How chemicals like PFAS can increase your risk of severe COVID-19

Nearly a year before the novel coronavirus emerged, Dr. Leonardo Trasande published "Sicker, Fatter, Poorer," a book about connections between environmental pollutants and many of the most common chronic illnesses. The book describes decades of scientific research showing how endocrine-disrupting chemicals, present in our daily lives and now found in nearly all people, interfere with natural hormones in our bodies. The title sums up the consequences: Chemicals in the environment are making people sicker, fatter and poorer.
As we learn more about the novel coronavirus and COVID-19, research is revealing ugly realities about social and environmental effects on health—including how the same chronic illnesses associated with exposure to endocrine-disrupting compounds also increase your risk of developing severe COVID-19.
In the U.S. and abroad, the chronic disease epidemic that was already underway at the start of 2020 meant the population entered into the coronavirus pandemic in a state of reduced health. Evidence is now emerging for the role that environmental quality plays in people's susceptibility to COVID-19 and their risk of dying from it.
Why endocrine disruptors are a problem
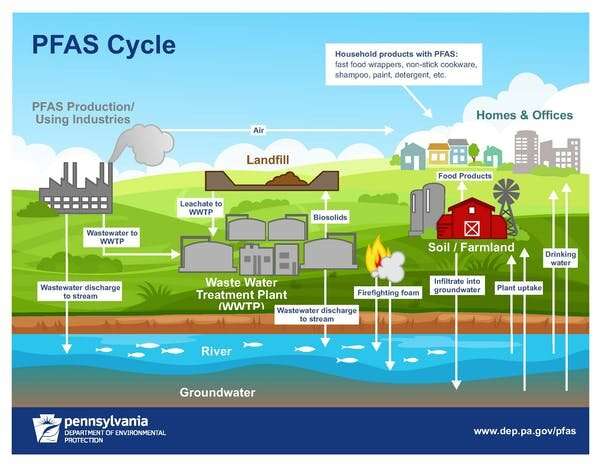
Endocrine-disrupting compounds, or EDCs, are a broad group of chemicals that can interfere with natural hormones in people's bodies in ways that harm human health. They include perfluoroalkyl and polyfluoroalkyl substances, better known as PFAS, flame retardants, plasticizers, pesticides, antimicrobial products and fragrances, among others.
These chemicals are pervasive in modern life. They are found in a wide range of consumer goods, food packaging, personal care products, cosmetics, industrial processes and agricultural settings. EDCs then make their way into our air, water, soil and food.
Research has shown that people who are exposed to EDCs are more likely than others to develop metabolic disorders, such as obesity, Type 2 diabetes and high cholesterol, and they tend to have poorer cardiovascular health.
EDCs can also interfere with normal immune system function, which plays a critical role in fighting off infection. Poor immune function also contributes to pulmonary problems such as asthma and chronic obstructive pulmonary disease; autoimmune diseases like rheumatoid arthritis and Crohn's disease; and metabolic disorders. Many EDCs are also associated with different cancers.
EDCs can mimic human hormones
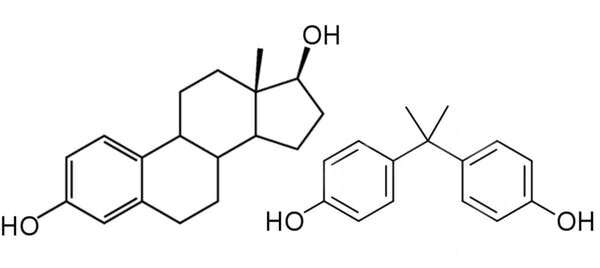
EDCs affect human health by mimicking our natural hormones.
Hormones are chemical signals that our cells use to communicate with one another. You might be familiar with reproductive hormones—testosterone and estrogen—which help distinguish male and female physiology and reproduction. Yet, hormones are responsible for maintaining virtually all essential bodily functions, including metabolism and healthy blood pressure, blood sugar and inflammation.
The chemical shape or structure of EDCs resembles hormones in ways that cause the body to misinterpret an EDC for a natural signal from a hormone.
Because the human body is very sensitive to hormones, only small amounts of hormones are required to convey their intended signal. Therefore, very small exposures to EDCs can have dramatic, adverse affects on people's health.
Environmental quality and COVID-19
Researchers are only just beginning to paint a picture about how environmental quality contributes to COVID-19 susceptibility, and there is much we still don't know. However, scientists suspect that EDCs can play a role based on clear scientific evidence that EDCs increase people's risk of developing chronic disease that put people at greater risk from COVID-19.
Public health organizations such as the U.S. Centers for Disease Control and Prevention and the World Heath Organization officially recognize underlying health conditions—including obesity, diabetes, hypertension, cardiovascular disease, immunosuppression, chronic respiratory disease and cancer—as risk factors for critical illness and mortality from COVID-19.
Scientific evidence shows that EDC exposure increases people's risk of developing all of these conditions. Scientists are thinking about these connections, and research efforts are underway to answer more questions about how EDCs may be influencing the pandemic.
Air pollution and other environmental risks
In addition to EDCs, other environmental conditions are also likely playing a role in the COVID-19 pandemic. For example, multiple studies have reported increased risk of COVID-19 illness and deaths. The findings are consistent with those reported in China following the SARS outbreak in 2002-2003.
Recent evidence also shows that COVID-19 infection can lead to lingering health conditions, including heart damage. Environmental conditions such as heat waves are particularly dangerous for individuals with heart disease or heart damage. In places like California that are currently experiencing wildfires and heat waves, we can clearly see how multiple environmental conditions can combine to further increase risk of deaths associated with COVID-19.
In the U.S., regulations such as the Clean Water Act and Clean Air Act have improved environmental quality and human health since the 1970s. However, the Trump administration has been trying to weaken them.
In the past three and a half years, about 35 environmental rules and regulations pertaining to air quality or toxic substances like EDCs were either rolled back or are in the process of being removed, despite unambiguous evidence showing how poor environmental quality harms human health. Allowing more pollution threatens to exacerbate the trend toward a sicker, fatter and poorer America at a time when people's overall health is necessary for our collective resilience to COVID-19 and future global health challenges.
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()