Passive immunization may slow down SARS-CoV-2, boost immunity in patients, buy time for vaccine
Using antibodies from recovered patients has been life-saving for other acute infections and should be explored in response to COVID-19, researchers say in the International Journal of Risk & Safety in Medicine.
The worldwide COVID-19 pandemic has infected more than 4 million people and killed close to 280,000. Finding a vaccine has become a global public health priority. However, creating a viable vaccine might take a long time; scientists estimate a vaccine may be available in between 12 and 18 months. A potential interim solution reported in the International Journal of Risk & Safety in Medicine may be a passive vaccine, or passive immummization (PI), which can provide instant, short-term fortification against infectious agents.
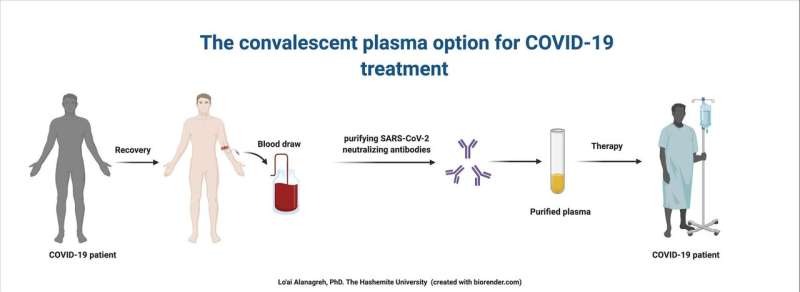
"Using valuable plasma from recovered patients might be useful in our global war against COVID-19," explained Foad Alzoughool, Ph.D. He and his co-author, Lo'ai Alanagreh, Ph.D., both of the Department of Laboratory Medical Sciences, Faculty of Applied Medical Sciences, The Hashemite University, Jordan, have studied the application of PI in previous pandemics and conclude that this approach is a potential solution to address the immediate health threat of COVID-19.
After exposure to a viral infection, an individual's body creates antibodies to fight off the virus. These antibodies in the blood of a recovered patient can be collected as convalescent plasma and transferred to the blood of a newly infected patient where it can neutralize the pathogen, eliminate it from the blood stream, and boost immunity. While PI does not provide long-term protection against the virus, it can reduce the aggressiveness and mortality of an infection.
The use of PI immunization dates to the beginning of the twentieth century during the Spanish flu epidemic, when patients who received convalescent plasma serum had lower mortality rates than others. Experimental usage of PI during outbreaks of Ebola virus, chikungunya virus and the H1N1 flu also shows the potential of using PI in the prevention and treatment of viral infecitions.
There is evidence as well of the effectiveness of the PI technique in the SARS-CoV epidemic in Guandong, China and the MERS-CoV in Saudi Arabia, particularly if it is introduced soon after symptom onset. In one report, patients who received PI had a significantly shorter hospital stay and lower mortality than other groups. In another, patients who received convalescent plasma before day 14 of illness had a higher discharge rate. Healthcare workers who were infected with SARS-CoV and failed to respond to treatment survived after transfusion with convalescent plasma.
"If you are looking for COVID-19 treatment, you will find it in the blood of survivors," said Dr. Alanagreah. "In a time when no registered antiviral drug or vaccine is available, PI might help in slowing down the deadly virus and save lives, particuarly for the elderly and patients with pre-existing conditions."
More than 1.5 million people have recovered from the disease, and many of them would be willing to donate plasma to help slow down the pandemic. Dr. Alzoughool and Dr. Alanagreh noted, importantly, that practicing this method now will help health systems be prepared in case a second wave of disease occurs.
More information: Foad Alzoughool et al. Coronavirus drugs: Using plasma from recovered patients as a treatment for COVID-19, International Journal of Risk & Safety in Medicine (2020). DOI: 10.3233/JRS-201017