People with OCD process emotions differently than their unaffected siblings

A new study in Biological Psychiatry: Cognitive Neuroscience and Neuroimaging reports that people with obsessive–compulsive disorder (OCD) feel more distress when viewing images to provoke OCD-related emotions than their unaffected siblings. Although the unaffected siblings showed lower levels of distress, they had higher levels of brain activity in regions important for attention. The findings suggest that the family members may draw on additional brain resources to compensate for potential abnormalities in emotion regulation.
The study reveals an important difference in how the brain processes and regulates emotion between patients with OCD and their unaffected siblings. "This indicates that the brain function of people with OCD is a product of currently having the disorder, and unrelated to genetic or familial risk," said first author Anders Thorsen, MSc, of Haukeland University Hospital, Norway. The distinction is crucial for efforts to identify people at risk for OCD—a disorder that has strong genetic influences. Although difficulty with emotion regulation is thought to contribute to OCD, the findings indicate that brain activity patterns associated with abnormal emotion regulation cannot be used to identify people who are at genetic risk of OCD.
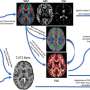
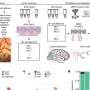
In the study, Mr. Thorsen and colleagues compared 43 patients with OCD, 19 unaffected siblings, and 38 unrelated healthy controls. During measurements of brain activity, participants viewed pictures to evoke fear or OCD-related symptoms, such as compulsive washing or checking the surrounding environment for potentialharm, and reported their levels of distress. The participants were instructed to either simply view the picture or try to tune down their negative emotions in response to the picture.
People with OCD and their unaffected siblings had similar brain responses and feelings of distress in response to fearful images as the healthy controls. However, when viewing OCD-related images, patients with OCD had increased distress and higher levels of activity in emotion-related brain regions than healthy controls. Brain activity in siblings fell between the levels in patients and controls, not distinguishable from either. "At the same time, siblings are also not like healthy controls," said Mr. Thorsen, referring to the higher levels of brain activity in attention-related brain regions when trying to regulate the negative emotion response.
"Interestingly, relatives show brain responses in areas that seem to be working harder to help them 'normalize' their responses to these types of OCD-related stimuli," said Cameron Carter, MD, Editor of Biological Psychiatry: Cognitive Neuroscience and Neuroimaging. The authors suggest that the harder working brain regions in siblings may represent compensation to help redirect their focus of attention to protect themselves from developing OCD.
"Future studies should try to further investigate this idea by following families with OCD through development," said Mr. Thorsen.
More information: Anders L. Thorsen et al. Emotion Regulation in Obsessive-Compulsive Disorder, Unaffected Siblings, and Unrelated Healthy Control Participants, Biological Psychiatry: Cognitive Neuroscience and Neuroimaging (2018). DOI: 10.1016/j.bpsc.2018.03.007