New insights about age-related macular degeneration could spur better treatments

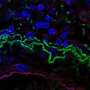
"Wet" age-related macular degeneration (AMD) is one of the most common causes of irreversible vision loss in the elderly, and it occurs when abnormal and leaky blood vessels form in the retina, in part due to inflammation. New research by investigators at Massachusetts General Hospital (MGH) reveals insights into potential drivers of the disease—which currently has no cure—that could be targeted through prevention or treatment strategies. The findings are published in eLife.
Two inflammatory pathways involving complement (which is an immune system component) and a protein complex called the inflammasome (which, as its name suggests, triggers inflammation) promote the formation of abnormal blood vessels that are hallmarks of wet AMD, but it's unclear how these pathways are activated. Previous studies suggest that the inflammasome may be activated by a protein called NLRP3, mainly in the retinal pigment epithelium of the eye (a cell layer that separates the vascular layer of the eye from the retina).
To investigate further, researchers conducted experiments in a mouse model of wet AMD. The team showed that inflammasome activation by NLRP3 occurs mainly in cells called macrophages and microglia, but not in the retinal pigment epithelium. The scientists also discovered that proteins other than NLRP3 can lead to inflammasome activation and worsening of wet AMD.
"This means that rather than targeting only NLRP3 in wet AMD, it may be beneficial to block essential proteins of the inflammasome instead that are required for its activation, independently of whether NLRP3 or other proteins initiate inflammasome activation," explains senior author Alexander G. Marneros, MD, Ph.D., a principal investigator at MGH's Cutaneous Biology Research Center and an associate professor of Dermatology at Harvard Medical School. "Our findings provide guidance on how to block inflammasomes in wet AMD."
Marneros notes that previous studies conducted in cells suggest that complement activation can in turn lead to inflammasome activation, but this study in mice found that this activation occurs largely independently from complement-mediated inflammation. "Our study in a mouse model defines the cell types that contribute to inflammasome-mediated inflammation in wet AMD and uncovers the specific roles and contributions of NLRP3 inflammasomes, non-NLRP3-inflammasomes, and complement for the manifestation of wet AMD," he says.
In addition to providing new insights into how inflammation is regulated in wet AMD, the study also suggests that novel therapies that block inflammasome-mediated inflammation could be improved when combined with treatments that inhibit complement-mediated inflammation. "A combined therapeutic approach that blocks both these inflammatory pathways is likely going to have synergistic effects in lessening the symptoms of wet AMD. Thus, our findings in this mouse model may have important clinical relevance for novel therapies for this common blinding disease," says Marneros.
More information: Jakob Malsy et al, Distinct effects of complement and of NLRP3- and non-NLRP3 inflammasomes for choroidal neovascularization, eLife (2020). DOI: 10.7554/eLife.60194