How gut microbiome and diet can affect depression

An international group of researchers headed by André Carvalho has published in Psychotherapy and Psychosomatics a paper that provides new data and prospects for the links between the intestinal flora and several disorders, notably depression.
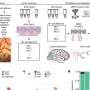
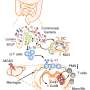
Persistent low-grade immune-inflammatory processes, oxidative and nitrosative stress, and hypothalamic-pituitary-adrenal axis activation are integral to the pathophysiology of major depressive disorder. The microbiome, intestinal compositional changes, and resultant bacterial translocation add a new element to the bidirectional interactions of the gut-brain axis. New evidence implicates these pathways in the onset of major depressive disorder. In addition, abnormalities in the gut-brain axis are associated with several chronic non-communicable disorders, which frequently co-occur in individuals with depression, including but not limited to irritable bowel syndrome, chronic fatigue syndrome, obesity, and type 2 diabetes mellitus.
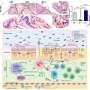
The composition of the gut microbiota is influenced by several genetic and environmental factors (e.g. diet). Several lines of evidence indicate that gut-microbiota-diet interactions play a significant pathophysiological role in depression and related medical comorbidities. Gut dysbiosis and the leaky gut may influence several pathways implicated in the biology of major depressive disorder, including but not limited to immune activation, oxidative and nitrosative stress, and neuroplasticity cascades. However, methodological inconsistencies and limitations limit comparisons across studies.
Authors conclude that intestinal dysbiosis and the leaky gut may constitute a key pathophysiological link between depression and its medical comorbidities. This emerging literature opens relevant preventative and therapeutic perspectives.
More information: Anastasiya Slyepchenko et al. Gut Microbiota, Bacterial Translocation, and Interactions with Diet: Pathophysiological Links between Major Depressive Disorder and Non-Communicable Medical Comorbidities, Psychotherapy and Psychosomatics (2017). DOI: 10.1159/000448957