World's first congenital pituitary hypoplasia model developed using patient-derived iPS cells
Researchers at Kobe University's Graduate School of Medicine have developed the world's first congenital pituitary hypoplasia (CPH) model using patient-derived iPS cells. The research group consisting of Associate Professor TAKAHASHI Yutaka, medical researcher Matsumoto Ryusaku and Professor Aoi Takashi et al. succeeded in using the model to illuminate the mechanisms underlying CPH. The team has been attempting to apply this model to other pituitary diseases and drug discovery.
The results of this study were published in the American scientific journal J Clinical Investigation on December 17, 2019.
Research Background
Hypopituitarism caused by CPH is not uncommon and it is sometimes life-threating. Patients with this disease require lifelong hormone replacement therapy. The causes and underlying mechanisms are not well understood.
Prior research on pituitary diseases has been mainly conducted using animal models, such as knock out mice. However, sometimes there are differences in the phenotypes between animal and human. This means that human models are necessary in order to fully understand the mechanisms of such diseases.
In recent years, iPS (induced pluripotent stem) cells have been utilized in the development of disease models, regenerative medicine, and drug discovery. In addition, a method using iPS cells to induce differentiation of both the pituitary and hypothalamus in vitro has been developed; however it had yet to be applied to pituitary disease modeling.
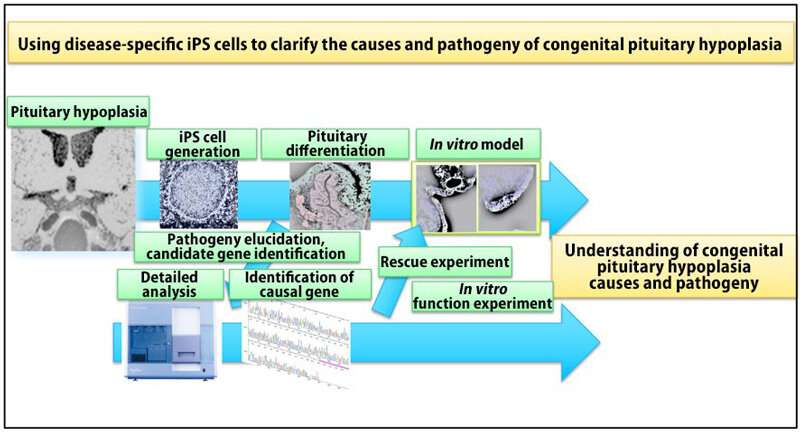
With this in mind, researchers at Kobe University's Graduate School of Medicine have applied this strategy to develop a human model of CPH in vitro using iPS cells to understand the pathophysiology and causes of the disease.
Research Methodology
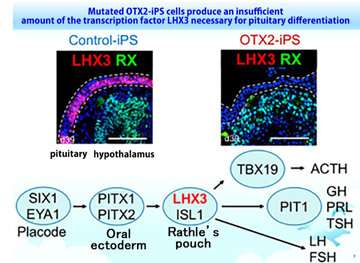
iPS cells were generated from blood samples taken from a patient with CPH. This patient exhibited congenital pituitary hypoplasia and was undergoing pituitary hormone replacement therapy. These patient-derived iPS cells were utilized to elucidate the underlying mechanisms in vitro. Interestingly, control iPS cells differentiated into hormone-producing cells; however, the CPH patient-derived iPS cells were not able to differentiate into these cells. Further analysis of the differentiation process revealed that the transcription factor LHX3, which is essential for pituitary differentiation, was not expressed in the pituitary progenitor from patient-derived iPS cells. Exome sequencing analysis revealed a mutation in the OTX2 gene and that its function was impaired. Correction of the OTX2 mutation in patient-derived iPS cells restored the pituitary differentiation ability, demonstrating that the OTX2 mutation was responsible.
Interactions between the pituitary and the adjacent hypothalamus are essential for pituitary differentiation and regulation. An advantage of this model is that it can simultaneously develop the pituitary and hypothalamus in vitro from iPS cells. This allowed the researchers to investigate the significance of interaction between these tissues. They clarified that the hypothalamus was responsible for the disease by performing chimera formation experiments using both patient-derived iPS cells and healthy iPS cells. Subsequent analysis exhibited that FGF10 (fibroblast growth factor 10) from the hypothalamus plays a pivotal role in the expression of the transcription factor LHX3 in the pituitary. Furthermore, expression levels of LHX3 were restored by adding FGF10 in vitro. These results demonstrated that FGF10 deficiency in the hypothalamus associated with OTX2 mutation was responsible.
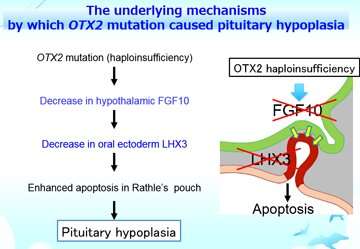
Collectively, the OTX2 mutation caused a decrease in hypothalamic FGF10, resulting in a lack of LHX3 expression in the oral ectoderm, which is the precursor of the pituitary. Consequently, loss of LHX3 caused apoptosis of the precursor cells, therefore causing the impaired development of the pituitary. These underlying mechanisms were illuminated for the first time by this study.
This pituitary disease model utilizing human iPS cells has elucidated the detailed underlying mechanisms, which animal models were unable to reveal.
Further Research
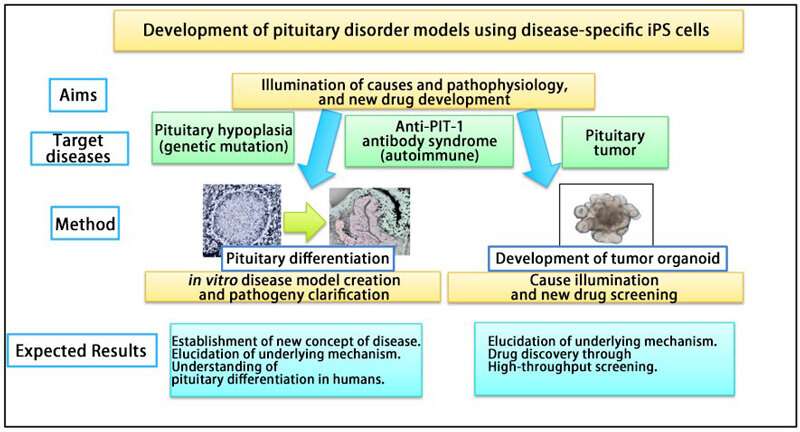
This research revealed the pathophysiology of CPH through disease-specific iPS cells. Furthermore, the model was also useful for understanding the pituitary differentiation process in humans.
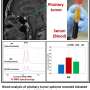
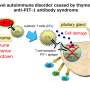
This research team is also investigating the causes, pathogenesis and treatment of other pituitary diseases (such as autoimmune disorders and pituitary tumors) using the same strategy. In particular, they are continuing to develop pituitary disease models to investigate the pathophysiology and precise mechanisms underlying the 'Anti-PIT-1 antibody syndrome,' which is a novel type of autoimmune pituitary disease that the team has established as a new clinical entity. Using this model, they have already demonstrated the antigen presentation of PIT-1 protein epitope on the anterior pituitary cells derived from patient iPS cells.
In addition, there are many other incurable pituitary diseases, for which the causes remain unknown. It is hoped that these iPS cell-based research methods for the diseases will lead to the clarification of the underlying mechanisms and drug discovery.
More information: Ryusaku Matsumoto et al, Congenital pituitary hypoplasia model demonstrates hypothalamic OTX2 regulation of pituitary progenitor cells, Journal of Clinical Investigation (2019). DOI: 10.1172/JCI127378