Study finds mechanism leading to herceptin resistance and pharmaceutical approach to reverse it
Research conducted by an international team of scientists discovered a mechanism that leads to Herceptin resistance, representing a significant clinical obstacle to successfully treating HER2-positive breast cancer. They also identified a new approach to potentially overcome it. The work is published online in Nature Communications.
"This work attempts to understand why some HER2-positive breast cancer patients do not benefit from treatment with Herceptin, which is a generally effective HER2-targeted therapy," explains Bolin Liu, MD, Professor of Genetics at LSU Health New Orleans' School of Medicine and Stanley S. Scott Cancer Center.
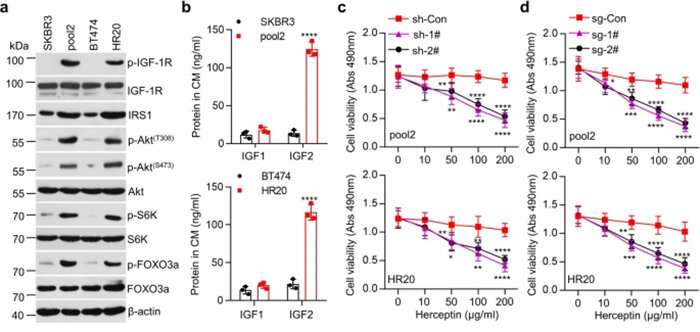
The researchers found increased signaling by IGF2/IRS1 (genes involved in regulating cell proliferation, growth, migration, differentiation and survival) in the HER2-positive breast cancer cells poorly responding to Herceptin. Further studies showed that disruption of a negative feedback loop formed by an important protein, FOXO3a, and several miRNAs that are controlled by FOXO3a causes abnormal activation of the IGF2/IRS1 signal, thereby leading to Herceptin resistance.
"Resistance to Herceptin frequently occurs and currently represents a major clinical challenge for successful treatment of HER2-positive breast cancer," notes Dr. Liu. "Data presented in the study not only improve our understanding of the molecular mechanism through which IGF-1R signaling activation leads to Herceptin resistance, but also promote identification of precision therapies to reverse the resistance phenotype."
The researchers write, "Breast cancer is the leading cause of cancer-related deaths in women worldwide. HER2-positive breast cancer is defined as a breast cancer subtype with amplified and/or overexpressed HER2 (or erbB2) gene. Amplification/overexpression of HER2 is observed in approximately 20-25% of breast cancers and is significantly associated with poor prognosis in breast cancer patients. Herceptin (or trastuzumab), a humanized anti-HER2 monoclonal antibody (Ab), is an effective HER2-targeted therapy against early and metastatic HER2-positive breast cancers. It has dramatically improved the survival of breast cancer patients with HER2-positive tumors, but not all HER2-positive breast cancers respond to Herceptin-based regimens. To date, we lack validated biomarkers predictive for Herceptin response."
"Our results may provide new avenues to identify useful biomarkers predictive for Herceptin efficacy and facilitate the development of novel approaches to enhance HER2-targeted therapy, thereby improving the survival of refractory breast cancer patients," Dr. Liu concludes.
More information: Liyun Luo et al, Disruption of FOXO3a-miRNA feedback inhibition of IGF2/IGF-1R/IRS1 signaling confers Herceptin resistance in HER2-positive breast cancer, Nature Communications (2021). DOI: 10.1038/s41467-021-23052-9