Researchers discover protein that promotes chemotherapy resistance
Chemotherapy is a drug treatment that uses powerful chemicals to kill fast-growing cancer cells in the body. It is a systemic treatment where drugs travel throughout the body and destroy cancer cells that have spread (metastasized) to parts of the body far away from the original (primary) tumor. As such, chemotherapy remains the main treatment against various cancers. Thus, when cancer cells resist chemotherapeutic drugs, treatment failure results.
The resistance of cancer cells to chemotherapy is marked by changes and increased output of certain proteins. These altered proteins can help doctors to identify patients who will not respond well to chemotherapy and paves the way for the development of therapeutic intervention to 're-sensitize' their cancer cells to treatment.
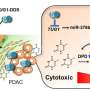
In a Nature Communications article published mid-April, Associate Professor Zhang Yongliang from NUS Yong Loo Lin School of Medicine's Immunology Translational Research Program reported the finding of one such altered protein in a study that identified how a molecule called DUSP16 plays an important role in a cancer patient's response to chemotherapeutic drugs.
Assoc Prof Zhang and his study team, in collaboration with clinical scientists including the team led by Professor Goh Boon Cher, Deputy Director of both the Cancer Science Institute of Singapore at NUS and NUS Center for Cancer Research (N2CR), found that an increased expression of DUSP16 led to resistance from cancer cells to chemotherapy in colorectal, nasopharyngeal, gastric and breast cancer. Prof Goh's team studies mainly cancers of the upper aerodigestive tracts (of the head and neck and lung), which are among the most frequent cancers, and seeks to understand these diseases.
These four cancers are among the most common and deadly ones affecting Singaporeans and Southeast Asians. Nasopharyngeal cancer has a high incidence rate in Southeast Asians, while colorectal cancer is the most frequently occurring cancer in Singapore. Breast cancer is the cancer with the highest incidence among women in Singapore and gastric cancer is among the top three cancers causing death worldwide. In addition, the fact that these four cancers manifest as solid tumors with chemotherapy being a common form of post-operative treatment meant that they made for good candidates for the study.
Analysis of head and neck cancer patients, and breast cancer patients showed that those with higher DUSP16 expression in their cancer cells lived for significantly shorter periods compared to patients with lower levels of DUSP16. DUSP16 expression can thus be used as a biomarker for sensitivity of cancer patients to chemotherapy, which will be important for clinicians seeking to design suitable treatment, said Assoc Prof Zhang. This molecule could also be targeted for the development of new therapies to improve the success of chemotherapy treatment. While this discovery is not only relevant to these four types of cancer, more research would be needed to examine other cancer types.
The study also found that chemotherapy drugs are a factor in the increased expression of DUSP16. This means that once chemotherapy begins, the expression of DUSP16 will increase in patients, Assoc Prof Zhang added. In addition, other factors such as stress or infections have also caused increased expression of DUSP16.
While there are no alternative treatments that might be effective in cancer patients who test positive for the increased expression of DUSP16, Assoc Prof Zhang and his team are planning to conduct further research to identify molecules and drugs that can reduce DUSP16 levels in patients.
The NUS Medicine Immunology Translational Research Program aims to understand the role of the immune system in health and diseases. The program strives to enable the discovery and development of more effective immunotherapy, new treatment guidelines and diagnostic tests for patients with disease-specific problems such as autoimmune and airway diseases, cancer, chronic inflammation, infections and organ/ tissue transplantation. These goals are to be achieved by fostering collaborative research and advancing latest technologies to probe immunological mechanisms, and enhancing infrastructure for clinical translation.
More information: Heng Boon Low et al, DUSP16 promotes cancer chemoresistance through regulation of mitochondria-mediated cell death, Nature Communications (2021). DOI: 10.1038/s41467-021-22638-7