Gene therapy vectors carrying the telomerase gene do not increase the risk of cancer
Negative results and findings in science are perhaps less newsworthy, but they are no less important. In fact, negative results in a cancer study have demonstrated that a possible new therapeutic pathway against idiopathic pulmonary fibrosis and other diseases associated with short telomeres is, in fact, safe. Researchers from the Spanish National Cancer Research Centre (CNIO) have shown in a new study that the gene therapy with telomerase, proven effective in mice against diseases caused by excessive telomere shortening and aging, does not cause cancer or increase cancer risk, even in a cancer-prone setting. Their paper has been published in the journal PLoS Genetics .
For years, CNIO's Telomeres and Telomerase Group has been investigating the possibility of using the enzyme telomerase to treat pathological processes related with telomere shortening, as well as diseases associated with aging—cardiovascular and neurodegenerative diseases, among others—and even the aging process itself. In 2012, they designed a highly innovative strategy: a gene therapy that reactivates the telomerase gene using adeno-associated viruses (AAV). These gene therapy vectors do not integrate in the genome of the host cell, thus, telomerase only performs its telomere-reparative actions during a few cell divisions before the vector is diluted out. This minimizes cancer promotion, a potential risk associated with the activation of telomerase. But to what extent? The potential medical use of telomerase still clashes with fears surrounding a possible increased risk of cancer.
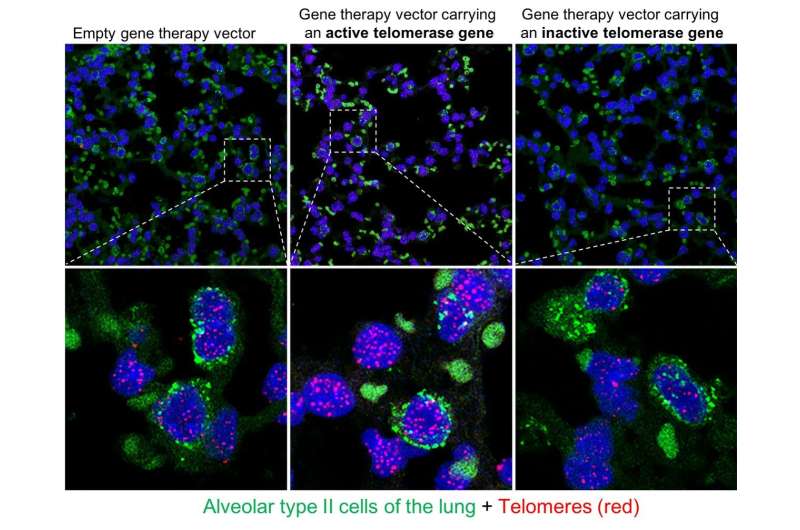
The paper being published now specifically tackles this question by applying gene therapy to a mouse model of human lung cancer. The results were negative: "The activation of telomerase by means of [this gene therapy] does not increase the risk of developing cancer," even though tumours are forced to appear in a relatively short time in this mouse model, authors write.
"These findings suggests that gene therapy with telomerase appears to be safe, even in a pro-tumour context," noted Blasco. "In our research, we were already seeing that this gene therapy does not increase the risk of cancer, but we wanted to conduct what is known as a 'killer experiment," an experiment that creates the worst conditions for your hypothesis to hold true; if it survives even under those circumstances, the hypothesis is truly solid. That is why we chose these mice; they are animals that spontaneously develop a type of lung cancer that is very similar to the human form, which normally never appears in normal mice. We can't think of any other experiment that would provide a better demonstration of the safety of this therapy."
Telomeres are at the ends of chromosomes in the nucleus of every cell. With each cell division, telomeres get a bit shorter, and when this shortening becomes excessive, the cell stops dividing and the tissue from which they are derived no longer regenerates. We know that telomere shortening plays a key role in aging. Both in animal models and in humans, it has been shown older animals have shorter telomeres. It has also been proven that mutations in genes related to telomeres give rise to a series of diseases called telomere syndromes, including aplastic anaemia and idiopathic pulmonary fibrosis.
Telomerase is the enzyme that repairs the telomeres. In general, telomerase is only active during embryonic development (especially in the so-called pluripotent cells), but a few days after birth, its expression is silenced. In healthy adults, most cells do not contain telomerase .Their telomeres cannot be repaired after each cell division, and are thus shorter than in younger individuals. One exception are cancer cells, in which telomerase is active, which is why these cells divide prolifically—their telomeres never shorten enough to halt division, and as a result, cancer cells are virtually immortal.
Telomerase has always been seen as a double-edged sword. Repairing telomeres prevents one of the causes of aging, along with a series of diseases, but it could also favour the unchecked division of emerging tumours, thus causing cancer.
Researchers from CNIO have witnessed the power of telomerase in action. In 2001, they created the first transgenic mice that expressed adult telomerase, and they saw that with aging, there could be a slight increase in the incidence of cancer. But in 2008, they proved that transgenic animals for telomerase also aged more slowly and lived up to 40 percent longer if, besides expressing telomerase, they were also made more resistant to cancer. This strategy is not applicable to humans, because it would entail modifying the genome from the embryonic stage.
However, gene therapy is potentially applicable, activating telomerase where it is required following a single local injection. Thus far, researchers have managed to demonstrate that gene therapy with telomerase is proving to be effective in mice against infarction, aplastic anaemia and idiopathic pulmonary fibrosis.
In all cases, gene therapy with telomerase has been seen to offer therapeutic effects. In one of the most spectacular results, telomerase therapy halted the progression of pulmonary fibrosis in animal models. Although none of the mice subjected to gene therapy developed more cancer, the CNIO group wished to conduct an experiment to dispel any doubts and prove that safe therapy based on telomerase is possible in order to speed up the clinical application of telomerase for the treatment of diseases that currently have no cure.
More information: Miguel A. Muñoz-Lorente et al, AAV9-mediated telomerase activation does not accelerate tumorigenesis in the context of oncogenic K-Ras-induced lung cancer, PLOS Genetics (2018). DOI: 10.1371/journal.pgen.1007562