Women once considered low risk for heart disease show evidence of previous heart attack scars
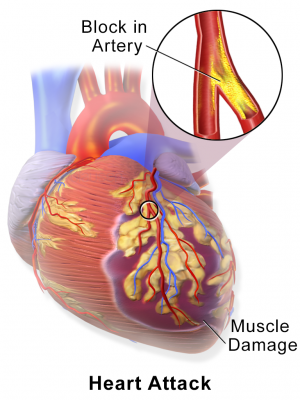
Women who complain about chest pain often are reassured by their doctors that there is no reason to worry because their angiograms show that the women don't have blockages in the major heart arteries, a primary cause of heart attacks in men.
But a National Institutes of Health study led by investigators at the Barbra Streisand Women's Heart Center in the Smidt Heart Institute, shows that about 8% of those women actually have scars on their heart that indicate they experienced a heart attack. The findings were published today in Circulation, the American Heart Association's peer-reviewed medical journal.
"This study proves that women need to be taken seriously when they complain of chest pain, even if they don't have the typical symptoms we see in men," said Janet Wei, MD, the first author of the study. "Too often, these women are told they don't have a heart problem and they are sent home instead of receiving appropriate medical care."
The study is part of the ongoing Women's Ischemic Syndrome Evaluation (WISE) study, a multiyear, multicenter research project. Sponsored by the National Heart, Lung, and Blood Institute, the study began in 1997 and has brought to light gender-related differences in heart disease.
The study looked at women who had complained of chest pain and had no coronary artery blockages. Results include:
- Of the 340 women who underwent cardiac magnetic resonance (CMR), a detailed imaging scan of the heart, 26, or 8%, were found to have myocardial scar, indicating the women had experienced prior heart muscle damage;
- Approximately one-third of those 26 women were never diagnosed with a heart attack, even though their cardiac scans indicated they had heart muscle damage;
- Of the 179 women who underwent a one-year follow-up CMR, 2 women, or 1% were found to have myocardial scar that wasn't there the year before; both of these women had interim hospitalizations for chest pain but were not diagnosed with heart attacks.
"Many women go to the hospital with chest pain but they often aren't tested for a heart attack because doctors felt they were low-risk," said Noel Bairey Merz, MD, director of the Barbra Streisand Women's Heart Center in the Smidt Heart Institute. "And they are considered low-risk because their heart disease symptoms are different than the symptoms men experience."
Bairey Merz, who also serves as the primary investigator of the WISE study, is a pioneer in uncovering the differences between men and women with heart disease.
Men with heart disease are more likely to have major plaque build-up in the major arteries bringing blood to the heart. A heart attack occurs when plaque causes blood flow to decrease or stop.
The WISE study has revealed that women who don't have blockages in their major heart arteries, but who experience chest pain might have microvascular dysfunction in the tiny vessels around the heart. That condition can go undetected because typical heart attack tests, such as an electrocardiogram, often don't detect microvascular dysfunction.
"We are finding that either these women are not being tested because doctors think they are at low-risk or that the tests doctors are ordering are not picking up these small heart attacks," Wei said.
As a result of the study, Wei and Bairey Merz are collaborating with Jennifer Van Eyk, PhD, a renowned expert in the study of proteins, including troponin, a protein that appears in the blood after a heart attack.
"By developing highly sensitive tests to detect previously unknown biomarkers, we may pinpoint and even prevent cardiovascular disease in women," Van Eyk said.