Autologous chondrocyte implantation in the knee: M-ACI has comparable benefit to therapy alternative
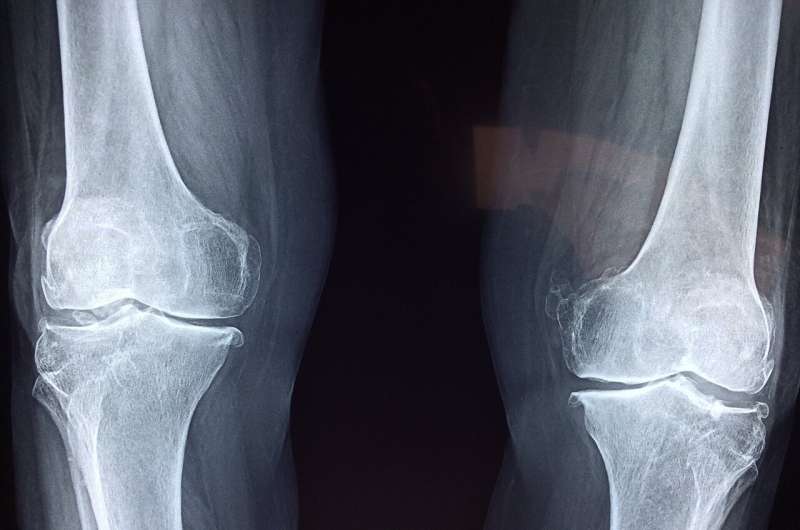
Autologous chondrocyte implantation (ACI) has been used in adults with deep cartilage defects for over 30 years and has been further developed and modified over time. For the most recent procedure, matrix-induced ACI (M-ACI), favorable effects have been shown suggesting that the benefits are at least comparable to those of therapy alternatives. No advantages are evident for the other two older procedures, collagen-covered ACI (ACI-C) and ACI with a periosteal flap (ACI-P)
This is the conclusion of the final report that the German Institute for Quality and Efficiency in Health Care (IQWiG) has now presented on behalf of the Federal Joint Committee (G-BA). The patient-relevant benefit of all three generations of ACI—ACI-P, ACI-C or M-ACI—was investigated.
Matrix-induced ACI offers technical advantages
ACI has been used in Germany for many years to treat cartilage defects in adults affecting more than 50 percent of the cartilage depth or extending into the underlying bone. Today, M-ACI is the most commonly used technique; according to several comments on the preliminary report, the two older procedures, ACI-C and ACI-P, no longer have any practical relevance.
In the two-stage procedure, cartilage is first removed, cultivated in a laboratory and then implanted into the defect in a second step. In M-ACI, the cultivated cartilage cells are directly fixed on a carrier matrix and reimplanted into the cartilage defect area. This technical progress supersedes the more complex fixation and watertight sealing of a cell suspension in the cartilage defect that is required with the older procedures—in the case of ACI-P using periosteum or in the case of ACI-C using a collagen membrane. Overall, M-ACI makes surgery much easier.
Favorable effects only with M-ACI
Based on a meta-analysis of the study data from seven RCTs, it can be assumed that the M-ACI procedure has a benefit at least comparable to that of therapy alternatives such as microfracturing or mosaicplasty: Statistically significant effects in favor of M-ACI were shown for knee function and health-related quality of life, but were not of a clinically relevant magnitude. The results for other outcomes also suggest almost without exception an advantage of M-ACI, so that overall a benefit for M-ACI at least comparable to the therapy alternatives can be determined.
The two older procedures, ACI-P and ACI-C, consistently produce worse results when examined individually: Based on partly inconsistent results from two RCTs on each procedure, neither a benefit of ACI-C and ACI-P is evident, nor can a comparable benefit to therapy alternatives be determined.