Researchers offer insights into liver disease caused by intravenous nutrition
Research by physician-scientists at the University of Colorado Anschutz Medical Campus offers hope for improved quality of life for people who rely on intravenous nutrition due to intestinal damage.
Karim C. El Kasmi, MD, Ph.D., assistant professor of pediatrics, and Ronald Sokol, MD, professor of pediatrics, are authors of an article in the April 2018 Nature Communications that sheds light on the underlying cause of intestinal failure-associated liver disease and suggests new therapeutic approaches.
Intestinal failure is a condition that occurs when a person's intestines are injured, damaged, or surgically shortened resulting in the need for the person to receive daily intravenous (IV) nutrition to sustain health. This IV nutrition, called parenteral nutrition, can be given in the hospital or at home through semi-permanent IV catheters.
Side effects of this form of nutrition are jaundice, liver injury called cholestasis, and eventually scarring in the liver. Intestinal failure-associated liver disease could eventually become so severe that the person would need a liver transplant or a combined liver and intestinal transplant to survive.
Until recently, there has been no effective therapy because of a poor understanding of how intestinal failure related to the development of the liver disease. Over the past decade, investigators have learned that reducing or changing the IV lipids can have a beneficial effect on some, but not all, patients.
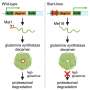
Drs. El Kasmi and Sokol developed a mouse model that mimics the situation in humans with intestinal failure who depend on IV nutrition. Mice with intestinal injury that are given PN through a central venous catheter for 7 to 28 days develop decreased liver function, called cholestasis, and liver injury.
The researchers were able to show that products from bacteria in the intestine of the mice, called lipopolysaccharides (LPS), are absorbed through the injured intestine and activate the immune system in the liver to produce a cytokine, IL-1 beta, leading to cholestasis. The combination of IV lipids and intestinal injury lead to the intestinal failure-associated disease.
With this understanding, the researchers identified three possible new targets for drug intervention to prevent or treat intestinal failure-associated disease. Several drugs that target these disease-causing pathways are already approved or in development. Further testing in clinical trials with affected patients is required, but this research opens the possibility of treating patients who need long-term IV nutrition without the worry of developing serious liver damage.
More information: Karim C. El Kasmi et al, Macrophage-derived IL-1β/NF-κB signaling mediates parenteral nutrition-associated cholestasis, Nature Communications (2018). DOI: 10.1038/s41467-018-03764-1