Tiny packet is making a big—and growing—dent in childhood HIV
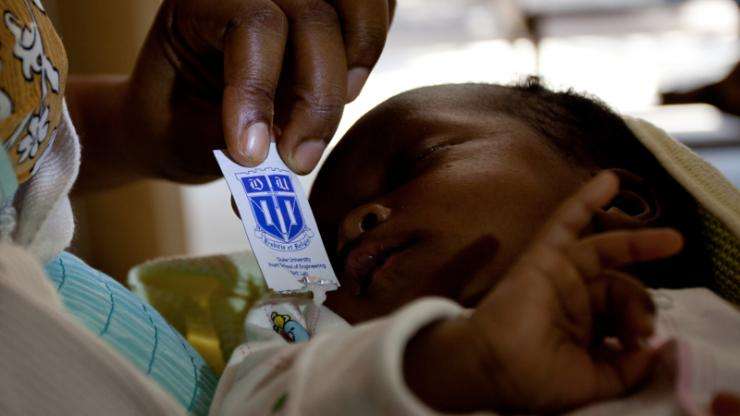
Developed in 2008, the Pratt Pouch—a ketchup packet-like pouch of antiretroviral drugs—has already saved thousands of lives in Ecuador, Zambia and Tanzania. And now, its reach is expanding in Ecuador and a new initiative will bring the pouch to Uganda.
The Pratt Pouch, named after Duke's Pratt School of Engineering, is a small packet of antiretroviral drugs that HIV-positive mothers can squeeze into their newborns' mouths to help prevent mother-to-child HIV transmission. The pouch, which made the World Health Organization's list of Top 10 Most Innovative Health Technologies in 2012, was developed by Robert Malkin, professor of biomedical engineering and global health, in collaboration with undergraduate engineering students.
Malkin is now working with undergraduates and community partners to make the pouch commonplace for HIV-positive mothers in Ecuador and Uganda.
Currently, the Pratt Pouch is being used in Guayaquil, Ecuador's largest city, to cover about twenty percent of births to HIV-positive women in the country. A new grant from a partnership between GSK and Save the Children will enable Malkin's team and their partners to offer the pouch in Quito, increasing coverage to about eighty percent.
Ecuador is a strategic location for pouch use expansion. "In Ecuador, every woman is tested for HIV when she comes into a hospital for pre-natal care or a birth, so we're able to reach a high percentage of HIV-positive women with the pouch," Malkin said.
Pouches are filled manually at local pharmacies, so the scale-up is not very difficult from an engineering perspective, Malkin shared. The challenge, he said, lies in the implementation—particularly the prospect of getting all of the stakeholders to work together. "This is a completely new way of packaging and delivering medications, requiring government agencies, hospitals and HIV support groups to cooperate and collaborate in new ways and, in some cases, for the first time," Malkin said.
Additionally, nurses and doctors must be trained to instruct mothers on how to use the pouch. Given high staff turnover rates, the training has to be efficient and repeatable.
The expansion is being managed by Fundación VIHDA, an organization based in Guayaquil that provides HIV services and works with the Ecuadorian Ministry of Health to improve HIV care in the country.
Meanwhile, with funding from USAID, Malkin is collaborating with the Elizabeth Glaser Pediatric AIDS Foundation, the Ugandan Ministry of Health and a number of other stakeholders to make the Pratt Pouch available in Uganda. The Uganda model differs from the project in Ecuador in two ways.
First, the target for this project is for 40 percent of HIV-positive mothers in the country to have access to the pouch, whether they give birth at a medical facility or at home. "Forty percent may not seem like much," Malkin said, "But HIV rates are much higher in Uganda than in Ecuador, so this is a very ambitious goal." Globally, Uganda has the fourth highest number of new HIV infections among children.
Second, the pouches will be manufactured using an automated filling process at a centralized plant, which will cut the time required to fill, seal and label one pouch from seventeen seconds to four seconds. Malkin hopes this new filling process will serve as a pilot to eventually scale up coverage to all of East Africa.
Duke engineering students designed and tested the machines that will help automate the pouch-filling process.
"The evolution of the Pratt Pouch has been driven by Pratt students from the beginning," said Malkin, "The idea for the machinery came from two of my students, Judy Zhu and Katie Gelman, in an independent study."
Zhu, a recent Pratt graduate, explained that the process was rewarding but difficult at times. "This was a medical application with direct impact, so the stakes were high," she shared. "However, it was also really cool to see the immediate impact that I was able to have on real people."
Malkin hopes one or more students will be able to travel to Uganda in the fall to assist in installing the machines and training workers.
As the global leader in the fight against pediatric HIV/AIDS, the Elizabeth Glaser Pediatric AIDS Foundation (EGPAF) is an ideal partner for this project.
EGPAF—which received the funding for this project through the Saving Lives at Birth Challenge—is providing technical oversight to the project and will advise on future scale-up initiatives. They're helping to integrate Pratt Pouch technology into the existing supply chain and service delivery platforms to design a sustainable, evidence-based model for national scale-up in Uganda and other low-resource countries.
Among EGPAF's contributions thus far are shepherding the project through intensive regulatory approval processes and providing technical assistance to Hospice Africa Uganda, the proposed pouch-filling facility.
Recently, with the help of Duke's Center for the Advancement of Social Entrepreneurship, Malkin connected with Joanne Moore, former vice president of Chemonics. Together, they founded Pratt Pouch Consulting (PPC), an organization dedicated to spreading the use of the pouch.
PPC partners with community organizations like EGPAF to write grants to fund expansion projects and help manage the projects.
More information: Learn more about the Pratt Pouch: dhtlab.pratt.duke.edu/pouch