Aggressive features in some small thyroid tumors increase the risk for metastasis
Although papillary thyroid carcinoma is the most common form of thyroid malignancy, it is considered to be an indolent disease that progresses slowly and has an excellent prognosis. Patients, therefore, may be monitored on a regular basis rather than undergo a surgical procedure at the outset. But results from a new large-scale study show that in nearly 20 percent of patients, papillary thyroid tumors less than 1 cm in size had pathological signs of more aggressive disease that increased the risk that these patients might develop distant metastasis (spread of the disease to other areas of the body away from the primary site of cancer). The study demonstrates the need for developing sophisticated tests that will find patients with these pathological signs early on and for them to be counseled on all treatment options, including immediate surgical removal of part or all of the thyroid gland. The research study appears in an "article in press" on the Journal of the American College of Surgeons website in advance of print.
Thyroid carcinoma is the most common malignancy of the endocrine system, and the papillary form of the disease accounts for 70 to 90 percent of these malignancies. Papillary thyroid microcarcinoma (PTMC) is a specific subgroup of papillary thyroid carcinoma that accounts for 30 percent of all papillary thyroid malignancies.
The prognosis for patients with PTMC is good; the disease is responsible for only 3 percent of all deaths from thyroid cancer and 5 percent of deaths of patients with papillary thyroid carcinoma.2 The indolent course of the disease is shown by the relatively high prevalence of PTMC in autopsies of individuals who died of other causes (3 to 36 percent) and comparable clinical outcomes for patients whether they underwent an operation or not. The American Thyroid Association's 2015 guidelines for treatment of PTMC support surgical removal of the thyroid gland of patients with PTMC. The guidelines also, however, discuss active surveillance or regular intensive monitoring and repeat testing, and at least one clinical trial recommended observation of patients with PTMC.
Patients with suspected PTMC typically have preoperative ultrasound or biopsy. However, pathological features of aggressive disease can be found only on a full examination of tissue removed at the time of surgery.
"In general, PTMC tumors are not aggressive and not likely to affect overall survival. However, there are subsets within the patient population who may develop more serious cancers that could be life-threatening. With that in mind, we looked specifically at the risk of distant metastasis and the pathological profiles of patients with PTMC," said lead author of the study Zaid Al-Qurayshi, MD, MPH, department of otolaryngology-head and neck surgery, University of Iowa Hospitals and Clinics, Iowa City.
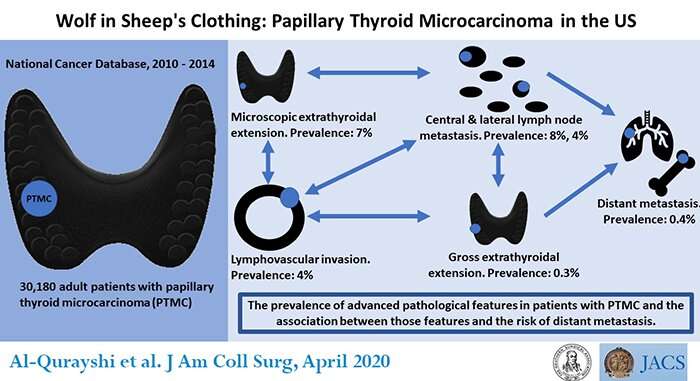
The researchers retrospectively analyzed 30,180 adult patient records in the National Cancer Database (NCDB) who were treated for PTMC between 2010 and 2014. NCDB is a joint program of the Commission on Cancer of the American College of Surgeons and the American Cancer Society. Among these patients, 5,628 (18.7 percent) exhibited pathological signs of advanced disease, such as central lymph node metastasis (8 percent), lateral lymph node metastasis (4.4 percent), microscopic disease outside of the thyroid (6.7 percent), gross disease outside the gland (0.3 percent), invasion of the lymphatics and blood vessels (4.4 percent), and distant metastasis (.04 percent).
The presence of some of these pathological features was associated with spread of the disease or a lower survival rate. "The death rate for patients with disease in the lymph nodes was 3 times higher, and it was 6 times higher for those with distant metastasis or spread to the lungs," said Emad Kandil, MD, FACS, a study coauthor and a professor of surgery in the department of surgery, Tulane University School of Medicine, New Orleans, La.
"Having a lymph node metastasis triples the risk of having distant metastasis. Extrathyroidal extensive has a 5-fold risk of spreading to the lymph nodes and a 9-fold risk of distant metastasis. These factors are all connected," Dr. Kandil said.
"The study provides a good, general perspective about the landscape of PTMC. More granular, clinical data are needed to help understand the risk factors for advanced disease and develop a preoperative test that could identify these patients who have them," Dr. Al-Qurayshi said.
Dr. Kandil's laboratory is currently testing a panel of genes that may tell which cancers will progress and which will not. In the meantime, all patients with PTMC should be carefully counseled.
"We don't have enough information at this time to confirm how the disease may progress. However, we do need to let patients know about the possible presence of aggressive disease and all their options for treatment," Dr. Kandil concluded.
More information: Zaid Al-Qurayshi et al. A Wolf in Sheep's Clothing: Papillary Thyroid Microcarcinoma in the US, Journal of the American College of Surgeons (2020). DOI: 10.1016/j.jamcollsurg.2019.12.036