Improving drug delivery for brain tumor treatment
Despite improvements in drug delivery mechanisms, treating brain tumors has remained challenging.
Costas Arvanitis, of Georgia Institute of Technology, studies the processes affecting therapeutic drug penetration into brain tumors. He will present two strategies for improving the delivery of therapeutic agents during a session at the 178th Meeting of the Acoustical Society of America, which will take place Dec. 2-6, at the Hotel del Coronado in San Diego.
The talk, "Controlled drug delivery and release in brain tumors with focused ultrasound," was presented Monday, Dec. 2 as part of the session on cavitation nuclei.
"For a bloodborne therapeutic agent to be effective, it must cross the blood vessel wall to reach cancer cells in adequate quantities," said Arvanitis. "However, tumors can thwart their effectiveness in many ways."
While tumors are known to compromise the integrity of the blood brain barrier—a specialized vessel wall evolved to keep the brain "safe"—the makeup of the barrier is inconsistent, which prevents drugs from being uniformly distributed throughout the tumor. Unfortunately, increasing dosages to help improve drug delivery is not possible due to the adverse effects caused by drug interactions with healthy tissue, and drug penetration to the tumor core remains limited.
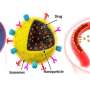
"To overcome these obstacles, new nanoparticle drug formulations that are associated with lower toxicity and clearance times have been proposed," he said. "Despite progress, improved nanoparticle penetration into brain tumors remains a major challenge."
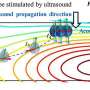
By combining focused ultrasound methods with different nanoparticle formulations, Arvanitis and his students, Yutong Guo and Chulyong Kim, have investigated two strategies for improving drug penetration into brain tumors. One approach is to use microbubbles to help overcome vascular barriers within the brain tumors and improve nanoparticle penetration across the vessel wall. The second method uses ultrasound in combination with temperature-sensitive nanoparticles. In this approach, ultrasound is used to trigger the release of the encapsulated drug only within the tumor, thereby locally increasing the drug effectiveness.
"While these concepts have been around for some time, our mechanistic investigations not only explain and underscore the potential of combining focused ultrasound with different nanoparticle formulations to treat brain cancer but also lay the groundwork for more rational design and deeper understanding of focused ultrasound-based treatment," Arvanitis said. "Our results demonstrate that these therapeutic strategies can provide unique opportunities to improve the delivery of nanoparticles and their cargo in the brain and brain tumor microenvironment."
More information: Arvanitis' presentation 1aBAb6, "Controlled drug delivery and release in brain tumors with focused ultrasound," Monday, Dec. 2, in the Hanover room of the Hotel del Coronado in San Diego.