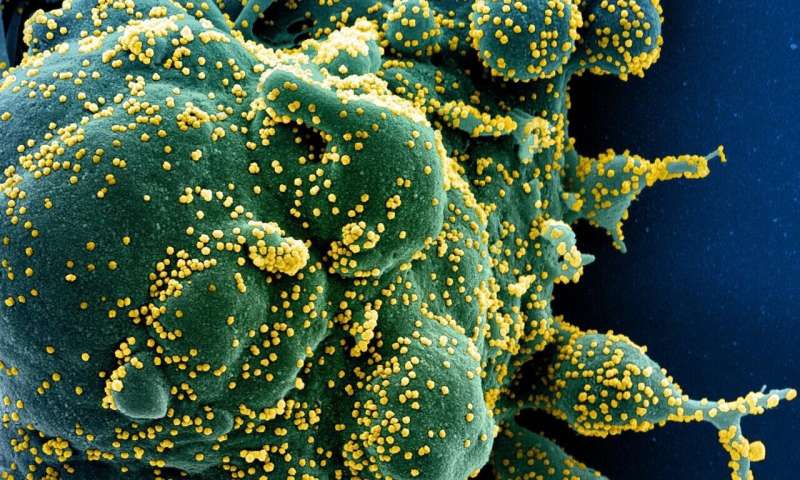
Colorized scanning electron micrograph of an apoptotic cell (green) heavily infected with SARS-COV-2 virus particles (yellow), isolated from a patient sample. Image captured at the NIAID Integrated Research Facility (IRF) in Fort Detrick, Maryland. Credit: NIH/NIAID
Johns Hopkins Medicine researchers have shown that it is possible for solid organ transplant recipients who contract COVID-19 to experience a natural immune response to SARS-CoV-2, the virus that causes the disease. In their study, published online Jan. 19, 2021, in the journal Transplantation, the researchers also suggest that measures used to provide short-term immunity against SARS-CoV-2—such as convalescent plasma (which contains antibodies from patients who have recovered from COVID-19)—may actually reduce the natural response.
"We followed 18 transplant recipients who were taking immunosuppressive medications to prevent rejection and who developed COVID-19 post-transplant," says study co-author Dorry Segev, M.D., Ph.D., the Marjory K. and Thomas Pozefsky Professor of Surgery and Epidemiology and director of the Epidemiology Research Group in Organ Transplantation at the Johns Hopkins University School of Medicine. "Our goal was to gain a deeper understanding of the immune response in these individuals, so that clinicians will be better able to treat transplant recipients who get COVID-19, prevent their disease from becoming severe and develop vaccine protocols that fit their special needs."
The study participants, all of whom were receiving immunosuppressive medication, represented a variety of organ transplants: nine kidney, five liver, one kidney and liver, two lung and one composite tissue allograft (composed of different tissue types, such as skin, muscle, bone, bone marrow, lymph nodes, nerves and tendons). The median age was 56, 56% (10) were female, 33% (six) were Black and 11% (two) were Hispanic. COVID-19 occurred at a median of six years following transplant surgery, with 89% (16) experiencing symptoms and 72% (13) requiring hospitalization. Five patients received convalescent plasma during their hospital stay. When the participants were screened for SARS-CoV-2 antibodies at a median 98 days after COVID-19 diagnosis, the researchers observed that most had antibody levels suggesting neutralizing immunity—the ability to prevent reinfection if exposed to the virus in the future.
Transplant recipients who had more severe cases of COVID-19, the researchers say, tended to have the highest antibody levels.
Interestingly, the researchers found that transplant recipients who received convalescent plasma or intravenous immunoglobulin (to reduce the risk of a serious inflammatory response) had lower natural antibody levels against the virus and, therefore, were less likely to have immunity.
"This raises the possibility that administered antibody preparations may blunt the natural formation of antibodies against SARS-CoV-2," says Jacqueline Garonzik Wang, M.D., Ph.D., associate professor of surgery at the Johns Hopkins University School of Medicine and study senior author. "Larger studies will be needed to substantiate this finding, which, if proven, would be invaluable to COVID-19 vaccine protocol development for the immunocompromised."
More information: Brian J. Boyarsky et al. Early Development and Durability of SARS-CoV-2 Antibodies Among Solid Organ Transplant Recipients, Transplantation (2021). DOI: 10.1097/TP.0000000000003637
Provided by Johns Hopkins University