Antibiotics reduce survival rates in cancer patients taking immunotherapy
Cancer patients on immunotherapy fare worse if they have recently taken antibiotics, with their response and overall survival rate "crashing."
The findings come from a study of almost 200 cancer patients in the UK taking a type of immunotherapy called checkpoint inhibitors, part of the standard treatment pathway for cancer patients on the NHS.
Researchers found that patients who received broad spectrum antibiotics in the month leading up to starting the treatment had significantly worse responses to immunotherapy.
Compared with patients who received antibiotics alongside the immunotherapy or not at all, antibiotic treatment before immunotherapy was associated with lower overall survival rates and patients' cancers were more likely to progress.
The researchers suggest this may be because antibiotics disrupt the balance of bacteria and microbes in the gut, called the microbiome, which in turn impact the immune system.
The prospective study, led by researchers at Imperial College London and published today in the journal JAMA Oncology, highlights the importance of the timing of antibiotic treatment and the need for further studies to understand the mechanisms at play.
The researchers say that the findings have the potential to influence clinical practice, including a higher threshold for giving antibiotics to cancer patients starting immunotherapy.
Dr. David Pinato, from Imperial's Department of Surgery & Cancer and corresponding author of the study, said: "Cancer immunotherapy can be successful in around 20 percent of patients, but it's very difficult to predict who is going to respond. This work adds further evidence that antibiotics have an impact. We have shown that with prior antibiotic exposure, patients' response to immunotherapy and survival crashes."
Immune response
In the study, the team looked at 196 patients receiving immunotherapy as part of their routine care on the NHS, and who were treated at Imperial College Healthcare and Chelsea and Westminster Hospital NHS Trusts.
Patients' primary disease included non-small cell lung cancer, melanoma, head and neck cancer, carcinomas and other types of cancer. All patients were treated with immune checkpoint inhibitors, a therapy which disrupts the ability of cancer cells to 'hide' themselves, enabling the body's immune cells to target and destroy tumours.
The researchers looked at whether patients had received broad spectrum antibiotics up to 30 days prior to beginning their immunotherapy treatment, or whether they received antibiotics during their therapy—with respiratory infections being the most common cause for being prescribed antibiotics.
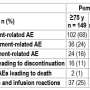
A total of 26 patients received prior antibiotics and 68 received them during their immunotherapy, and median overall survival after therapy was 14.6 months.
However, analysis revealed that patients with prior antibiotic use had a median overall survival of just two months, compared to 26 months for those with no antibiotic use prior to treatment. A similar effect was seen across all cancer types.
Patients with prior antibiotic use were likely to be less responsive to immunotherapy, with their primary disease almost twice as likely to progress. The study also showed the effect was independent of the class of antibiotic used—which for this group of patients included beta-lactams, quinolones, macrolides, sulphonamides, tetracyclines, aminoglycosides and nitroimidazole.
Critical timing
According to the researchers, more work is urgently needed to understand the mechanism behind the reduced response and drop off in overall survival.
But they believe that broad spectrum antibiotics before immunotherapy disrupt the balance of microbes in the gut—collectively called the microbiome—reducing the diversity of bugs present and potentially impacting on the body's immune response.
"We know that giving patients antibiotics affects their microbiome and increasingly, the evidence shows it influences treatment outcomes," Dr. Pinato added.
"It is important that patients who need antibiotics to treat bacterial infections receive the drugs they need," he explained. "But these findings urge for more care in the decision-making process for some patients.
It raises questions of whether we need a higher threshold for antibiotic prescribing in cancer patients due to receive immunotherapy."
The team highlight some limitations to the findings, including the small number of patients, and a lack of direct observations of changes to the gut microbiome. They also add that it is not possible to account fully for the impact any other health conditions the patients may have had (comorbidities) could have had on their survival. However, they explain they remain confident of the link and the need for further studies to expand on these findings.
The researchers now aim to carry out further studies to see what impact, if any, prior antibiotic use is having on the microbiome of patients with a follow-up observational clinical trial funded by the NIHR Imperial Biomedical Research Centre. They add that future studies could investigate whether rebalancing or augmenting the microbiome could improve patient outcomes.
More information: David J. Pinato et al. Association of Prior Antibiotic Treatment With Survival and Response to Immune Checkpoint Inhibitor Therapy in Patients With Cancer, JAMA Oncology (2019). DOI: 10.1001/jamaoncol.2019.2785



















