Credit: Pixabay/CC0 Public Domain
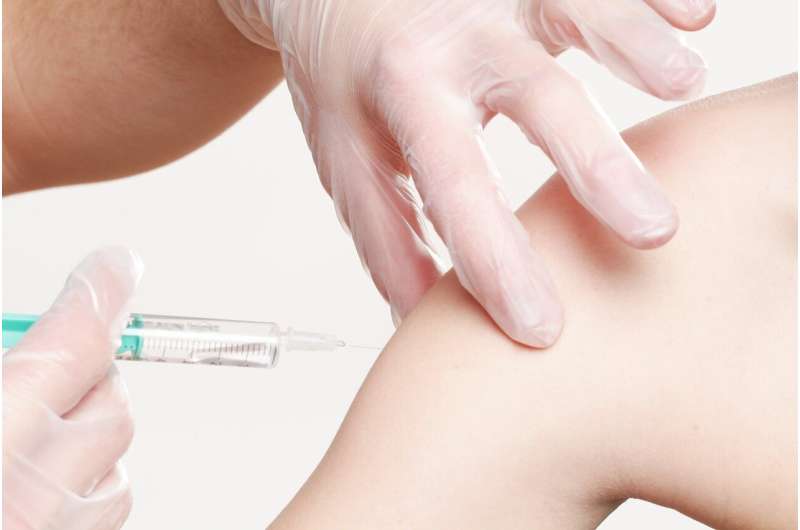
This week the COVID-19 vaccine by Pfizer and BioNtech has started to be injected into health care workers across the country after gaining emergency use approval from the federal government. While the vaccine was developed in a matter of months, it was based on decades of research.
Unlike traditional vaccines where a weakened or inactive form of the virus or pieces of a viral protein is injected into a person, the coronavirus vaccine utilizes messenger RNA technology. mRNA is a single-strand molecule of RNA that corresponds to the genetic sequence that codes for the production of proteins and can be used to transport information to a cell. Researchers first discovered mRNA in the late 1960s, but only within the past couple of decades has work been done to utilize the discovery to cure disease. This is the first time the federal government has approved usage of the technology in humans.
Sandro da Rocha, Ph.D., a director of the Center for Pharmaceutical Engineering and Sciences at Virginia Commonwealth University, researches nanomedicines for drug delivery including the use of RNA and said he believes the vaccine is safe and effective. The mRNA breaks down quickly and does not have a lasting impact on the body like something based on DNA.
da Rocha, a professor in the Department of Pharmaceutics at the VCU School of Pharmacy and in the Department of Chemical and Life Science Engineering at the VCU College of Engineering, is more concerned about people being willing to take the vaccine, not the mRNA itself. He discussed these concerns, and shared more about mRNA, in an interview with VCU News.
How does the vaccine technology work?
This new vaccine technology consists of a nanomedicine platform. You are basically getting mRNA and placing it in a nanoparticle, and you are using that to safely and effectively deliver the vaccine. This is my area of expertise—drug delivery. I work with various types of molecules but focus on treating cancer. [Editor's note: da Rocha conducts research in Developmental Therapeutics at VCU Massey Cancer Center.] I don't develop vaccines for cancer but the same technology can be used. This is technology that has been in the works for a long time, but it hasn't received approved until now as a vaccine.
When did research begin on mRNA in pharmaceuticals?
In the early 1990s mRNA was studied on how it could be used to produce proteins in the body. At that time, the biggest challenge was the fact that these break down very, very quickly. That is why the vaccine needs to be shipped at such low temperatures. The biggest challenge when doing any type of RNA vaccine is really getting the mRNA into the cytosol (the liquid found inside cells) while avoiding its exposure to our system. That is why in the 1990s people started to think about that. There was no technology for you to efficiently do this. That is where nanomedicine can contribute to the area. Some of our projects include figuring out ways to get RNA into cells.
What is the difference between a traditional virus-based vaccine and an mRNA vaccine?
You are not injecting any type of antigen in the body, so the body is not going to provide your response to the mRNA itself. This is different from the old virus technology that has the whole antigen there. The mRNA is different. It has to get into the cell and then uses the machinery in our cells to start producing proteins. In this particular case, the protein is called a "spike protein," which is seen in pictures of the COVID-19 virus. This spike protein will do the same job to stimulate the immune system as a vaccine that contains the virus itself. mRNA is non-infectious, and the cell will eventually break down the mRNA.
How was the mRNA vaccine developed so quickly?
This technology is much simpler than other vaccine technology. That is why it can be deployed so fast. I think the Moderna vaccine was a little over 60 days to "go" from the time they had the genetic sequence until they went to clinical trials. That speaks to the fact that this is a platform technology. You can quickly translate what people have learned before in terms of producing mRNA and preparing the nanomedicine.
Why is now the time when mRNA technology is being used?
It was the right opportunity to push that. The vast amount of studies with mRNA vaccines available today that show their safety, and the fast and straightforward production of these nanomedicines for quick deployment makes such vaccines ideal candidates for situations like this.
Do you have concerns about this new technology being used on such a large scale so quickly?
I do not. First and foremost I really trust the science. We are always looking at risk-benefits. Right now the benefits outweigh the risks tremendously. Right now, more people are dying of COVID-19 in a single day compared to all of those who died in 9/11 in the United States. There is always a risk, but this technology was really ripened for this time, especially mRNA. If it was something else, I would be a bit more cautious. But the mRNA breaks down quickly. The mRNA is there for a long enough time for your immune system to be primed and then [the mRNA] just goes away.
What about the side effects? People have reported getting COVID-like symptoms.
An immune response from the vaccine is to be expected. There are always people who would feel more of the response from the immune system. The recommendation is that when you get the shot, you are going to be monitored for 10 or 15 minutes before they let you go. That is because, like any type of drug, you can have an allergic reaction. I think that was reported in several cases of health care workers in the U.K. so it cannot be ignored. People can have adverse reactions but you cannot get COVID-19 from the vaccine.
What type of protection do you get from the vaccine?
The research is showing around 50% protection after the first shot and 95% after the second shot. That means you are 95% protected, but it is still debated whether you could have the virus and transmit it even after the vaccine. That is why they are saying to take the vaccine but don't go see [your] grandpa. The CDC still recommends you to wear a mask and stay six feet away even after the two doses of vaccine. They don't know if you can still pass it to someone else. The reality is we are still learning how this thing is transmitted.
What are the challenges faced when getting this to the general public?
The problem of shipping logistics and keeping it at cold temperatures can be solved. I think the biggest challenge is that right now a significant number of Americans says they are unsure if they are going to take the vaccine. Getting public trust is going to be a challenge. We at universities are going to have a role. We need to have campaigns, and having staff and students taking the vaccines once all the front-line personnel are vaccinated.
How much more safe will the public feel in six to 12 months?
That will depend on if we can convince 75-85% of the population to use the vaccine. That is where we get herd immunity. Eventually this vaccine is going to get to people even if it takes a little while. People not only need to get the first shot but they need to come back for the second shot.
What are the risks for older adults given they often have a weaker immune system?
That goes back to the risk-benefit. 0.6% of the population lives in a nursing home or assisted living facility but is responsible for 40% of [COVID-19] deaths. If you are an older person right now, my mom for instance, I would say it doesn't matter, go get the vaccine, go ahead and get the shot.
Provided by Virginia Commonwealth University