The role of macrophages in the progression from acute kidney injury to chronic kidney disease
Acute kidney injury (AKI) is a condition in which kidneys are unable to filter waste from the blood effectively, leading to various health complications. Numerous studies have demonstrated that acute kidney injury (AKI) subsequently leads to long-term renal damage and progresses into chronic kidney disease (CKD)—a more severe form of kidney failure. The transition from AKI to CKD is dependent on various factors, such as sepsis, type of surgery, and the presence of cardiovascular diseases.
At present, the exact mechanisms underlying this multifactorial transition are unclear. Unraveling these mechanisms can contribute to the development of therapeutic strategies to prevent the AKI-CKD transition. Currently, it is known that macrophages, which are a type of immune cell, play a key role in the transition from AKI to CKD.
To explore the role of macrophages further, a team of researchers led by Dr. Xiaoming Meng from Anhui Medical University in China, wrote a review article highlighting the impact of different macrophage subtypes on the transition from AKI to CKD. This article, which was published the Chinese Medical Journal, also explored the potential of macrophage targeted therapy in the prevention of the AKI-CKD transition.
The source from which a macrophage is derived affects its phenotype and function. In fact, macrophages can evolve into multiple phenotypes, each of which takes up a different role in regulating kidney failure and repair. For example, resident macrophages, which are specific to the kidney tissue, are involved in anti-inflammatory processes during kidney repair, while circulating macrophages, which are derived from blood monocytes, play a pro-inflammatory role upon migrating to the site of injury.
Generally, macrophages are categorized into two types: M1 and M2. A few studies have suggested that M1 macrophages, which are pro-inflammatory, play a role in certain early processes associated with AKI development. On the other hand, M2 macrophages have been found to reduce the inflammation and fibrosis associated with AKIs.
How do pro-inflammatory macrophages contribute to CKD? Dr. Meng says that "renal injury which leads to CKD is enhanced by pro-inflammatory macrophages. These macrophages accelerate renal inflammation via the release of several pro-inflammatory cytokines and chemokines or by triggering abnormal wound healing processes, which eventually lead to renal fibrosis."
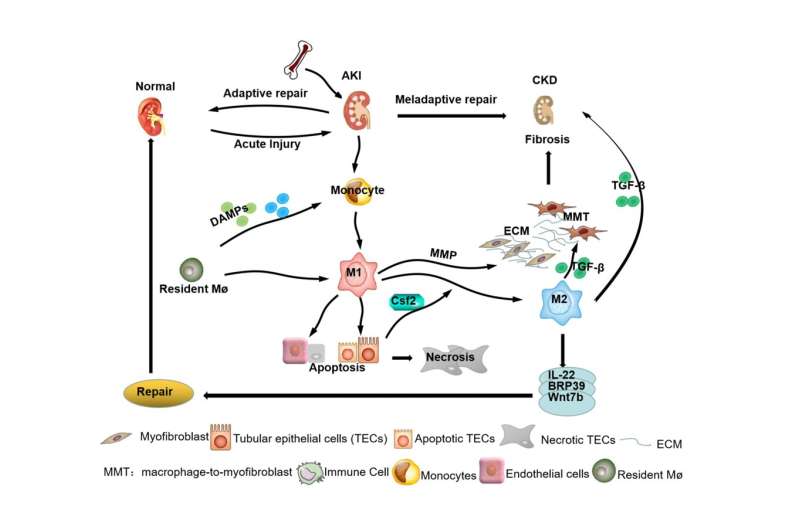
The unique nature of macrophages allows them to change their phenotype from M1 to M2 in response to kidney injury—a process known as polarization. Macrophages can also alter the kidney microenvironment through interactions with endothelial cells, immune cells, fibroblasts, and tubular epithelial cells (TECs). For example, macrophages infiltrating the kidney in response to injury promote TEC injury and death, which ultimately blocks the AKI-CKD transition brought about by the TECs.
In sepsis-induced AKI, Csf2, which is a cytokine secreted by injured TECs, promotes the transition of M1 macrophages to M2 macrophages. Interestingly, certain M2 macrophages that express CD206 and/or CD163 receptors contribute to subclinical inflammation, tubular injury, and the progression of renal fibrosis—a stark contrast from their usual anti-inflammatory behavior. Moreover, in case of extreme inflammation, M2 macrophages adopt a 'pro-fibrotic phenotype' wherein they activate myofibroblasts, which are cells involved in wound contraction and healing.
"Unexpectedly, we discovered that macrophages can directly trans-differentiate into myofibroblasts, via a process known as macrophage-myofibroblast transition (MMT). These newly formed myofibroblasts increase renal fibrosis, which eventually leads to renal failure," stated Dr. Meng. At present, the exact role of MMT in the AKI-CKD transition is unclear.
The article also discusses three signaling pathways that contribute to the AKI to CKD transition, which include the Notch signaling pathway, the TGF-β/Smad signaling pathway, and the Wnt/β-catenin signaling pathway. "Targeting the pathways that regulate macrophage and MMT activation or modification of macrophage phenotypes can be a promising therapeutic approach for kidney diseases, by blocking the AKI to CKD transition," says Dr. Meng, while discussing how the AKI-CKD transition can be prevented.
Therapeutic strategies that interfere with the activation and pathogenic role of macrophages in this transition have been widely studied. The article highlights the role of molecules known as clodronate liposomes, which can deplete macrophages and reduce the extent of renal fibrosis. Altering the activation of macrophages and blocking factors that they interact with can also prevent renal fibrosis and subsequent failure.
Moreover, treatment with a compound known as quercetin has been shown to block macrophage infiltration and M2 polarization. Additionally, a receptor known as colony stimulating factor (CSF)-1 influences the proliferation, differentiation, and survival of macrophages. Blocking the gene that codes for this receptor can lead to an inhibition of macrophage proliferation in the kidneys. Moreover, a molecule known as vorapaxar has been reported to suppress macrophages by blocking pathways that are involved in the AKI to CKD transition.
More information: Xiaoming Meng et al, Driving role of macrophages in transition from acute kidney injury to chronic kidney disease, Chinese Medical Journal (2022). DOI: 10.1097/CM9.0000000000002100