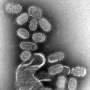
The U.S. may be in for a tough flu season—4 questions answered

This year, Australia suffered a record number of flu infections. This has some experts concerned that the U.S. will suffer a harsh flu season as well. Irena Kenneley, associate professor of nursing at Case Western Reserve University, explains what the news means and why it's important for Americans to receive their annual flu vaccine.
1. When exactly is flu season, anyway?
The timing of peak activity varies from year to year. Peak influenza activity in the U.S. usually occurs during December through February, but there can be substantial influenza activity up until the month of May.
This year, after a slow start in October, influenza cases are on the rise in many parts of the country, especially in the South. The flu season is now considered to be widespread in New York and California.
The influenza virus is among the most likely to cause significant epidemics in humans. The virus causes acute upper and lower respiratory tract infections, and can lead to potentially serious complications, such as pneumonia, bronchitis, sinus and ear infections.
The flu can be spread from person to person when an infected person talks, sneezes or coughs. That means it spreads easily. The virus circulates globally and affects all age groups.
2. Why do some think that it will be a bad season?
The Centers for Disease Control and Prevention estimate that, since 2010, the flu has led to hundreds of thousands of hospitalizations and somewhere from 12,000 to 56,000 deaths in the U.S. each year.
Clinicians are bracing for a potentially harsh flu season this winter. As of early December, there have been 7,000 confirmed cases in the U.S. That's double the amount as the same time last year.
Between Oct. 1 through Nov. 25, there were 566 confirmed hospitalizations due to influenza. The hospitalization rate was highest for those 65 and older.
There have been news reports that this year's flu vaccine is only about 10 percent effective, but those reports are misleading. Many of those reports focused on one strain of influenza found in Australia this year, which led to a record number of flu outbreaks.
However, health officials say that it's too early to tell how well the vaccine with work against the flu virus in the U.S.
The American vaccine is similar to Australia's vaccine, and the dominant strain of flu virus in Australia also appears to be the same as ours this season. This strain, called H3N2, is considered particularly virulent. Historically, it's considered the worst type of influenza A strain, even worse than H1N1. Right now, approximately 78 percent of the early strains that are circulating in the U.S. appear to be this H3N2 strain.
Last year, the U.S. flu vaccine was about 42 percent effective.
3. Why is it so tough to make flu vaccines?
One of the best ways to prevent the flu is through vaccination.
In general, flu vaccinations have an excellent safety record, but their efficacy varies greatly. Sometimes, the vaccine fails due to a mismatch of virus strains.
The problem with the influenza virus is that it is a moving target with dozens of strains. Unlike measles or chickenpox, which are stable viruses, the influenza virus mutates from year to year, enabling it to evade our immune system. From an evolutionary perspective, that makes it very successful.
The influenza virus can even cross over to other animals and then back to humans. When that occurs, it creates the potential for a new potentially lethal strain that can quickly become widespread.
Scientists are searching for a universal vaccine that would work against a wide variety of influenza viruses. An influenza vaccination that is genuinely universal would both protect us from viral mutations and give us lifelong immunity.
While there are many new ideas for designing a universal influenza vaccine, it will take years to develop one.
4. What does this mean for me?
Each year, only about 4 in 10 adults in the U.S. receive the flu vaccine.
Anything you can do to help prevent you and your family from getting the flu is very beneficial. The CDC recommends annual influenza vaccinations for everyone age 6 months or older. Vaccination is especially important for pregnant women, the elderly and others at high risk of influenza complications.
You can also prevent the spread of flu by washing your hands well and disinfecting common high-touch surfaces. Children should be taught to cover their coughs and stay home when sick, so as not to share their germs.
For people with confirmed or suspected influenza, particular those who are at high risk for complications, it's important to seek treatment with influenza antiviral medications as close to the onset of illness as possible.
Although the effectiveness of the U.S. flu vaccine is unknown, the vaccine remains a valuable public health tool. It is always better to get vaccinated than not to get vaccinated.
This article was originally published on The Conversation. Read the original article.![]()