With 250,000 US deaths, COVID-19 is triggering more end-of-life planning—and young people want in on the discussions
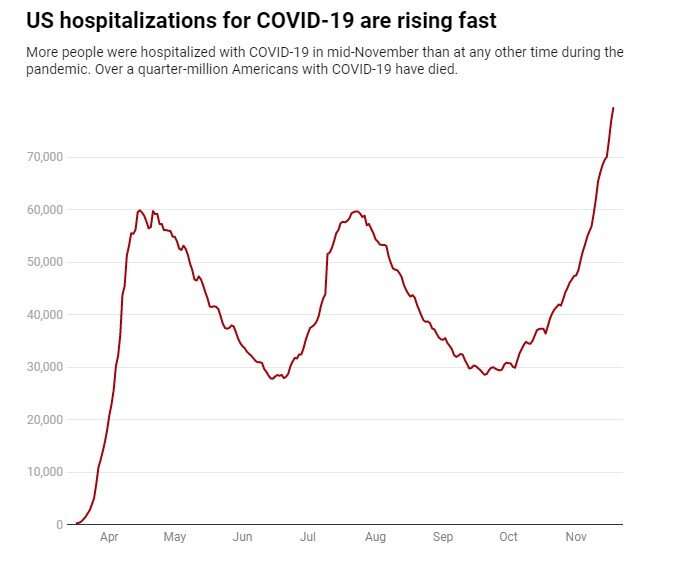
In homes across the U.S., families increasingly know someone who has been sick or hospitalized with COVID-19. The death toll passed a quarter-million Americans on Nov. 18, less than 10 months into the pandemic.
With health officials issuing stark warnings about the coronavirus's spread, studies show more people are thinking about end-of-life decisions and seeking advice on advance care planning.
Everyone directly affected by these choices should be part of the conversation—including young adults.
Advance care planning allows people to make health care choices before they become ill, such as whether they would want to be on life support and who should make health care decisions for them if they can't. The pandemic is now raising difficult new questions, as well, and for younger people. For example, if you were allowed only one visitor in the hospital, who should it be? And if you can't care for yourself after you leave the hospital, where would you want to live?
My colleagues and I have found that young adults, who are often shielded from these discussions, want to be involved, and we have some advice for how to go about it.
Young adults take health care planning seriously
For the past four years, I have taught a course called Ethics at the End of Life at the University of South Florida. When I was encouraged to offer this class, I thought I would need to win over students to the importance of the topic. Instead, many of them relate personally as caregivers for parents and grandparents. In fact, roughly 15% of family caregivers are between the ages of 18 and 25. Yet young adults are often overlooked when the topic of advance care planning arises.
Philip Barrison, one of my students, demonstrated young adults' interest in advance care planning in a recent study published in the American Journal of Hospice and Palliative Medicine. He presented voluntary advance care planning workshops to college students and surveyed them about their knowledge of the topic, their willingness to talk to others, and their actions after the workshops. Over 70 students participated in the workshops and learned from sources such as The Conversation Project and the National Academy of Medicine's "Dying in America" report.
Barrison found that young adults are more interested in advance care planning than older adults perceive, but they, like many adults, are also uninformed.
American health care culture emphasizes acute care in which a "do everything to save them" agenda is the default. Without knowing what "everything" means, families plead for physicians to save their loved ones, and patients often end up unconscious, connected to life-prolonging machines.
That can leave families with a cruel choice: let their loved one live the rest of his or her life in that state or sign a form removing the machine and ending a life. About 30% of adults over 65 are treated in intensive care in the month before they die.
Advance care planning can alleviate some of the anxiety associated with surrogate health care decision-making. In fact, the planning process itself, starting with family conversations, may provide more benefits by bringing people together than the formal advance care directives, such as living wills, do-not-resuscitate orders and medical power of attorney designations, that can come out of it.
How to start the conversation
The Netflix documentary Extremis explores the emotional trauma of choices for both families and health care workers. And books like Being Mortal by Atul Gawande, a member of Joe Biden's COVID-19 task force, have brought this challenge to light.
What has been missing is the importance of including young adults in end-of-life decisions and conversations. With many Americans waiting longer to have children and more older adults raising their grandchildren, more young adults are moving into decision-making roles for the aging population.
As blessings stand in stark relief against recent losses, this holiday season is an opportunity to discuss these important questions with the entire family.
Here are a few tips for starting the discussion:
- Frame the conversation around life rather than death. Many important comforts such as music, food and stories are enjoyable through the final moments of life, yet these may be missed if the focus is on dying rather than living.
- Initiate conversations by talking about your own wishes for how you would want to live if you were to develop a serious illness or have an accident. This may prompt others to express their similarities and differences.
- Create a written record of your conversations. These records can be developed into advance care directives—legal documents that typically require witness signatures or a notary. Checklists of questions to ask and tools for developing these documents are available online through sources like The Conversation Project, Five Wishes and The National Institute on Aging. There are also tools for children, adolescents and young adults with life-limiting illnesses.
- If you have documented a health care surrogate, be sure to talk with that person about what you do and do not want. Never assume someone will know how to make decisions for you. It's unfair to put someone you love in that position.
- Remember that people change over time. Think of these conversations as ongoing and revisit the topic on occasion to see if there are new thoughts or wishes that have emerged.
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()



















