Reviving exhausted immune cells to fight cancer
Eliminating a single gene can turn exhausted cancer-fighting immune cells known as CD8+ T cells back into refreshed soldiers that can continue to battle malignant tumors, a new study led by UT Southwestern researchers suggests. The findings, published online this week in the Journal for Immunotherapy of Cancer, could offer a new way to harness the body's immune system to attack cancers.
In 2017, the Food and Drug Administration approved treatments involving chimeric antigen receptor T (CAR-T) cells, which consist of immune cells known as T cells that have been engineered to recognize specific proteins on the surface of cancer cells. When these cells are delivered by infusion, they mount a targeted immune response against cancer cells.
CAR-T cells have been successfully used to treat blood cancers such as leukemia and lymphoma, often with dramatic results, says Venuprasad Poojary, Ph.D., associate professor of internal medicine and immunology at UTSW. However, these treatments have had little success against solid tumors, such as those that develop in the colon, breast, and lung.
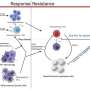
When CAR-T cells enter these solid tumors, Poojary explains, they quickly become dysfunctional and lose their cancer-fighting abilities. This state, referred to as "exhaustion," is accompanied by the addition of proteins, including PD1 and Tim3 on their surfaces and an inability to produce their usual immune-inciting molecules, such as Interferon-gamma and tumor necrosis factor. Finding a way to prevent CAR-T cells from becoming exhausted has become a significant goal in cancer research, Poojary adds.
Toward this end, he and his colleagues scoured published research comparing gene activity in working and exhausted T cells. The researchers quickly zeroed in on a gene called Cbl-b, which is more active, or upregulated, in exhausted cells.
Poojary and his colleagues confirmed that Cbl-b was activated in T cells that infiltrated tumors in a mouse model of colon cancer. Not only did these cells lose their tumor-fighting abilities, but they also developed a characteristic set of cell surface proteins and inability to produce, or express, immune molecules characteristic of exhaustion. However, when the scientists used the gene editing tool CRISPR to delete Cbl-b in these cells, they regained their cancer-fighting capacity and lost other exhaustion features.
Adding evidence to Cbl-b's key role in T cell exhaustion, the researchers used genetically altered mice in which this gene was shut down. When they transplanted cancer cells into these animals, the cells grew tumors markedly smaller than in cancer cells of mice with active Cbl-b.
Further experiments showed that removing Cbl-b also prevented exhaustion specifically in CAR-T cells, Poojary adds. When he and his team deleted this gene from CAR-T cells engineered to recognize carcinoembryonic antigen, a cell surface protein commonly overexpressed in colon cancer, the cells effectively fought cancer in mice bearing these tumors—significantly extending their survival. However, CAR-T cells with functioning Cbl-b quickly became useless, providing little anti-tumor effect in animal models.
Poojary and his colleagues are working to understand the molecular mechanisms behind how Cbl-b causes T cell exhaustion. Once researchers better understand this mechanism, he notes, using CAR-T cells to effectively treat solid tumors could be as simple as genetically engineering them without Cbl-b.
"Our study is a major step forward in developing CAR-T cells to fight solid tumors," Poojary says. "This could overcome the limitations of some current immunotherapy strategies for cancer."
More information: Jitendra Kumar et al. Deletion of Cbl-b inhibits CD8+ T-cell exhaustion and promotes CAR T-cell function, Journal for ImmunoTherapy of Cancer (2021). DOI: 10.1136/jitc-2020-001688