Gene panel predicts course of cystic fibrosis
Researchers at National Jewish Health have identified 10 immune-related genes whose activity during a respiratory infection predict the long-term prognosis for cystic fibrosis patients better than conventional measures. Five years after being evaluated, patients in the lowest-risk group were all alive and doing well, whereas 90 percent of patients in the highest risk cluster had been admitted to an intensive care unit, put on mechanical ventilation, referred for lung transplant, had a transplant or died. National Jewish Health has applied for a patent on the 10-gene panel.
"By looking at the underlying biology of the immune response, this panel allows us to identify subsets of cystic fibrosis patients who are likely to do better or worse in the long term," said Milene Saavedra, MD, associate professor of medicine and lead author on an article published in the Annals of the American Thoracic Society. "This information can help guide our treatment plans so we deliver the best outcomes for our patients."
National Jewish Health has the largest adult cystic fibrosis program in the nation. Cystic fibrosis is the most common genetic disease among Caucasians and afflicts about 30,000 people in the United States. It is caused by a defective chloride channel in cells, which can affect several organs. Patients develop thick mucus in their lungs, which provides an inviting environment for bacterial infections. Most patients die due to respiratory failure caused by repeated bacterial infections that damage the lungs.
Dr. Saavedra and her colleagues originally identified the 10 genes as early indicators of patients' response to treatment for disease exacerbations cause by respiratory infections. They next looked to see if those responses at the time of disease exacerbation correlated with long-term outcomes.
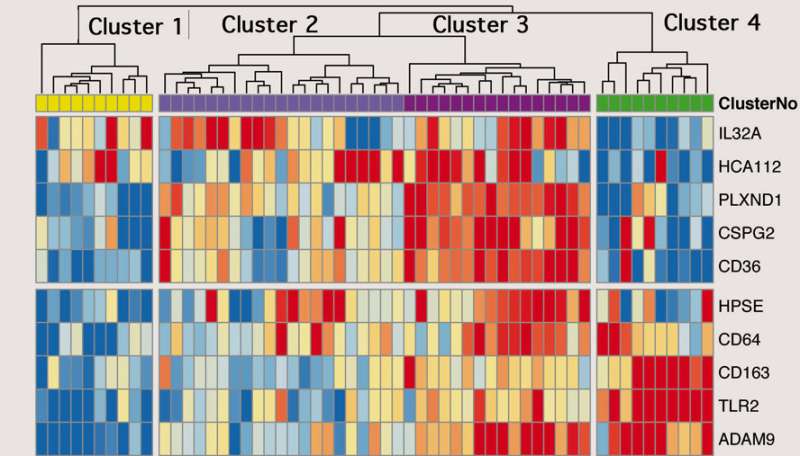
The gene expression of patients during exacerbations naturally fell into four distinct groups. The groups differed on several measures of disease activity and progression. Time to next exacerbation ranged from 291 days in Cluster 1 to only 73 days in cluster 4. Patients in Cluster 4 also had more severe exacerbations and more intense infections. The incidence of major illness events or death ranged from 0 percent in Cluster 1 to 92 percent for Cluster 4.
Standard measures for prognosis include a breathing measure known as FEV1, which measures the amount of air a person can expel in one second, and exacerbations in the previous year. The 10-gene panel was more sensitive than these tests, often enabling useful distinctions among patients with similar lung function or exacerbation history.
"FEV1 and exacerbation history tell us about a patient's disease history and existing lung damage," said Dr. Saavedra. "The gene panel tells us more about a patient's biological response to infection, which provides valuable information about the future course of the disease."
The genes upregulated in Cluster 4 patients showed excessive activation of the innate immune response, the first line of defense against infections. Patients in the low-risk Cluster 1 demonstrated greater expression of genes associated with the adaptive immune response, which is highly specific to particular pathogens.
"These findings can help guide our treatment plans for cystic fibrosis patients by further stratifying the highest acuity patients," said Dr. Saavedra. "We would presumably treat Cluster 4 patients more aggressively, trading potential side effects for more effective control of damaging infections."