Study finds youth suicide rates rise with community poverty levels
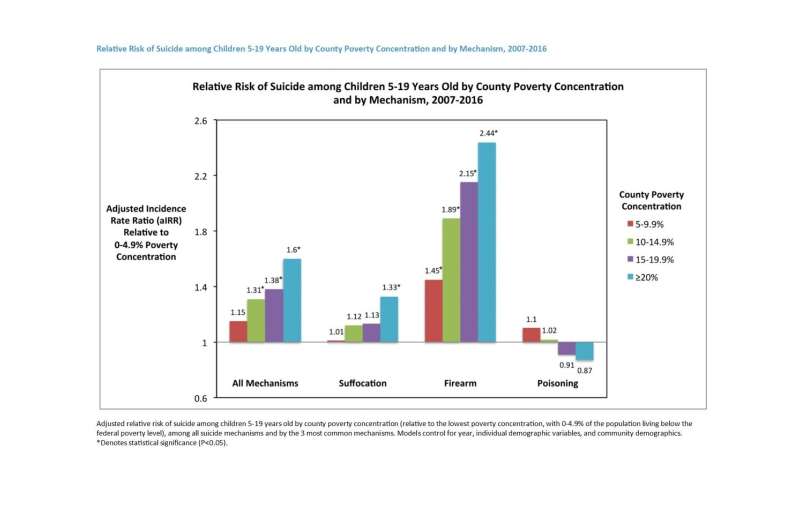
Research being presented at the American Academy of Pediatrics (AAP) 2019 National Conference & Exhibition shows that U.S. children living in counties with the highest poverty level are more than one-third more likely to die by suicide than those living in the least impoverished counties. The association is most pronounced for suicide by firearms.
An abstract of the study, "Pediatric Suicide Rates and Community-Level Poverty in the United States, 2007-2016," will be presented on Sunday, Oct. 27, at the Hilton New Orleans Riverside.
Youth suicide has nearly doubled in the last 10 years, making it the second leading cause of death for children and adolescents between ages 10 and 19 years old in the United States.
"Understanding risk factors for youth suicide is critically needed to inform prevention efforts," said abstract author Jennifer A. Hoffmann, MD, FAAP, a pediatric emergency medicine physician at Ann & Robert H. Lurie Children's Hospital of Chicago and an Assistant Professor of Pediatrics at Northwestern University Feinberg School of Medicine.
For the study, researchers conducted a retrospective, cross-sectional analysis of suicides among U.S. children ages 5-19 years old from 2007 to 2016 using Centers for Disease Control and Prevention and U.S. Census data.
Overall, the annual suicide rate was 3.4/100,000 children 5 to 19 years old. Of the 20,982 children between 5-19 years old who died by suicide during that time period, 85% were 15 to 19 years old, 76% were male, and 69% were Caucasian.
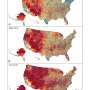
The researchers then divided counties into five poverty concentration categories, ranging from 0% to 20% or more of the population living below the federal poverty level. Controlling for variables including the year, demographics of the children who died (age, sex, and race), county rural-urban classification, and community demographics (county age, sex, and racial composition), the researchers found that counties with greater than 10% poverty concentration had a higher incidence of suicide compared to the lowest poverty concentration counties (0-4.9%). Suicide rates continued to rise with increased poverty concentration, with children living in counties with the highest poverty concentration (greater than 20% of the population living below the federal poverty level) being 37% more likely to die by suicide than youth living in the least impoverished counties.
The researchers also performed subgroup analyses for the three most common suicide mechanisms: suffocation (including hanging), firearms, and poisoning. Suicide rates from hanging and overdoses were not different between the different county poverty levels. Among firearm suicides, the suicide rate increased with increasing poverty concentration, relative to the lowest poverty concentration counties.
Dr. Hoffmann calls for additional research into the association between youth suicide and poverty.
"We need to figure out why children living in higher poverty communities are at increased risk for suicide," she said. "It could be related to unsafe gun storage, limited access to mental health care, or the build up of chronic stressors that children in poverty experience throughout the lifespan."
More immediately, Dr. Hoffmann said the findings suggest a need to target pediatric suicide prevention strategies in high poverty areas, including firearm suicide prevention.
"The majority of teen suicides by firearm occur in the home with a firearm owned by an adult in the home. Safe firearm storage (keeping the gun unloaded and locked separately from the ammunition) has been shown to decrease youth firearm suicide," Dr. Hoffmann said. Safely storing dangerous medications is another proven way to help decrease suicide risk among children.
Dr. Hoffmann also recommends parents keep an open line of communication with their children.
"Parents should not be afraid to have a conversation with their child about mental health and suicide. Talking about mental health openly decreases stigma and may allow a child to access help before it's too late," she said.
More information: Abstract Title: Pediatric Suicide Rates and Community-Level Poverty in the United States, 2007-2016