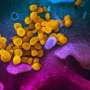
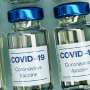
COVID-19 vaccines can cause side effects. Here's why that shouldn't stop you from getting the shots
A friend of Paul Offit's volunteered for one of the COVID-19 vaccine trials but, like everyone who participated, was not told whether he was injected with a placebo or the real thing.
The morning after getting the second dose, the North Carolina man woke up feeling crummy, with a headache and overall fatigue, and immediately called Offit. He was elated.
"He said 'Yes, I got the vaccine!'" recalled Offit, a prominent infectious-disease specialist at Children's Hospital of Philadelphia.
The man's unpleasant symptoms were a sign that the vaccine was working, said Offit, who spoke Wednesday on a webcast run by JAMA (the Journal of the American Medical Association). When his friend received the injections, cells in his immune system responded by sending out inflammatory warning signals, which in turn triggered the formation of antibodies and other customized defenses that would remain in his system should he ever encounter the actual virus.
But as with any vaccine, those inflammatory chemicals also can cause side effects. And therein lies the public health messaging challenge of the next few months.
Some people will experience side effects and conclude that the vaccine gave them COVID. Wrong. With the three vaccines for which results have been revealed so far—made by Pfizer, Moderna, and AstraZeneca—that is biologically impossible, for reasons we'll explain below.
Others may worry that the process was rushed, or that two of them consist of genetic molecules called messenger RNA —the first such vaccines that would be approved for general use. Fair questions. But the record speed in developing the drugs was made possible by massive government investment and technological advances that have been in the works for years—not because any corners were cut on safety, infectious-disease experts say.
Yes, some people will develop side effects. Most will be mild or moderate, disappearing within a day or two. There is no sign of any long-lasting complications. Given the alternative—risk of infection with a virus that, as Offit put it, "has brought us to our knees"—physicians say the vaccines are worth a bit of collateral unpleasantness.
Here's what to expect.
The complete safety data have not yet been disclosed, but preliminary results are encouraging.
With the vaccine made by Cambridge, Mass.-based Moderna, no significant safety concerns were identified in the first 15,000 people to get the injections. Most reported side effects occurred after the second dose: fatigue (in 9.7% of recipients), muscle pain (8.9%), joint pain (5.2%), headache (4.1%), and redness at the injection site (2%). Fewer than 2% have reported a high fever.
Among those who received the Pfizer vaccine, a joint effort with German firm BioNTech SE, 3.8% reported fatigue and 2% suffered a headache. More details are expected to be announced Tuesday, two days before the data are reviewed by an advisory panel of the U.S. Food and Drug Administration (Offit is a member).
It is likely that some volunteers experienced more than one of these side effects, said Seth Welles, a professor of epidemiology at Drexel University's Dornsife School of Public Health. In other words, we should not add up all those percentages to determine the likelihood of side effects. There is some overlap.
Still, let's say a total of 15% of recipients feel pretty awful for a day or two after getting their second dose. That will be millions of people. An employer with essential workers should take care not to vaccinate everyone at once, should some of them need to stay home for a day.
But a day off work is worth the trade-off, said Neil O. Fishman, an infectious-disease specialist and chief medical officer at the Hospital of the University of Pennsylvania. Preliminary trial results suggest the Moderna and Pfizer vaccines prevent 95% of COVID cases.
"I've seen what a world without vaccine looks like," Fishman said. "I've seen the death, I've seen the toll on the economy. I've seen the impact on our doctors, our nurses, their families, and the impact on the educational system and our children. When I look at the data that we have, it is very clear to me that the benefits of these vaccines far outweigh the risks."
Side effects from vaccines tend to emerge within a day or two—after a few weeks, at most. If any truly serious effects were to occur in the tens of thousands of volunteers in the various clinical trials, they would have been detected by now, said Welles, the Drexel epidemiologist.
It is possible that some rare side effect could emerge once larger numbers of people are vaccinated, say at a rate of 1 in 200,000 or 1 in a million, he said. But even in normal times, vaccine trials are conducted in far fewer than 100,000 volunteers, similar to what has happened this year.
And if you get sick after a vaccine, that is no proof that the injection was the culprit, Welles said. Establishing cause and effect is a question of math—is the apparent side effect happening any more often than in people who have not been vaccinated?—and biological plausibility.
The textbook example is Guillain-Barré syndrome, a neurological disorder that occurred in several hundred people who received a swine flu inoculation in 1976 and 1977—a vaccine developed in response to an outbreak of swine flu at Fort Dix, in New Jersey.
Guillain-Barré occurs when the immune system attacks the "peripheral" nervous system—nerve cells outside the brain and spinal cord—leading to muscle weakness and even paralysis.
For every 100,000 people who were vaccinated, epidemiologists determined that one additional case of Guillain-Barré occurred above the usual rate of this rare condition. And the link between cause (a ramped-up immune response) and effect was medically plausible.
But most medical conditions have no connection to vaccines. Robert Wachter, chair of the department of medicine at the University of California-San Francisco, worries that people will blame the COVID vaccines for such entirely unrelated maladies as cancer, heart attack, and stroke. In a long thread on Twitter, he warned:
"The vaccines will have zero to do with any of them."
Vaccine trials generally last for years. That's mainly to see how well, and how long, recipients are protected against disease, though scientists also watch for side effects.
Participants in the COVID vaccine trials will be followed for years, too. So how can scientists say already that the injections worked?
Call it the silver lining of living in a pandemic.
In normal times, it can take many months for enough cases of a disease to occur so that statisticians can determine whether people who get vaccinated are less likely to get sick than those who receive a placebo. But as COVID case numbers surged this fall, the answers came a lot faster.
In the case of Moderna, for example, 95 cases of disease were identified by mid-November out of 30,000 trial participants. In 90 cases, the person got the placebo—dramatic enough for researchers to conclude that the vaccine prevented most cases of disease.
The unusual speed with which these vaccines were developed was made possible for other reasons, too. Ordinarily, a drug company might wait months, even years, in between various regulatory hurdles before deciding to invest in manufacturing a vaccine.
But investments by multiple governments, such as the Trump administration's Operation Warp Speed, took much of the business risk out of the equation. Drug makers began gearing up months ago to make the vaccines in case they worked.
Lastly, technology speeded the process. The first two companies to report results, Pfizer and Moderna, made their vaccines with molecules called messenger RNA. They contain genetic instructions for human cells to make the "spike" protein: the little protrusions that form the namesake corona around each coronavirus particle.
Traditional vaccines consist of whole viruses that have been weakened or inactivated, prompting the immune system to make antibodies and other defenses called T-cells. But the Pfizer and Moderna results indicate that the spike protein alone is enough to prompt this protective response.
And by itself, a protein cannot cause infectious disease. "It is impossible" for these vaccines to cause COVID, said Fishman, the Penn physician.
The vaccine made by AstraZeneca, the third company to report results, delivers instructions for the spike in a different way: carried by another virus called an adenovirus. Those viruses, too, are unable to cause disease in humans, much less COVID itself.
If approved, the Pfizer and Moderna products will be the first RNA vaccines to be administered to the general public. But the basic science behind them has been going on for years, including a major hurdle that was cleared in 2005 by two of Fishman's Penn colleagues, immunologist Drew Weissman and Katalin Karikó, who is now at BioNTech.
The molecules are well-tolerated by the human body. And in any event, they don't stick around. Once it is used to make a protein, RNA is rapidly degraded. And it can't become part of your DNA.
Fishman is convinced the approach is rock-solid.
"To me, the most important measure of a vaccine is: Would I give it to my family?" he said. "I will give this vaccine to my wife and my children, and to me as soon as it is available."
©2020 The Philadelphia Inquirer, LLC. Visit at inquirer.com. Distributed by Tribune Content Agency, LLC.