Q&A: Thyroid disorder may not show symptoms until pregnancy

Dear Mayo Clinic: I'm five months pregnant and was just diagnosed with hypothyroidism. I've never had thyroid problems before. Could this diagnosis be connected to my pregnancy? Will the hypothyroidism go away after I have my baby?
A: It's likely that the hypothyroidism was triggered by your pregnancy, but the underlying cause of the condition probably isn't the pregnancy itself. Some women have a thyroid disorder that doesn't show any symptoms until they become pregnant. Once symptoms appear, it's important to receive treatment and continue to receive follow-up care for six to nine months after the baby is born. You'll also need periodic checkups after that to monitor your thyroid function, especially if you become pregnant again.
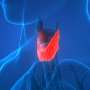
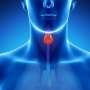
Your thyroid is a small, butterfly-shaped gland at the base of the front of your neck. The hormones that the thyroid gland makes—triiodothyronine, or T3, and thyroxine, or T4—affect all aspects of your metabolism. They maintain the rate at which your body uses fats and carbohydrates, help control your body temperature, influence your heart rate, and help regulate the production of proteins.
Research has shown that about 10% of young women have a thyroid disorder that, although it doesn't cause any problems before pregnancy, flares up and produces symptoms during pregnancy. Women who have a thyroid disorder often are found to have high concentrations of anti-thyroid antibodies in their bodies, a condition known as chronic thyroiditis, Hashimoto's disease or autoimmune thyroid disease. After childbirth, the antibody level usually increases and may lead to temporary altered thyroid function. This also may occur during pregnancy.
As in your case, this thyroid disorder often leads to hypothyroidism—a condition caused by low levels of thyroid hormones in the body. Some common symptoms of hypothyroidism can be hard to spot during pregnancy because they mimic signs of pregnancy, such as weight gain, fatigue and constipation. Other symptoms of hypothyroidism that may be more obvious during pregnancy include increased sensitivity to cold, dry skin, a puffy face, muscle weakness, hoarseness, joint pain or stiffness, and difficulty with concentration or memory.
For someone in your situation, treatment for hypothyroidism with thyroid hormone (levothyroxine) is crucial because untreated hypothyroidism can affect fetal development and maternal health during pregnancy. You'll need to be monitored carefully throughout your pregnancy, including blood tests to check your thyroid function every four to eight weeks.
In some women, this condition also results in a disorder known as postpartum thyroiditis after pregnancy. This disorder can lead to hypothyroidism or hyperthyroidism, which is a condition caused by high levels of thyroid hormones in the body. Hyperthyroidism after pregnancy often resolves on its own without treatment. If hypothyroidism develops after childbirth, however, treatment typically is needed for about six to 12 months. It usually can be discontinued after that.
Keep in mind, though, that even when treatment successfully eliminates hypothyroidism in a case like yours, the underlying thyroid disorder remains. That means if you get pregnant again, the likelihood is high that you will develop hypothyroidism again—no matter how much time elapses between your pregnancies. Knowing that ahead of time enables you and your health care provider to work together to decide on a treatment plan. When treatment begins early in pregnancy, it often can prevent symptoms of hypothyroidism from appearing.
You also should work with your health care provider to establish a timeline for follow-up care to check your thyroid function over time, even if you don't have any additional pregnancies. Some research has found that women who have a thyroid disorder that triggers symptoms during and after pregnancy also are at risk for developing other thyroid problems later in life. Regularly scheduled checkups can catch any additional thyroid dysfunction when it's still in the early stages and more easily treated.
©2019 Mayo Foundation for Medical Education and Research
Distributed by Tribune Content Agency, LLC.