Possible new immune therapy target in lung cancer
A study from Bern University Hospital in collaboration with the University of Bern shows that so-called perivascular-like cells from lung tumors behave abnormally. They not only inadequately support vascular structures, but also may actively modulate the inflammatory and immune response. These findings may represent a novel stromal cancer target.
Lung cancer accounts for the highest number of cancer-related deaths, with an estimated 1.6 million deaths in 2012 worldwide. Among different types of lung cancer, non-small cell lung cancer (NSCLC) is the most prevalent. Recent advances in genetic analyses led to targeted treatments that work very effectively in cases where tumors carry a specific targetable mutation. Another promising strategy focuses on redirecting the immune response to recognize and attack tumor cells. Despite these promising approaches, there is still a need to better understand the tumor dynamics that lead to lung cancer progression.
A research team from the Division of General Thoracic Surgery, Bern University Hospital that is also affiliated with the Department for Biomedical Research, as well as the ARTORG Center for Biomedical Research of the University of Bern found that perivascular cells play an important role in tumor progression. Their findings could lead to a novel immune therapy target in lung cancer. The results of the study have been published in Scientific Reports.
Perivascular cells are supporting the tumor
"There is increasing evidence for a link between perivascular cells and tumor growth, that's why we were trying to find it", says Sean Hall from the Thoracic Surgery Research Lab, Bern University Hospital. NSCLC specimens were collected from patients that underwent surgery at the Division of General Thoracic Surgery, Bern University Hospital. In the laboratory, he then isolated the perivascular cells from the lung cancer tissues.
In comparison with the same cell type isolated from normal lung tissue, perivascular cells from NSCLC lesions showed several abnormalities. Interleukin-6, a pro-inflammatory cytokine, was upregulated, as was PD-L1, a targetable immune-checkpoint-inhibitor. "These findings suggest that perivascular cells in NSCLC actively modulate the inflammatory and immune response", says first author Colette Bichsel from the ARTORG Center for Biomedical Engineering Research.
Leaking blood vessels
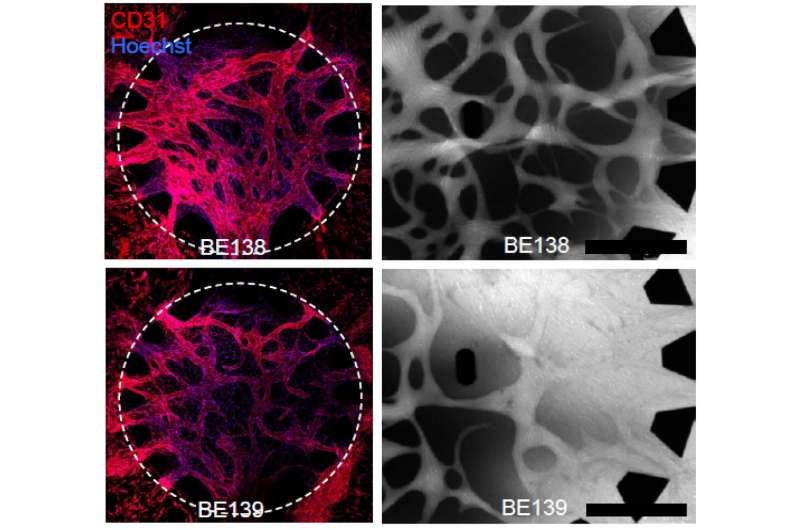
Next, the research team wanted to see how these cells fulfill their function of supporting blood vessels. To test this, Colette Bichsel developed a chip on which blood vessels can be grown and maintained in the lab. Blood vessels were successfully grown using both NSCLC-derived and normal perivascular cells as supporting cells. But there was one important difference: blood vessels with tumor-derived perivascular cells were leakier than normal blood vessels. "This shows that tumor pericytes inadequately support vascular structures, which may increase the likelihood of tumor cell evasion", explains Bichsel.
Taken together, the findings from this study show for the first time that perivascular cells play an important role in promoting a pro-inflammatory and immune-suppressing microenvironment. Further studies are needed to evaluate if they may present a target for new lung cancer treatments.
More information: Colette A. Bichsel et al. Increased PD-L1 expression and IL-6 secretion characterize human lung tumor-derived perivascular-like cells that promote vascular leakage in a perfusable microvasculature model, Scientific Reports (2017). DOI: 10.1038/s41598-017-09928-1