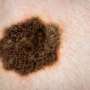
Melanoma linked with CLL, close monitoring recommended
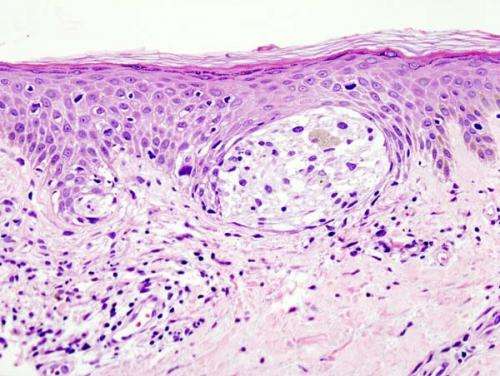
While studying a large group of individuals with chronic lymphocytic leukemia (CLL), a Wilmot Cancer Institute scientific team made an important discovery—these patients had a sizable 600 percent higher risk of melanoma, the most dangerous form of skin cancer.
Although a higher risk of melanoma had been known, a full analysis of detection rates and treatments among CLL patients has never been reported before, said Clive Zent, M.D., who led the study. It was published by the journal Leukemia Research.
As a result of this new data, Zent, an international expert in CLL, recommends that all clinical teams who care for CLL patients should actively monitor for melanoma as a part of routine care. The goal is to catch the skin cancer early and manage it with the newest targeted therapies.
"We do not for sure know why CLL patients are more susceptible to melanoma, but the most likely cause is a suppressed immune system," said Zent, a professor of Hematology/Oncology and Medicine at the University of Rochester Medical Cancer and Wilmot. "Normally, in people with healthy immune systems, malignant skin cells might be detected and destroyed before they become a problem. But in CLL patients, failure of this control system increases the rate at which cancer cells can grow into tumors, and also the likelihood that they will become invasive or spread to distant sites."
Study results showed that 22 melanomas were diagnosed among 470 people in the cohort, a rate that's more than 600 percent higher than what would be expected in a similar group of age- and gender-matched people from the general population. Of the 22 diagnoses, 15 (or 68 percent) were detected through monitoring in the UR Medicine dermatology clinic associated with Wilmot, and two cases (9 percent) were found by CLL specialists. Eighty eight percent of the cases involved earlier-stage disease with a better prognosis, the study said.
Researchers also noted a bright spot: one CLL patient, a 75-year-old woman, who developed advanced melanoma, was treated with a targeted cancer-immunotherapy drug, pembrolizumab (Keytruda), and went into remission for more than two years. She had been taking another targeted therapy, ibrutinib, for the leukemia. Zent believes this is the first published report to offer evidence that the ibrutinib/pembrolizumab combination was effective.
CLL is the most common type of leukemia in the U.S., with about 140,000 people living with the disease. Immune dysfunction is a major complication. Zent said the
Wilmot research supports the need for larger studies to seek solutions for the CLL/skin cancer risk.
The Cadregari Endowment Fund at the Wilmot Cancer Institute supported the investigation. First author is William J. Archibald, a former UR School of Medicine and
Dentistry student who has since graduated and performed much of the work on the study while in Rochester. Zent is editor-in-chief of the journal that published the paper, but he was blinded to the peer-review process, which was overseen by another editor at the journal.
More information: William J. Archibald et al, Management of melanoma in patients with chronic lymphocytic leukemia, Leukemia Research (2018). DOI: 10.1016/j.leukres.2018.07.003