Size matters when fighting cancer, study finds
Doctors could be a step closer to finding the most effective way to treat cancer with a double whammy of a virus combined with boosting the natural immune system, according to a pioneering study by researchers at The University of Texas Health Science Center at Houston (UTHealth) and The Ohio State University.
"The findings of this research are very exciting because it helps unravel the complex yin and yang relationship between the natural cancer-fighting power intrinsic to our immune system and externally added cancer-killing cells that are given as a therapy. It's very significant because it shows, contrary to recent scientific claims, that virotherapy can be combined with cell therapy for a positive effect," said the study's corresponding author Balveen Kaur, Ph.D., professor and vice chair of research in the Vivian L. Smith Department of Neurosurgery at McGovern Medical School at UTHealth.
Previous scientific wisdom has discredited combining virotherapy and externally added NK cell therapy to the body's natural killer (NK) cells, but there could be clear cancer-fighting benefits - providing enough external NK cells are deployed to destroy the tumor and stop its spread, as revealed in the paper published this week in Proceedings of the National Academy of Sciences (PNAS).
To reach this conclusion, physicians devised a mathematical formula unlocking the complex interactive relationship between externally introduced viruses and NK cells in addition to the immune system's existing NK cells to calculate cancer cell-killing potency. The mathematical modeling was able to predict how a virus-treated tumor would respond to NK cell therapy, depending on the number of NK cells introduced to the tumor. It showed that when the number of externally introduced NK cells is increased, the ability to fight cancer is strengthened. While the patient's own NK cells, present in smaller numbers, concentrate on clearing the virus and therefore have an adverse effect on virotherapy by limiting the virus's cancer-busting power, this impact can be reversed to destroy more of the tumor by introducing greater numbers of external NK cells. The theory behind these equations was subsequently confirmed in practice by experiments on mice with brain tumors, paving the way for further work.
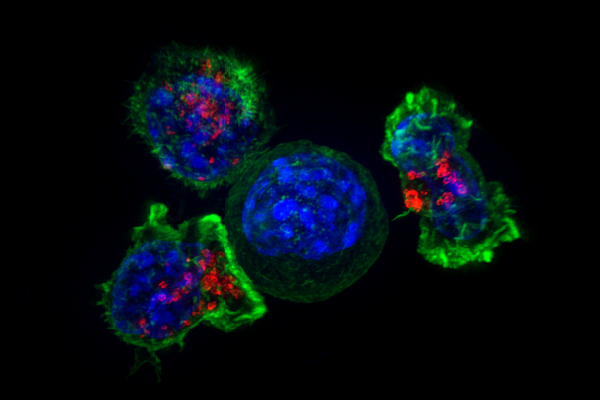
NK cells are an essential part of the innate immune system and they play a critical role in protecting the body from cancer. The primary function of NK cells is to fight infections, which means they attack the introduced virus, thus thwarting its therapeutic capacity. However, if sufficient numbers of extra NK cells are added, they can kill more tumor cells directly and compensate for this negative influence.
"Natural NK cells sense and kill infected cancer cells, thus clearing viruses. But by adding exogenous NK cells in sufficient quantities, they can also destroy the residual tumor. Our tests showed when you get this ratio right, there's a significant improvement in cancer-fighting efficacy," said Kaur, who is a member of The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences. "So it's a big step forward, which should create more opportunities for further research and development of clinical trials for the treatment of cancer in humans and animals."
More information: Yangjin Kim et al. Complex role of NK cells in regulation of oncolytic virus–bortezomib therapy, Proceedings of the National Academy of Sciences (2018). DOI: 10.1073/pnas.1715295115