New study highlights need for ethnic and ancestral diversity in genomic research

A new multicenter analysis led by researchers at the Fred Hutchinson Cancer Research Center, the Icahn School of Medicine at Mount Sinai and other institutions found the inclusion of diverse, multiethnic populations in large-scale genomic studies is critical for reducing health disparities and accurately representing genetics-related disease risks in all populations. The results appear in the June 19 issue of the journal Nature.
Genetic association studies look for genes or regions of the genome that contribute to a disease, but most genome-wide association studies to date have centered on populations of European ancestry. Because genetic architecture differs across racially and ethnically diverse populations, drawing universal conclusions from a limited sample can be misleading and even dangerous, exacerbating health care disparities.
"Previous articles have alluded to the need for multiethnic diversity in genome-wide studies, but our study is among the first to clearly delineate the scope of the problem, using detailed analyses of minority genetic samples," said Dr. Christopher Carlson, associate member of the Public Health Sciences Division at Fred Hutch and one of the study's two corresponding authors.
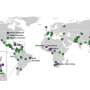
The research team analyzed data from the PAGE (Population Architecture using Genomics and Epidemiology) study, which assessed genetic associations of 26 clinical and behavioral traits in 49,839 non-European individuals from the United States. They included obesity, lifestyle risk and cardiometabolic traits such as body mass index, number of cigarettes smoked per day, amount of coffee consumed, blood pressure, disorders like Type 2 diabetes and others.
"To date, millions of genomes have been sequenced, but ethnic diversity has been lacking," said Dr. Eimear Kenny, associate professor of Medicine and Genetics, director of the Center for Genomic Health at the Icahn School of Medicine, and a corresponding author. "Because the availability of non-European genomic data is limited, existing clinical therapies may disproportionately benefit those of European descent, further widening the health disparities gap."
Using a variety of analytical tools, the researchers created a blueprint for analyzing genetic associations in diverse populations and identified 27 new trait-variant associations.
"By examining previously underrepresented populations, we found new ancestry-specific associations, which furthers our understanding of the genetic architecture of traits and underscores the importance of including diverse populations in these studies," said Dr. Ulrike Peters, associate director of Fred Hutch's Public Health Sciences Division and a senior author of the paper.
The study design accounted for the fact that subjects in the PAGE study were not discrete population groups, but instead were on a continuum of genetic ancestry, and results showed that ancestry-specific findings may be transferable among groups that share components of genetic ancestry. For example, the researchers identified in some Hispanics/Latinos a genetic association that was recently reported in African-Americans—the connection being a shared African ancestry.
"Among other things, this specific genetic variant can increase the risk of Type 2 diabetes complications by skewing results of glucose tests. This finding suggests that these types of genome-wide studies with diverse populations can help level the playing field in clinical practice and expand the reach of precision medicine to individuals who otherwise would not be included," said Dr. Charles Kooperberg, head of the Hutch's Biostatistics Program, one of the article's senior authors.
More information: Genetic analyses of diverse populations improves discovery for complex traits, Nature (2019). DOI: 10.1038/s41586-019-1310-4, www.nature.com/articles/s41586-019-1310-4