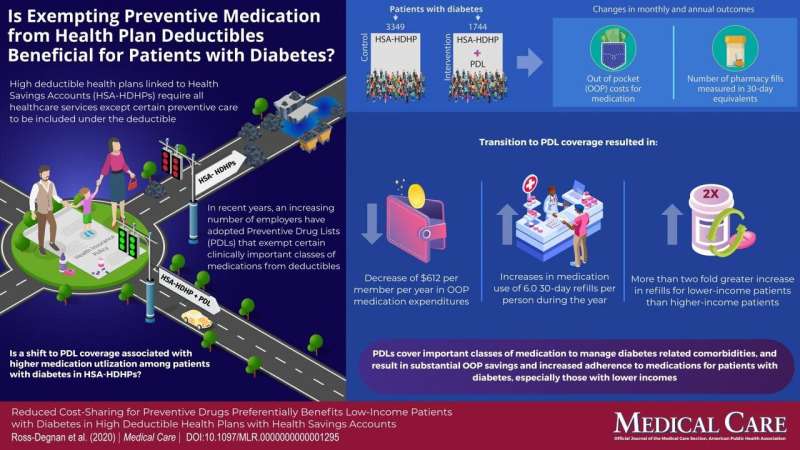
For patients with diabetes -- especially those with lower incomes -- preventive drug lists (PDLs) of essential medications available with no deductible can reduce out-of-pocket costs while increasing use of important treatments, reports a study in a June supplement to Medical Care. The journal is published in the Lippincott portfolio by Wolters Kluwer. Credit: Ross-Degnan et al. (2020) / Medical Care / DOI: 10.1097/MLR.0000000000001295
For patients with diabetes—especially those with lower incomes—preventive drug lists (PDLs) of essential medications available with no deductible can reduce out-of-pocket costs while increasing use of important treatments, reports a study in a June supplement to Medical Care.
The special issue presents a series of "natural experiments"—evaluating how changes in healthcare policy or practice affect real-world outcomes in patients with diabetes—from the Natural Experiments for Translation in Diabetes 2.0 (NEXT-D2) Network. "Natural experiments are permitting us to take advantage of the rapid proliferation of big data to rigorously study the impact of policies that otherwise would go unevaluated," comments Edward Gregg, Ph.D., of Imperial College, London, one of the co-leaders of the NEXT-D2 Network.
As Out-of-Pocket Costs Go Down, Use of Essential Treatments Goes Up
A growing number of Americans are covered by high-deductible health plans (HDHPs) - insurance plans with annual deductibles of $1,000 or higher—designed to reduce unnecessary care and promote higher-value care. But HDHPs include annual deductibles, copayments and other forms of cost-sharing, which can adversely impact treatment for diabetes and other chronic diseases, including use of needed medications. Adverse effects on medication use may be particularly large in federally regulated HDHPs linked to Health Savings Accounts (HSAs) that require patients to pay the full cost of medications until their annual deductible amounts are met.
To address this issue, some employers and insurers have developed PDLs specifying medications exempt from deductibles or copayments. Dennis Ross-Degnan, ScD, and colleagues of Harvard Medical School and Harvard Pilgrim Health Care Institute, Boston, evaluated a natural experiment to determine how these PDLs have affected out-of-pocket costs and use of clinically essential medications for patients with diabetes.
The study included 1,744 patients with diabetes enrolled in HDHPs with HSAs, whose employers switched all employees to PDL coverage. The switch meant that key medications and supplies for preventing the long-term adverse effects of chronic illness—including antidiabetic drugs, insulin, test strips, and blood pressure- and cholesterol-lowering drugs—became available with no or limited cost-sharing.
Analysis of insurance claims found that the PDLs led to a significant decrease in out-of-pocket medication costs: an average savings of $612 per year for patients with diabetes. This was accompanied by a sharp increase in preventive medication use: an average of six additional medication refills per year.
The increase in prescription refills was much larger for lower-income patients, for whom high cost-sharing may have been an important reason for previous underuse. The researchers also noted: "Overall savings in out-of-pocket spending were much larger for patients with severe diabetes, primarily due to savings on insulin."
'What Works' in Diabetes Management—NEXT-D2 Papers Provide Insights
There are many promising strategies to improve care and prevent complications for the millions of Americans affected by diabetes. The eight NEXT-D2 projects in the special issue address initiatives related to health insurance expansion, including Medicaid expansion and community health centers; healthcare financing and payment models, such as HDHPs and new Medicare/Medicaid initiatives; and innovations in care coordination for patients with diabetes.
"These and other natural experiments in the NEXT-D2 collaboration are using existing health data to fill the knowledge gaps in terms of what works for preventing diabetes and its complications," Dr. Gregg adds. NEXT-D2 is co-sponsored by the Centers for Disease Control and Prevention, the National Institute of Diabetes and Digestive and Kidney Diseases, and the Patient-Centered Outcomes Research Institute.
More information: Edward W. Gregg et al. Filling the Public Health Science Gaps for Diabetes With Natural Experiments, Medical Care (2020). DOI: 10.1097/MLR.0000000000001330
Journal information: Medical Care
Provided by Wolters Kluwer Health