Putting research at heart of response to epidemics like Ebola saves lives
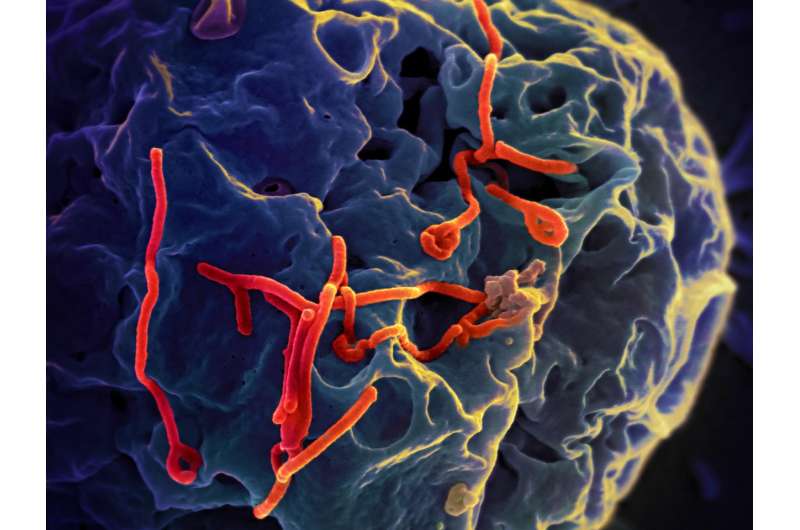
With the recent outbreak of Ebola in the Democratic Republic of the Congo declared officially over, Michael Regnier looks at how Wellcome's support has helped the people of DRC – and the rest of the world – to be better prepared for the next one.
On 8 May 2018, the government of the Democratic Republic of the Congo (DRC) confirmed an outbreak of Ebola virus in the country. DRC has experienced and contained Ebola several times since the virus was first identified there in 1976, but following the 2013-16 outbreak in West Africa, in which more than 11,000 people died, there was an appreciation that this had the potential to become more serious than previous outbreaks.
On the same day Ebola was confirmed, Wellcome released £2 million to fund research in DRC that would support the emergency response. A further £1 million was given by the UK Department for International Development through our partnership with them, the Joint Initiative on Epidemic Preparedness.
No one knew how big the outbreak would be or how long it would last. Because some of the first cases were around the city of Mbandaka, there were concerns that it might spread out of control. In the end, 33 people died, out of 54 cases – about the same scale as three outbreaks in DRC between 2008 and 2014, and much less devastating than the West African epidemic.
So what research was supported this time, and how will it help us prepare for future epidemics?
Vaccination
For the first time, an Ebola vaccine was available at the start of an outbreak. The vaccine, rVSV-EBOV, is manufactured by MSD (Merck). It was developed thanks to the efforts of many people, from researchers at the Public Health Agency of Canada to pharma companies, governments and NGOs, as well as the scientists and medical teams who ran clinical trials and the volunteers who took part in them.
Wellcome played a role, too, funding research and pushing for clinical trials to be done during the 2013-16 epidemic. These trials, coordinated by the World Health Organization (WHO), showed that the vaccine was safe and effective.
rVSV-EBOV is not the only vaccine in development, but it was the only one to demonstrate protective benefit in the 2013-16 epidemic and has been stockpiled by GAVI, the Vaccine Alliance as a result. It has not yet been licensed, though, meaning that it can be used only in research studies when consent is obtained from the people taking part and they are followed up to monitor safety.
With our research funding in place, the DRC government, the WHO and Médecins Sans Frontières were quickly able to start setting up a vaccination programme. This included everything from bringing in freezers to store the vaccine at -70°C, to hiring the people who would do the fieldwork, as well as working with other partners such as UNICEF when engaging affected communities.
Experts were flown over from Guinea to share their first-hand experience of good clinical practice when caring for people with Ebola and of the 'ring vaccination' approach. Ring vaccination means starting with a patient and finding everyone who has been in contact with them, and then tracing everyone the people in that first 'ring' have been in contact with as well. Everyone in these rings is then offered the vaccine, as well as first responders such as health workers and taxi drivers.
Compared with vaccinating the entire population, this is a more practical approach during a crisis. But it still relies on epidemiologists, lab workers testing samples, and thousands of personal visits by trained contact tracers.
The programme in DRC started on 21 May and by the end of June, 3,300 people had been vaccinated as a result.
The vaccination programme may have helped to slow and even stop the spread of the virus, but it will be hard to draw any firm conclusions given that the outbreak was relatively – and thankfully – short. We will, however, know more about the vaccine's safety as a result of this programme.
Clinical care
People with Ebola need to be able to trust that they will get the best possible care, and the best care starts with the right diagnosis. In its early stages, Ebola tends to involve a fever, aches and pains – not unlike other infections such as malaria or the flu.
During an epidemic, it's vital to know who actually has Ebola – preferably before they develop the life-threatening symptoms that follow, including vomiting, diarrhoea, organ failure, and internal and external bleeding.
Some of our funding went towards building up the DRC's capacity to use and assess new and developing diagnostic tools in outbreaks such as this one.
A handful of drug treatments for Ebola are in development – again, none of them has yet been licensed so WHO and DRC authorities agreed protocols for using them in this outbreak on a compassionate, case-by-case basis. Although the outbreak was over before any of them were prescribed, it is helpful to have those protocols in place so that investigational drugs can quickly be used and assessed during the next outbreak.
Communication, coordination and capacity
Epidemics are alarming and frightening wherever they happen. It's vital that communication between officials and the public is constructive, that research is supported, coordinated and shared, and that people feel engaged with decisions that get made.
Wellcome funded a team to produce operational briefs setting out local social and cultural contexts – these helped shape communication with the affected communities about Ebola, the vaccine and other public health measures in effect.
Some of our funding has also been used to strengthen research capacity in DRC so that the country will be even better prepared for the next time Ebola strikes. This includes support for the National Regulatory Authority and the Ethics Research Committee, and establishing a national research coordinator at the National Biomedical Research Institute (INRB) in Kinshasa.
Our support means issues such as how best to share samples and data have been considered, facilitating further research on Ebola now and in the future.
Preparation
Ultimately, the effect of quickly committing funding was to ensure that research was integrated in the emergency response to the Ebola outbreak, led by the DRC government with support from the WHO and other partners.
Epidemics are not single events. Every nation around the world needs to know their risks – some have to deal with seasonal epidemics, others with sporadic outbreaks, but all have to be ready with robust plans in place. And, crucially, research needs to be an integral part of these plans so that we learn more from every outbreak and become better prepared for the next one.
















