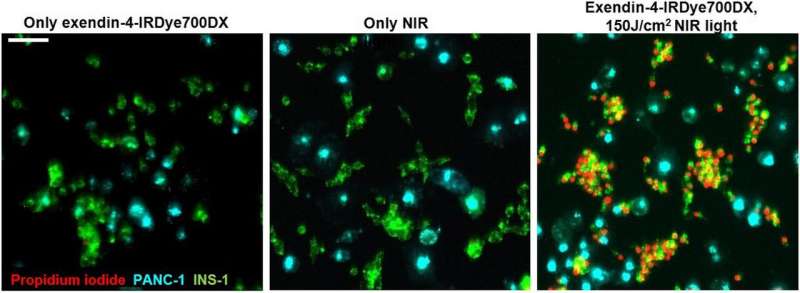
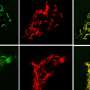
Fluorescence microscopy of INS-1 cells labeled with the fluorescent dye DiO (green) and PANC 1 cells labeled with the fluorescent dye DiD (cyan), co-cultured and incubated with propidium iodide (red), after incubation of exendin-4-IRDye700DX or only binding buffer and with and without NIR irradiation with a radiant exposure of 150 J/cm. The scale bar denotes 100 µm. Credit: Society of Nuclear Medicine and Molecular Imaging
A new method to treat hyperinsulinemic hypoglycemia has proven highly selective in targeting lesions and effective in slowing tumor growth, according to research published in the November issue of the Journal of Nuclear Medicine. The novel approach utilizes receptor-targeted photodynamic therapy with exendin-4-IRDye700DX to induce phototoxicity in insulin-producing cells that cause hyperinsulinemic hypoglycemia.
Insulin production by pancreatic beta cells is usually a well-regulated process; however, uncontrolled overproduction of insulin can arise. In adults, this overproduction is most often caused by insulin-producing lesions known as insulinomas. In newborn children, the most common cause of insulin overproduction is congenital hyperinsulinism. When this excessive insulin production causes dangerously low levels of blood glucose, hyperinsulinemic hypoglycemia occurs. Prolonged hyperinsulinemic hypoglycemia may lead to seizures, loss of consciousness, permanent brain damage or brain death.
"Treatment of hyperinsulinemic hypoglycemia is challenging," said Marti Boss, Msc, postdoctoral researcher in the department of medical imaging at the Radboud University Medical Center in Nijmegen, Netherlands. "Current treatment consists of invasive surgery, which comes with major risks of morbidity, and medication to treat hypoglycemic episodes, which is not always effective and causes side effects. Because of these challenges, a novel, minimally invasive treatment option for hyperinsulinemic hypoglycemia in adults and children is warranted."
To address this issue, cell and animal models were developed to bear the glucagon-like peptide 1 receptor (GLP-1R), which is expressed on pancreatic beta cells and in high levels on insulinomas. Researchers used receptor-targeted photodynamic therapy, coupling the light sensitive molecule IRDye700DX with the peptide exendin-4 (which specifically targets insulin-producing cells) to irradiate the GLP-1R cells and xenografts. The efficacy and specificity of receptor-targeted photodynamic therapy in causing cell death was measured in vitro. Tracer biodistribution, induction of cellular damage and the effect on tumor growth were measured in vivo to determine treatment efficacy.
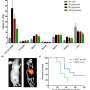
Receptor-targeted photodynamic therapy was found to cause significant specific phototoxicity in GLP-1R positive cells. In the animal model, the tracer accumulated dose-dependently in GLP-1R positive tumors. In vivo receptor-targeted photodynamic therapy also induced cellular toxicity in tumors without damaging the surrounding tissue, leading to a prolonged median survival.
"This technique provides the first evidence of the effectiveness of receptor-targeted photodynamic therapy, which has previously proven to be successful for several forms of cancer, for the treatment of insulin-producing lesions," remarked Boss. "In the future, this could provide a completely new, minimally invasive and highly specific treatment method for hyperinsulinemic hypoglycemia that would improve the clinical management of patients dramatically."
More information: Marti Boss et al, Receptor-Targeted Photodynamic Therapy of Glucagon-Like Peptide 1 Receptor–Positive Lesions, Journal of Nuclear Medicine (2020). DOI: 10.2967/jnumed.119.238998
Journal information: Journal of Nuclear Medicine
Provided by Society of Nuclear Medicine and Molecular Imaging