Heart procedure for AFib better than drug therapy for reducing episodes
Atrial fibrillation is a common arrhythmia that affects an estimated 30 million people worldwide. New research shows that catheter ablation, a common cardiovascular procedure, appears no more effective than drug therapy to prevent strokes, deaths and other complications in patients with atrial fibrillation. But patients who receive catheter ablation experience much greater symptom relief and long-term improvements in quality of life. And they have fewer recurrences of their atrial fibrillation and fewer hospitalizations than those who receive only drugs. You can learn more about this new research in the March 15 issue of JAMA.
This research, funded by the National Heart, Lung, and Blood Institute (NHLBI), part of the National Institutes of Health and industry collaborators, is the result of the Catheter Ablation Versus Antiarrhythmic Drug Therapy for Atrial Fibrillation trial (CABANA), the largest international randomized clinical trial comparing left atrial catheter ablation—which involves inserting long, narrow tubes to reach and apply energy (hot or cold) to destroy abnormal heart tissue—with current state-of-the-art drug therapy to reduce the consequences of atrial fibrillation. A related observational study using big data to support clinical trial evidence is published in the European Heart Journal.
Most individuals with atrial fibrillation have identifiable risk factors, such as high blood pressure or structural heart disease, and tend to be elderly. Some patients with atrial fibrillation are symptomatic, while others remain asymptomatic. Atrial fibrillation also increases a person's risk of stroke, heart failure and other serious health conditions. Treating atrial fibrillation with antiarrhythmic drugs has been challenging due to limited effectiveness and potential adverse effects. Thus, catheter ablation therapy has become a generally adopted alternative technique to treat atrial fibrillation. Modestly sized randomized controlled trials have compared the therapies, but much uncertainty still exists about the long-term benefits of ablation relative to drug therapy.
"We have long known that physicians and patients are dissatisfied with drug therapy for atrial fibrillation, so we pursued this study to find out if catheter ablation would provide more effective treatment for these patients," says Douglas Packer, M.D., a Mayo Clinic cardiologist and the study's principal investigator. "While data from the trial was inconclusive in showing that catheter ablation was better than drug therapy in reducing rates of deaths and strokes, it showed strong evidence of reduced recurrence of atrial fibrillation, as well as reductions in mortality or cardiovascular hospitalizations."
CABANA enrolled 2,204 patients at 126 centers in 10 countries from 2009 to 2016. Each patient had new-onset or undertreated atrial fibrillation. In the study population, the median patient age was 68, and 37 percent were women. There were significant co-morbidities, such as high blood pressure, and a history of stroke and diabetes. Patients were randomly assigned to two groups of equal proportions to catheter ablation or drug therapy.
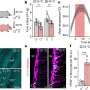
The primary comparison between catheter ablation and drug therapy showed a 14 percent lower risk of major complications such as death, stroke, severe bleeding and cardiac arrest, but the difference was not statistically significant. Ablation significantly reduced mortality or cardiovascular hospitalization by 17 percent when compared with drug therapy and reduced atrial fibrillation recurrence by 48 percent. When compared to drug therapy, ablation produced clinically important improvements in quality of life and in symptoms related to atrial fibrillation. These improvements were sustained over five years.
In large trials with longer follow-up, such as CABANA, patients don't always follow the assigned therapy. About nine percent of the ablation patients did not get their procedure and almost 30 percent of the drug therapy group got an ablation procedure, researchers reported. These "crossovers" who did not receive their assigned therapy may have affected the results of the study, Dr. Packer says. "You can't benefit from a therapy if you don't receive the therapy," he says.
However, when investigators examined the data according to the treatment received, the ablation group had significantly lower rates of death (40 percent), as well as the combination of death, disabling stroke, serious bleeding, or cardiac arrest (33 percent), compared with patients who only received drug therapy, he says.
One year after the start of treatment, patients in both groups showed substantial improvements in quality of life measures and measures related to atrial fibrillation, such as fatigue and shortness of breath. When compared to drug therapy, however, ablation produced additional improvements in quality of life and symptoms that were sustained over the five-year period, says Daniel Mark, M.D., of Duke Clinical Research Institute who led the quality of life analysis.
For example, at the beginning of the study, 86 percent of patients in the ablation group and 84 percent of patients on drug therapy reported atrial fibrillation symptoms during the previous month. By the end of the study, only 25 percent in the ablation group reported symptoms, compared with 35 percent in the drug therapy group, Dr. Mark says.
More information: JAMA (2019). dx.doi.org/10.1001/jama.2019.0693