Statins may be effective treatment for patients with ulcerative colitis
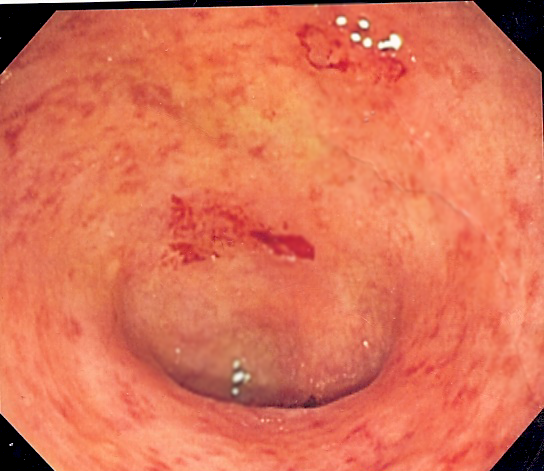
There may be good news for the nearly 1 million people battling ulcerative colitis, a type of inflammatory bowel condition with no real cure: Statins, a commonly prescribed cholesterol-lowering drug, seem to be an effective, if unexpected, treatment for the condition, according to a new Stanford Medicine study.
Currently, the only lines of defense against ulcerative colitis are anti-inflammatory drugs, which don't always work, and a colectomy, the surgical removal of part or all of the colon. Discovering another option is significant, said Purvesh Khatri, Ph.D., associate professor of medicine and of biomedical data science, who led the research.
"About 30% of ulcerative colitis patients eventually have to undergo a colectomy as a last resort. It's a drastic measure; you're removing part of your body," said Khatri. "So we thought, 'Can we use available data to see whether drugs that are already approved by the FDA can be repurposed to better treat these patients?'"
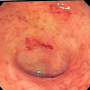
Ulcerative colitis causes inflammation and ulcers in the bowel, leaving patients vulnerable to an array of unpleasant symptoms, including abdominal pain, blood in the stool, constipation and fatigue. The condition, while not life threatening, can be severely debilitating, especially if anti-inflammatory medications don't work.
By tapping into publicly available datasets of anonymized patient health information, including genomic and prescription data, Khatri and his team tracked down a connection between a handful of drugs and decreased symptoms of ulcerative colitis. As it turned out, atorvastatin, sold under the brand name Lipitor, was one of the top performers, significantly decreasing the rate of surgical treatment for ulcerative colitis, the need for anti-inflammatory medication and hospitalization rates.
A paper describing the study will be published Sept. 16 in the Journal of the American Medical Informatics Association. Khatri is the senior author. Graduate students Lawrence Bai and Madeline Scott are co-lead authors.
Analyzing genes and drugs' effects on them
Khatri and his team began their research by analyzing publicly available genomic data from hundreds of patients with ulcerative colitis who had undergone a colon biopsy, a somewhat common practice that helps doctors diagnose the disease and its severity. Specifically, Khatri and his team were looking for certain genomic "signatures," or patterns of gene activity, that seemed to persist in most patients with the condition.
"We looked at national and international data, and we found a disease signature that was robust across all the datasets irrespective of whether the patient was experiencing a flare in disease," Khatri said.
From there, it was matter of identifying how certain drugs affected the gene activity associated with ulcerative colitis. Khatri turned to data from previously conducted lab studies in cells that showed how certain drugs changed the activity of genes. The idea was to find the drugs that seemed to reverse the gene signature associated with ulcerative colitis. For instance, if patients with ulcerative colitis had a dip in the activity of gene A and B, the team looked for drugs that increased activity in those genes. They looked only at drugs that had been approved by the Food and Drug Administration so that, if they found a drug that worked, it could be rolled out to patients sooner.
Statins emerge
After cross-referencing the genomic and experimental sets of data, the team identified three drugs that effectively reversed the gene signature of ulcerative colitis. "The first two were chemotherapy drugs, which of course you wouldn't prescribe to someone due to serious side effects, but the third was a statin. Statins are generally safe enough that some doctors joke they should be put in the water," Khatri said.
The next step would usually be to set up a clinical trial. But, ever the data enthusiast, Khatri took a different approach. Statins are among the most commonly prescribed drugs in the United States, so it seemed reasonable to think that a relatively large number of patients with ulcerative colitis might also be taking statins to help manage their cholesterol. So, instead of turning to a clinical trial, the team turned to data from electronic health records. "We were able to see if they had ulcerative colitis, if they were on statins and whether they'd needed a colectomy," Khatri said.
People with ulcerative colitis who were taking statins, regardless of their age, had about a 50% decrease in colectomy rates and were less likely to be hospitalized. In addition, ulcerative colitis patients who were taking statins were prescribed other anti-inflammatory medications at a lower rate.
While it's not entirely known how statins quell symptoms of the disease, Khatri said they are known to have some sort of general anti-inflammatory capacity.
"At this point, one could argue that this data shows a strong enough connection to start prescribing statins for ulcerative colitis," Khatri said. "I think we're almost there. We need to validate the effects a bit more stringently before moving it into the clinic."
The other benefit of the study, Khatri said, is that it provides a framework for how to suss out drugs that are already in circulation and repurpose them to treat other diseases. The system, he said, is rife with potential, particularly for autoimmune diseases.
Other Stanford co-authors are graduate students Ethan Steinberg and Laurynas Kalesinskas; professor of medicine Aida Habtezion, MD; and professor of medicine and of biomedical data science Nigam Shah, MD, Ph.D.