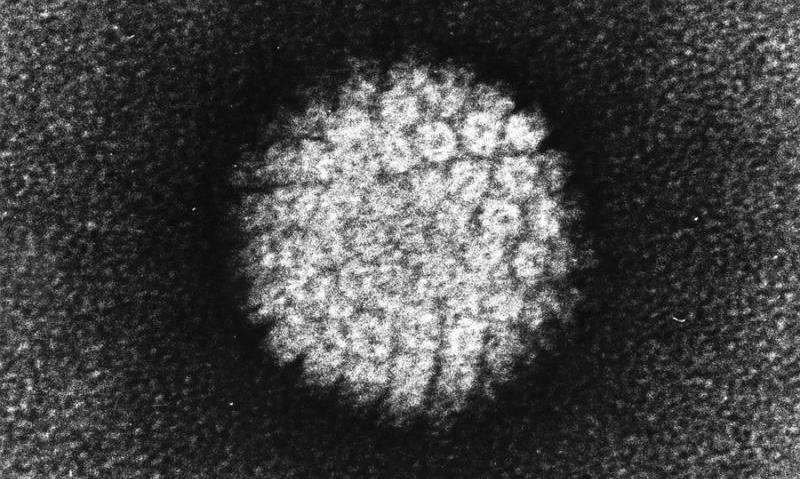
Electron micrograph of a negatively stained human papilloma virus (HPV) which occurs in human warts. Credit: public domain
A health economic model suggests that extending the U.S. human papillomavirus (HPV) vaccination program to include women and men through age 45 would produce relatively small health benefits compared with the current immunization program. Findings from a modeling study are published in Annals of Internal Medicine.
In October 2018, the U.S. Food and Drug Administration expanded the approved age range for use of the 9-valent HPV vaccine from 9 through 26 years to 9 through 45 in women and men. Among other considerations for policy recommendations is the potential for population-level health benefits relative to the increased costs.
Researchers used publicly available data to develop a model that would evaluate the added population-level effectiveness and cost-effectiveness of extending the current U.S. HPV vaccination program. Different strategies were compared with routine vaccination of all adolescents at age 11-12 years and vaccination through age 26 for women and 21 for men who were not vaccinated previously. The model showed that the current vaccination strategy in the U.S. will substantially reduce HPV-associated diseases and is cost saving, whereas vaccinating mid-adult women and men through age 45 years is predicted to produce small additional reductions in HPV-associated diseases and result in substantially higher cost-effectiveness ratios than the current recommendations.
These findings suggest that policies extending HPV vaccination programs to include middle-aged adults may produce relatively small population benefit.
More information: Annals of Internal Medicine (2019). http://annals.org/aim/article/doi/10.7326/M19-1182
Journal information: Annals of Internal Medicine
Provided by American College of Physicians