Cardiovascular event risk of RA patients comparable to type-2 diabetes over 15-year period
Rheumatoid arthritis is associated with serious risk of cardiovascular (CV) disease events such as heart attack or stroke. Over a 15-year period, people with RA may have double the risk of CV events as those in the general population, rates that are similar to people with type-2 diabetes, according to new research findings presented this week at the 2016 ACR/ARHP Annual Meeting in Washington.
Rheumatoid arthritis (RA) is a chronic disease that causes pain, stiffness, swelling, and limitation in the motion and function of multiple joints. Though joints are the principal body parts affected by RA, inflammation can develop in other organs as well. An estimated 1.3 million Americans have RA, and the disease typically affects women twice as often as men.
Researchers at Amsterdam Rheumatology Immunology Center, VU University Medical Center and Reade in the Netherlands set out to learn more about the causes of increased mortality among people with RA, and the severity of their risk.
"In daily clinical practice, it seemed that RA patients more frequently suffered from myocardial infarctions than people in the general population. We started this study more than 15 years ago, as at that time, there were only sparse data with respect to cardiovascular morbidity in RA," said Prof. Michael T. Nurmohamed, MD, PhD, Head of the Rheumatology Research Department and one of the study's lead authors along with Rabia Acga, MD.
Data from the CARRÉ Study, a prospective cohort study whose aim is to investigate CVD risk factors in a random sample of 353 patients with long-term RA, researchers at VU University Medical Center Amsterdam in the Netherlands assessed heart disease-related events at 3, 10, and 15 years of follow-up. They compared their findings from these RA patients to glucose metabolism and CVD risk factors data from the Hoom Study of 2,540 patients in the general population.
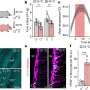
The researchers found that risk of cardiovascular events for people with established RA was more than double that of people in the general population. Their findings showed that 96 people in the RA group had a CVD event during 2,703 person-years of follow-up, or an incidence rate of 3.6 per 100 person-years. In the general population group, 298 individuals had a CV event during a follow-up of 25,335 person-years, or an incidence rate of 1.4 per 100 person-years. Out of those 298 patients, 41 had diabetes mellitus. Age- and sex-adjusted hazard rates for CV events were higher for both RA and diabetes compared to those in the general population.
Increased risk for heart attacks or strokes among people with established RA is comparable to individuals with type-2 diabetes. The increased risk for RA patients even after adjustments were made for traditional heart-disease risk factors remained elevated as much as 70 percent compared to the general population, the study showed. Their findings indicate that chronic, systemic inflammation in RA contributes independently to cardiovascular risks for these patients.
"In RA, there is also a need for cardiovascular risk management, just as in diabetes," said Dr. Nurmohamed. "There is a need for attention to this by patients as well as their treating rheumatologists. Cardiovascular risk management in RA should target disease activity as well as traditional cardiovascular risk factors. Unfortunately, despite all the knowledge, the latter is only poorly implemented."
Treating systemic inflammation effectively may address the increased risk of cardiovascular events and the higher mortality risk associated with them, said Dr. Nurmohamed.
"There's accumulating evidence that biologics reduce the cardiovascular risk in RA. However, the current strategy of tapering biologics might impose our patients to an increased cardiovascular disease risk," he said. "We aim to conduct some mechanistic studies in this respect."
Improvement of current cardiovascular risk prediction models by adding relevant biomarkers may also help rheumatologists better understand who in the RA population is most at risk for CV events and why, so effective interventions may be identified, he said.