Exercise training program improves cardiorespiratory fitness in adults with chronic kidney disease

A randomized trial recently published in the American Journal of Kidney Diseases (AJKD) found that a 12-month program of in-center aerobic and resistance exercise program improved physical functioning among adults 55 years and older with CKD stages G3b-4 and a high level of medical comorbidities.
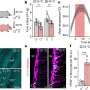
Among adults ≥55 years with CKD stages G3b-4 and with a high level of comorbidity, a 12-month program of in-center aerobic and resistance exercise training was safe and feasible, and compared to health education control was associated with improvements in submaximal gait and mobility, as quantified by validated objective measure of physical performance. The exercise program also improved measured aerobic exercise capacity after 6 months compared to the health education group, although this difference was not sustained at 12 months.
In contrast, there was no impact on secondary outcomes of cardiovascular risk, including blood pressure, lipids, kidney function, and body mass index when compared to health education control. The latter finding may be explained by insufficient statistical power, a true absence of effect of the exercise training program on these risk factors, or (for blood pressure and glycemia) post-randomization changes in medical therapy. Compared to trials of similar interventions, adherence to the thrice weekly exercise regimen was moderately high, especially for the initial 6-month intervention period, though with a decline for the second 6-month period despite the option for at-home exercise once weekly.
In contrast to many prior exercise studies in CKD patients, this trial included an active comparator group, which provided similar (albeit less intensive) group social interaction to that experienced by participants in the supervised exercise training. Therefore, the observed differences in physical function are more likely to represent true physiologic effects of exercise training and are less likely to be explained by greater motivation among the exercise group from greater interactions with healthcare providers and other patients.
Furthermore, the exercise intensity goal was individualized for each subject, as a fixed range of each participant's heart rate reserve. This accounted for inter-individual differences in maximal heart rate due to factors such as chronotropic incompetence and pharmacological beta-blockade. Study participants received 12 months of exercise training, testing the durability of the benefits of such interventions, in contrast to the 2-6 months of training in the majority of prior studies in kidney disease patients.
Finally, the study population included a racially diverse CKD population with a high burden of comorbidity including chronic cardiovascular diseases, reflective of the characteristics of many CKD patients in the U.S., thus enhancing the external validity of the study results.
More information: Daniel E. Weiner et al, Effect of Long-term Exercise Training on Physical Performance and Cardiorespiratory Function in Adults With CKD: A Randomized Controlled Trial, American Journal of Kidney Diseases (2022). DOI: 10.1053/j.ajkd.2022.06.008