Limiting food intake to daytime shows promising beneficial metabolic effects in adults with type 2 diabetes

A new study published in Diabetologia (the journal of the European Association for the Study of Diabetes [EASD]) finds that following a time-restricted eating (TRE) protocol, which limits food intake to a maximum 10-hour time window, shows promising beneficial metabolic effects in adults with type 2 diabetes (T2D). The research was conducted by Prof. Patrick Schrauwen, Charlotte Andriessen and colleagues at NUTRIM School of Nutrition and Translational Research in Metabolism, Maastricht University Medical Center, the Netherlands.
Our modern 24-hour society is characterized by endless food availability and disrupted day-night rhythm brought on by irregular sleep-activity patterns and frequent exposure to artificial light sources. In Western nations, people also tend to spread their daily food intake over a minimum of 14 hours, which is likely to result in the absence of a true, nocturnal fasting state. These factors all contribute to the development of T2D, which has become one of the most common metabolic diseases globally, estimated by the World Health Organization to cause more than 1.5 million deaths per year.
TRE is a novel strategy for improving metabolic health and is intended to counteract the detrimental effects of eating throughout the day by limiting the duration of food intake (typically 12 hours or less) and restore the cycle of daytime eating and prolonged fasting during the evening and night.
Previous studies show that TRE leads to promising metabolic changes in people with overweight or obesity, including increased fat burning, decreased blood sugar levels and improved insulin sensitivity; but these effects have not been studied in detail. Moreover, while these results are promising, these studies used extremely short eating time windows (6-8 hours) and highly controlled study settings, making such protocols difficult to implement in daily life. TRE is sometimes accompanied by unintended weight loss, which would be expected to increase metabolic health, but such improvements have also been reported in the absence of weight loss, indicating that additional mechanisms are involved in how restricted eating influences metabolism.
Individuals with impaired metabolic health experience alterations in the rhythms of metabolic processes, compared to healthy, lean individuals and the authors hypothesize that a disturbed feed-fasting cycle contributes to these impairments in metabolic rhythms. They suggest that restricting food intake to daytime only and extending the length of the nocturnal fast may have beneficial effects on metabolic health.
The researchers recruited 14 individuals with T2D for the study, aged between 50 and 75 years (7 male, 7 female, average age 67.5 years) and body mass index (BMI) ≥25 kg/m2. The study consisted of two 3-week intervention periods: TRE and control (CON), separated by a wash-out period of at least 4 weeks. At the start of each intervention, participants had their body weight measured and were fitted with a continuous glucose monitoring (CGM) device, which measured their blood sugar level every 15 minutes. They were instructed to keep to their normal sleep patterns and physical activity, and to maintain a stable weight. A food and sleep diary completed during the first intervention was used to ensure that diet during the second period was similar in both quantity and quality.
During TRE participants were instructed to consume their normal diet within a 10-hour window during the daytime, and to complete their food intake by no later than 6:00 in the evening. Outside this time window they were permitted to drink water, plain tea, or black coffee, and zero-calorie soft drinks were also allowed during the evening if consumed in moderation. During CON, volunteers were only required to spread their normal food intake over at least 14 hours, with no other restrictions.
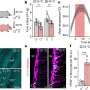
The eating window for TRE averaged 9.1 hours compared to 13.4 hours in CON, while sleep-wake patterns were similar in each case, with mean sleep durations of 8.1 hours and 8.0 hours respectively. Mean body mass was comparable at the start of both TRE and CON, and although volunteers were instructed to remain weight-stable, a small but statistically significant weight loss occurred in response to TRE but not CON.
TRE was found to decrease 24-hour glucose levels, primarily as a result of lower nocturnal blood sugar, and the average time spent with blood glucose in the normal range increased to 15.1 hours versus 12.2 hours during the CON phase. Morning fasting glucose was consistently lower among the TRE group than those on the control diet, which might have been the result of lasting changes in nocturnal glucose control. Time spent in hypoglycemia (low blood sugar) was not significantly increased by TRE and no serious adverse effects were reported resulting from the protocol, demonstrating that an eating window of approximately 10 hours is a safe and effective lifestyle intervention for adults with T2D.
Approximately half-way through each intervention, liver glycogen levels were assessed in the morning following the 10-hour or 14-hour nighttime fast period, and were measured again at the end of each study period after an 11-hour fast for both TRE and CON. In both cases, liver glycogen did not differ significantly between TRE and CON and an analysis of liver fats showed no difference in their quantity or composition between interventions.
Unlike a previous study into TRE, this one did not show that the protocol had any effect on insulin sensitivity. However, the earlier research had used a much shorter 6-hour food intake window with the last meal being consumed at 3:00 in the afternoon. This resulted in a longer fasting period, which may have been more effective but was felt to be unrealistic to incorporate into the lifestyle of most adults with T2D. The team advises, "Future studies will be needed to reveal whether the duration of the fasting period is indeed crucial in determining positive effects on insulin sensitivity."
The authors say, "Mechanisms underlying the improvement in glucose regulation upon TRE remain unclear. Our results show that TRE did not improve peripheral and liver insulin sensitivity, skeletal muscle mitochondrial function, energy metabolism or liver fat content, all of which are known to be affected in T2D." They propose that the mechanisms involved in the effects and their implications should be investigated further, with particular focus on studying nocturnal glucose metabolism in more detail.
Limitations of this research include its relatively short duration and that some but not all participants were on glucose-lowering medication, which may have caused TRE to have less effect. Despite this, a 3-week intervention period has been found to be long enough to affect the variables being analyzed, and the authors highlight that only recruiting volunteers who were not on medication would reduce the study's relevance to the general T2D population.
The authors conclude, "A daytime 10 hour TRE regimen for 3 weeks decreases glucose levels and prolongs the time spent in the normal blood sugar range in adults with T2D as compared with spreading daily food intake over at least 14 hours. These data highlight the potential benefit of TRE in T2D."
They also suggest, "Since our TRE protocol was feasible and safe, and resulted in improved 24-hour glucose levels, it would be interesting to examine the impact of 10-hour TRE on glucose regulation and insulin sensitivity in type 2 diabetes in the long term to address the clinical relevance of TRE."
More information: Three weeks of time-restricted eating improves glucose homeostasis in adults with type 2 diabetes but does not improve insulin sensitivity: a randomised crossover trial, Diabetologia (2022).