Using music to counter delirium in mechanically ventilated older adults in the ICU
Regenstrief Institute, Indiana University School of Medicine and Mayo Clinic researcher-clinicians are conducting a multi-site study to establish that music intervention can reduce the likelihood of critically ill, mechanically ventilated older adults in a hospital intensive care unit (ICU) developing delirium and can also improve their post-ICU brain health. The study is one of the first to measure dosage of music exposure as the researchers continue their pioneering exploration of the potential of music to decrease or even prevent delirium.
One million adults in the U.S. receive mechanical ventilation in a hospital ICU annually. While in the ICU, as many as 80 percent of these individuals experience delirium, a syndrome of acute brain dysfunction. Delirium predisposes patients to longer ICU and hospital stays and increased risk of death. Delirium is also associated with long-term complications including cognitive impairment and dementia.
Individuals with delirium experience a sudden change in mental status, often acting confused, disoriented or distracted. Individuals experiencing delirium could become overactive, agitated and restless. They may have rapid emotional changes, have trouble concentrating and often experience hallucinations or anxiety.
"No effective drug for delirium exists so there is great need for nonpharmacological therapies to prevent or manage delirium," said study co-principal investigator Babar Khan, M.D., M.S., of Regenstrief Institute and IU School of Medicine. "We are conducting this study to firmly establish that music reduces delirium in ICU patients who are mechanically ventilated, with the goal of music listening as anti-delirium therapy becoming the standard of care for patients in ICUs across the country."
A past president of the American Delirium Society, Dr. Khan is the developer of the CAM-ICU-7, an easy-to-use delirium severity evaluation tool. CAM-ICU-7 is being used in the study to score delirium on a zero (no delirium) to 7 (severe) scale to provide objectivity to brain failure assessment. This information is vital not only for current and future brain health management by clinicians, but also for use in future clinical studies by researchers. He has also developed the post-critical care model for ICU survivors.
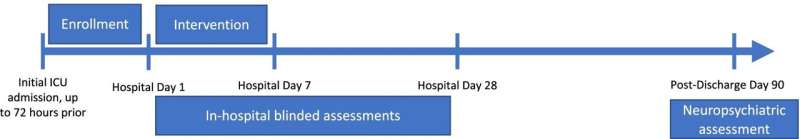
In the current music to decrease delirium study, 160 mechanically ventilated adults, 50 years of age or older, are being randomized to one of two groups within 72 hours of ICU admission. Those in the music arm of the study receive a dose of slow tempo (60 to 80 beats per minute) instrumental music through noise-canceling headphones for one hour twice daily for seven days. The other arm receives a placebo consisting of a silent audio track administered in the same manner and duration. In addition to twice daily delirium assessments, pain and anxiety will be evaluated daily.
The primary outcome of improving delirium is measured by the number of days patients are alive, not comatose and free of delirium during the seven days of exposure to music or silence.
For both groups a specially designed computer application (app), which has been pilot tested by the Regenstrief, IU and Mayo researchers, tracks the length and frequency of listening sessions. For those in the music arm of the study, the app also gathers data about music selection from an extensive playlist.
Three months after hospital discharge, the effects of exposure to music on cognition, as measured by memory, attention, information processing, speed and executive cognitive function of recipients of music versus silent track will be assessed as well as study participants' mood and anxiety.
"As a secondary outcome of the study, we are exploring the downstream effects of relaxing, slow-tempo music on brain health outcomes that matter to ICU survivors," said study co-investigator Sikandar Khan, D.O. He is co-program director of the COVID-19 Recovery Program for Older Adults at Regenstrief Institute and director of the Indiana University Health Intensive Care Unit (ICU) Survivor Center.
The research was published in Trials.
More information: Sarah Seyffert et al, Decreasing delirium through music listening (DDM) in critically ill, mechanically ventilated older adults in the intensive care unit: a two-arm, parallel-group, randomized clinical trial, Trials (2022). DOI: 10.1186/s13063-022-06448-w