Peptide improves glucose and insulin sensitivity, lowers weight in mice
Treating obese mice with catestatin (CST), a peptide naturally occurring in the body, showed significant improvement in glucose and insulin tolerance and reduced body weight, report University of California San Diego School of Medicine researchers.
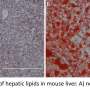
In a study published in Diabetes on February 6, researchers identified CST's role in the recruitment and function of macrophages in the liver as well as regulation of obesity-induced liver inflammation and insulin resistance.
"We have shown that an endogenous peptide, catestatin, can directly suppress glucose production from hepatocytes and can indirectly suppress lipid accumulation in liver as well as macrophage-mediated inflammation in obese mice," said Sushil K. Mahata, PhD, professor of medicine at UC San Diego School of Medicine. "The net results are improved glucose tolerance and insulin sensitivity. Therefore, this peptide has immense potential for an anti-obesity reagent as well as a novel drug to treat type 2 diabetes."
In a normal human body, the liver helps regulate blood sugar by stimulating the body to absorb glucose as glycogen (for future use as energy). When sugar levels increase in the blood, the pancreas secretes insulin to decrease glucose production from the liver to maintain balance.
When the liver stops responding to insulin, blood glucose levels rise, causing insulin production to go into overtime. If the body cannot maintain this heightened insulin production, the excess glucose leads to diabetes and other health disorders.
The liver also controls lipid production and metabolism. But in obesity, accumulation of lipids can cause fatty liver, resulting in cellular damage to the organ. In response to this damage, immune cells residing in the liver are activated, especially macrophages, and additional immune cells are recruited from the circulating blood. Macrophages are specialized immune cells that promote tissue inflammation by secreting inflammatory molecules, which can lead to insulin resistance and metabolic disease.
Treating obese mice with CST inhibited the recruitment of monocyte-derived macrophages to the liver and decreased inflammation, suggesting CST is an anti-inflammatory peptide. CST treatment also lowered blood sugar and insulin levels to normal, and reduced fatty liver. Administering CST had no effect on insulin or glucose tolerance in control lean mice, showing that the effect of CST is restricted to obese animals. This difference may be explained by the reduced levels of normal CST in obese mice compared to the lean control animals.
To confirm the importance of naturally occurring CST, the authors studied mice that lacked CST. These mice ate more and were heavier but lost weight when treated with CST. The researchers theorize that naturally occurring CST may help maintain body weight by suppressing hunger and enhancing glucose tolerance.
"The improved glucose and insulin sensitivity with CST treatment may be partly explained by the anti-inflammatory effects of catestatin on the liver," said Mahata. "We have identified a novel pathway for suppression of liver glucose production that could be used to compensate for the loss of naturally occurring CST or to bolster its impact. But further studies are needed to uncover how CST suppresses liver inflammation to improve metabolism."
More information: Wei Ying et al. Catestatin Inhibits Obesity-Induced Macrophage Infiltration and Inflammation in the Liver and Suppresses Hepatic Glucose Production Leading to Improved Insulin Sensitivity, Diabetes (2018). DOI: 10.2337/db17-0788