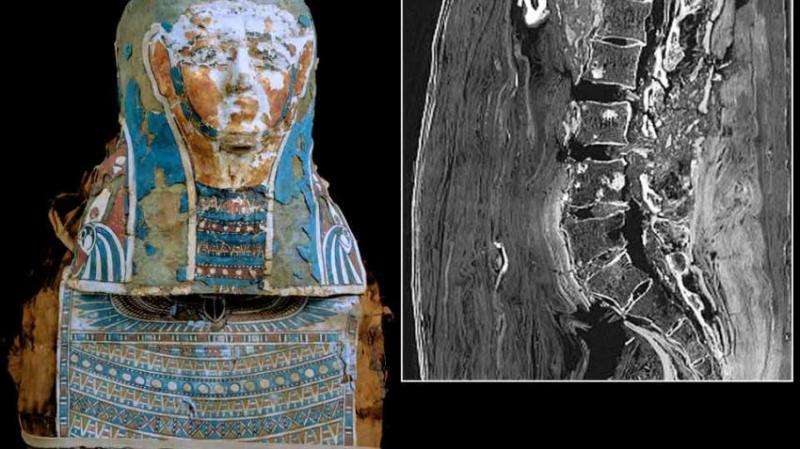
I take every opportunity to write about old bones, so this is the moment to mention that the oldest case of prostate cancer known so far was found in the 2700 year-old bones of a Scythian king who lived in southern Siberia. The second-oldest prostate cancer case is from an Egyptian mummy dating back 2250 years, which Heather Pringle reported on at Science.
Both men were relatively young by our standards, in their 50s. And in both cases the prostate cancer had metastasized and spread all over their bodies. Very, very painful.
The oldest known human cancer of any kind, according to Sarah Emerson at Motherboard, was revealed in a July paper that reported finding a malignant tumor in the foot of a 1.7 million year-old hominin fossil (species unknown.)
The paper's co-author told Emerson, "It's likely modern people suffer from cancer more than did our ancient ancestors, [but] it's more accurate to say that cancer has always been with us. Most likely, our modern lifestyles increase its prevalence."
It's a popular line of argument, that cancer is largely a disease of modernity. All those damn chemicals in the environment, you know.
But is it true?
The argument is based partly on the relative absence of cancer in fossils and mummies. I haven't found any recent data on this, but Pringle says a 1998 paper reported only 176 cases of skeletal malignancies among tens of thousands of ancient human remains examined.
As we all know, however, "absence of evidence is not evidence of absence."
Pringle suggests that paleopatholgy is subject to the same advantages-disadvantages as contemporary diagnostic methods. When the method improves, researchers find more cases. But that's not a real increase. It's simply improved diagnosis.
Diagnosticians of whatever era are at the mercy of their technologies. The Egyptian's metastasized prostate cancer lesions were very small, only detectable because the researchers had access to a new generation of high-resolution CT scanners.
Another obvious explanation for an apparent cancer increase in our times is this one: cancer is largely a disease of aging. Some possibly large proportion of modern cancer is almost certainly due to the fact that we are living much longer than our forebears. Long enough to develop cancer. Long enough for it to be diagnosed. Few Egyptians lived past 40. Which makes the one who died of metastasized prostate cancer in his 50s an old man for his time.
Steven Novella notes at Neurologica, "Given this fact, the dearth of malignancy [in ancient remains] hardly seems like a mystery." He concludes, "It is certainly possible that modern life does produce environmental factors that increase cancer risk. Smoking is a well established risk factor. Diets and sedentary lifestyle may also contribute. That does not make cancer a modern or man-made disease, however."
This story is republished courtesy of PLOS Blogs: blogs.plos.org.