Scientists identify promising therapeutic target for incurable brain cancer
Researchers at VCU Massey Cancer Center discovered a cellular partnership that drives the growth of deadly brain tumors and could potentially serve as a novel target for disease treatment.
Gliomas are any cancer that start in the glial cells of the nervous system and account for nearly one-third of all brain tumors. The most aggressive type of glioma is called glioblastoma (GBM), which affects the brain and is virtually incurable.
A new study—published this week in Science Advances — uncovered a previously unknown genetic process that could inform the development of novel treatment options for GBM.
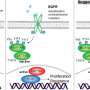
The epidermal growth factor receptor (EGFR) signaling pathway has previously been shown to be highly active in the majority of GBMs. Signaling pathways are like a cellular chain-of-command through which a string of proteins is triggered in a sequence to stimulate a specific cell function. The irregular activation of certain pathways can often lead to the development of disease, including cancer.
"Dysregulated EGFR signaling is associated with worse outcomes and increased resistance to traditional therapies in GBM patients; thus, targeting EGFR has been regarded as a promising therapeutic strategy," said study author Suyun Huang, M.D., Ph.D., the Paul M. Corman, M.D., Chair in Cancer Research and member of the Cancer Biology research program at Massey. "However, the underlying cellular processes through which EGFR contributes to tumor growth are largely unknown."
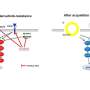
Previous research indicates that the EGFR pathway obstructs a natural process through which cells stop dividing called senescence, a mechanism that is critical in stunting the growth and spread of cancer cells. Blocking the function of the EGFR pathway promotes senescence and helps prohibit tumor growth.
Through this new study, Huang and her research team demonstrated that a specific protein called ubiquitin-specific protease 16 (USP16) regulates senescence and mitigates the growth of glioma cells. They also identified a separate strand of long non-coding RNA—molecules that control gene activity—called lncEPAT that is activated through EGFR and is highly functional in GBM. Huang's findings suggest that lncEPAT acts as a genetic moderator allowing for EGFR to escape the antitumor role of USP16 and fuel cancer progression.
In preclinical models, Huang found that the depletion of lncEPAT increased the activity of USP16 and stifled GBM cell growth.
"We have compelling evidence that lncEPAT's cancer-driving function in GBM is dependent on the inactivation of the USP16 protein," said Huang, professor in the Department of Human and Molecular Genetics at the VCU School of Medicine. "EGFR-induced, overexpressed lncEPAT provides a promising new target for pro-senescence treatment for GBM."
Huang collaborated on this study with Massey research members Jinze Liu, Ph.D., and Hengbin Wang, Ph.D.; Runping Fang, Ph.D., Linlin Li, Ph.D., Peng Li, M.D., and Hope Richard, M.D., Ph.D., of the VCU School of Medicine; Yiwen Chen, Ph.D., Li Ma, Ph.D., Longqiang Wang, Ph.D., Yanjun Wei, Ph.D., and Aldong Zhou, Ph.D., of MD Anderson Cancer Center; Feng Liu, Ph.D., of the Ludwig Institute for Cancer Research; and Sicong Zhang, Ph.D., of The Rockefeller University.
More information: Linlin Li et al, Critical Role of LncEPAT in Coupling Dysregulated EGFR Pathway and Histone H2A Deubiquitination during Glioblastoma Tumorigenesis, Science Advances (2022). DOI: 10.1126/sciadv.abn2571. www.science.org/doi/10.1126/sciadv.abn2571