Sustained virological response to oral hepatitis C virus treatment associated with reduced mortality in Italian cohort
Patients with chronic hepatitis C virus (HCV) infection who achieve a sustained virological response (SVR) after direct-acting antiviral agent (DAA) treatment have lower all-cause mortality, according to a real-world study presented today at The International Liver Congress 2018 in Paris, France. The study, conducted in Italy, found that patients who achieved SVR were at reduced risk of death from both liver-related and other causes.
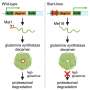
Chronic HCV infection affects an estimated 71 million people globally. Left untreated, a significant number of those people will develop cirrhosis or liver cancer, which leads to the death of an estimated 700,000 people with HCV infection each year. SVR, defined as undetectable HCV RNA 12 or 24 weeks after the end of therapy, equates to cure in >99% of patients. Although DAAs have proven highly effective at curing HCV, longer-term morbidity and mortality following DAA-induced SVR has not been well characterized.
"The long-term health benefits of an HCV cure, in terms of survival, need to be evaluated in long-term, real-world settings," explained Dr. Vincenza Calvaruso from the University of Palermo in Italy, and lead author of the study. "We were able to prospectively follow almost 5,000 patients from when they started DAA treatment and look at the impact of achieving SVR on their survival prospects, particularly in patients with Child-Pugh A compensated cirrhosis."
The study evaluated data from the prospective RESIST-HCV (Rete Sicilia Selezione Terapia—HCV) cohort which collates data for all HCV cases at Sicilian liver centres.23 Patients who started DAA treatment in 22 centres between March 2015 and December 2016 (4,926 patients, mean age 65.9 ± 11.6 years, 57.6% male) were observed for a median of 65 weeks (range 1-199). The patients were at different stages of disease; 1,158 (23.5%) were non-cirrhotic, 3,326 (67.5%) had compensated cirrhosis, and 442 (9%) had decompensated cirrhosis. Following DAA treatment, more than 90% of patients achieved SVR.
Fifty-three patients (1.1%) died after the antiviral therapy, 23 from liver-related causes and 30 from unrelated causes such as cardiovascular disease and sepsis. Patients who failed to achieve SVR were almost 30 times more likely to die from any cause than those who did achieve SVR (HR 28.9; 95% CI 16.5, 50.8; p<0.001). Both liver-related and non-liver related mortality were predicted by lack of SVR (HR 14.9, 95% CI 6.3, 35.1; p<0.001 and HR 41.77, 95% CI 17.3, 100.9; p<0.001, respectively) and by presence of decompensated cirrhosis (Child-Pugh B; HR 29.4, 95% CI 3.8, 223.9; p<0.001 and HR 3.0, 95% CI 1.4, 6.2; p=0.006, respectively). Body mass index and the presence of diabetes were also found to be predictors of non-liver-related mortality.
"We found that in this real-world setting with patients using a variety of DAA regimens, achieving SVR reduced mortality from both liver-related and unrelated causes at all stages of disease," said Dr. Calvaruso. "An interesting finding that deserves further investigation was a reduced risk of cardiovascular mortality for patients achieving SVR."
"DAA therapy results in the achievement of SVR, which is a cure of HCV infection in more than 90% of patients," said Prof. Markus Cornberg from the Hannover Medical School, Germany, and EASL Governing Board Member. "However, a recent Cochrane analysis has challenged whether or not DAA therapy will have an impact on mortality rates. These data are therefore important in documenting that achievement of SVR is beneficial and associated with reduced mortality."