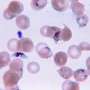
What is the economic impact of malaria for a pregnant woman living in an endemic area of Colombia?

Although malaria treatment is free of charge in Colombia, the economic costs incurred by pregnant women seeking care are considerable (mainly due to transportation and time lost), according to a new study led by ISGlobal.
Malaria in pregnancy leads to adverse health effects in the mother and newborn. This is true even in low transmission settings such as Colombia, where P. vivax is the predominant parasite species. Despite the fact that malaria treatment is free of charge within the Colombian health system, patients still incur costs, such as transportation and value of time lost due to the disease
The research team estimated such costs among 40 pregnant women with clinical malaria (30 percent Plasmodium falciparum, 70 percent Plasmodium vivax) in the municipality of Tierralta, Northern Colombia, an area characterized by armed conflict at the time of the study, where half of the population lives in rural areas and malaria risk is high. The economic costs incurred by pregnant women in the study were substantial (between US$16 and US$ 54). Total costs associated with inpatient treatment of a whole malaria episode (US $54.33) represented 18 percent of the monthly minimum salary in the country (US $307 at the time of the study). Transportation and indirect costs (time lost to the disease) accounted for great part of the total cost.
"Most of the women in the study belonged to the subsidized (and therefore poorest) group of the Colombian health system and 25 percent of them were indigenous, so we can speculate that the costs incurred by these women represent a significant share of their limited household budgets", explains lead author Elisa Sicuri. These costs likely represent one of the multiple constraints that women face when seeking care in areas marked by conflict, displacement and vulnerable indigenous populations.
Notwithstanding, the authors point out that Colombia is making strong efforts to improve access to quality health care and is not far from achieving universal health care insurance. Furthermore, the Colombian peace process, which culminated with the cease-fire in August 2016, will likely have a positive impact on achieving universal access to healthcare in conflict areas. They conclude that the current study can help inform malaria elimination initiatives in Colombia.
More information: Elisa Sicuri et al, Patients' costs, socio-economic and health system aspects associated with malaria in pregnancy in an endemic area of Colombia, PLOS Neglected Tropical Diseases (2018). DOI: 10.1371/journal.pntd.0006431